Aortic Regurgitation (Valve Insufficiency)
What is aortic regurgitation?
Aortic regurgitation is a condition where blood flows backward back from the aorta into the heart when the ventricles relax. Backward flow (regurgitation) is prevented by the aortic valve. In other words it ensures blood only flows in one direction – from the left ventricle into the aorta and then onwards to the rest of the body. Aortic regurgitation is a consequence of dysfunction of this aortic valve or an abnormality at the aortic root (where the aorta emerges from the heart known as the ascending aorta). This backward flow disrupts the heart’s ability to pump blood normally and can ultimately weaken the heart over the long term.
How common is aortic regurgitation?
Since aortic regurgitation tends to develop gradually in most people, it may only cause a minor disruption and the compensatory mechanism the heart can cater for it appropriately. Due to this fact, there may be no signs and symptoms. Therefore it is difficult estimate the incidence of mild aortic regurgitation as it can remain undiagnosed for years, decades or even throughout life. However, severe aortic regurgitation causes serious heat dysfunction that requires medical or surgical intervention.
It is believed that aortic regurgitation may affect as much as 30% of people in th 40 to 60 year age group and as many as 10% of these patients have severe aortic regurgitation that will require medical attention. However, severe aortic regurgitation is not common in people younger than 70 years of age. Men are about one and a half times more likely to suffer with aortic regurgitation than women.
What happens in aortic regurgitation?
Left side of the heart
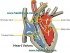
Normally oxygen rich blood is forced out of the left ventricle, into the aorta and is then distributed throughout the body. When the ventricles relax, it fills with more oxygen-rich blood from the left atrium. Once it is filled completely, the left ventricle contracts again thereby pushing blood out of the aorta. In this way oxygen-rich blood just received from the lungs can be distributed to all the cells and tissues of the body. This process is essential for life as oxygen is used by every cell for life sustaining processes.
Heart valves prevent regurgitation
To prevent backward flow in the heart, there are valves. One such valve is the aortic valve which lies between the origin of the aorta and the left ventricle. It is a ‘one-way’ valve ensuring that blood flows out of the heart and into the aorta. As the heart relaxes, the blood in the aorta can flow backwards by the aortic valve prevents this. It has leaflets, which when filled with blood, blocks the channel between the left ventricle and aorta. This allows the left ventricle to fill only with blood from the left atrium.
Backward flow of blood into the left heart
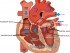
The term ‘aortic regurgitation’ is often used interchangeably with aortic valve insufficiency. This is based on the fact that backward flow is a result of the aortic valve not functioning properly thereby not closing the channel between the left ventricle and aorta completely as it should. However, abnormalities in the ascending aorta can also compromise aortic valve functioning, despite the valve being normal in structure. Should the left ventricle fill partially with aortic blood, then it is not pushing out as much blood as it should since blood that it has already pushed out has now returned. Ultimately this means that there is less oxygen-rich blood being circulated through the body. The heart tries to compensate by enlarging the left ventricle and thereby increasing the volume it can receive and push out.
Effects of regurgitation
Over time left ventricular dilatation (enlargement) has several adverse effects on heart function. The now enlarged heart that has to pump harder may also not receive sufficient oxygen for its needs (ischemia). The rate and rhythm is compromised and with the host of other complications, it can eventually lead to heart failure in severe cases. However, in mild cases the heart’s moderate compensatory measures may not affect the health and functioning of the heart as adversely. A person can live life normally and may not even known that they have aortic regurgitation until it is routinely diagnosed in the course of investigations for other heart problems.
Signs and Symptoms
As previously mentioned, mild aortic regurgitation is often asymptomatic. Aortic regurgitation can be acute or chronic. Acute aortic regurgitation starts up suddenly and presents with intense symptoms. Chronic aortic regurgitation develops gradually over years and decades and the symptoms become worse of time. The symptoms of acute and chronic aortic regurgitation are largely the same although the pattern of development may vary. These symptoms include :
- Shortness of breath (dyspnea) that is more prominent when a person is lying down or during periods of strenuous activity.
- Weakness with exertion.
- Easily fatigued.
- Dizziness and sometimes fainting spells.
- Tightness or pain in the chest, sometimes mistaken for heart attack pain.
- Irregular heart rhythm (arrhythmia)
- Throbbing or fluttering heart sensation (palpitations)
- Abnormal or extra heart sound (murmur)
As the condition worsens and the heart function declines, swelling of the ankles and feet becomes evident.
Causes and Risk Factors
The causes of aortic regurgitation can be divided into acute or chronic. The acute type is considered to be more serious because it arises suddenly and the heart does not have sufficient time to adapt.
Acute
- Infective endocarditis
- Aortic dissection
- Rupture of a valve that is abnormal from birth
- Injury to the chest associated with blunt trauma
- Surgical procedures like aortic balloon valvotomy
- Prosthetic heart valve malfunction
Chronic
- Age-related degeneration of the aortic valve
- Congenital heart defect (from birth) involving the aortic valve
- Rheumatic fever
- Marfan syndrome
- Ankylosing spondylitis
- Rheumatoid arthritis
- Systemic lupus erythematosus (SLE)
Tests and Diagnosis
A clinical examination, along with the symptoms reported by the patient and medical history may lead to a differential diagnosis of aortic regurgitation. Different clinical signs such as a visible beating of the pulses at some sites and abnormals sounds heard over pulses (bruits) are characteristic of left ventricular hypertrophy. More definitive diagnostic tests include :
- Standard chest x-ray is the easiest imaging study to conduct immediately.
- Echocardiogram where ultrasounds waves are used to form images of the heart. Three types of echocardiogram are useful – Doppler, transesophageal or transthoracic echocardiogram.
- Cardiac computed tomography (CT) scan and magnetic resonance imaging (MRI).
Treatment and Surgery
Although medication may be useful in treating and managing some of the complications of aortic regurgitation, the condition itself needs to be corrected surgically. Vasodilators are used to relax the arteries in the body thereby reducing the workload on the left ventricle. It can be used in both acute and chronic aortic regurgitation until the condition eases or resolves in acute cases, or can eventually be surgically in both acute and chronic cases. Vasodilators also help to ease the severity of the symptoms.
There are two procedures that need to be considered for severe aortic regurgitation – aortic valve repair or replacement.
Valve Repair
Repair of the natural valves of the heart is suitable when the damage to the valve is not too severe. The natural valve is modified to function properly in a procedure known as valvuloplasty. ‘Blood thinning’ drugs (anticoagulants) are not required if the natural valve is repaired.
Valve Replacement
Replacement of the aortic valve involves the use of a mechanical (artificial prosthetic) valve or a tissue valve (bioprosthetic valve). The decision about which valves is the better choice is decided upon based on several guidelines and criteria.
- Mechanical valves which are made of metal are often preferred for its durability. However, a person needs to be on ‘blood thinners’ (anticoagulants) for life as there is a risk of blood clots forming on these valves.
- Tissue valves, or bioprosthetic valves, are sourced from pigs and sometimes cows or human transplant donors. These valves are not as durable as mechanical valves but do not require lifelong use of anticoagulants.
References :
http://emedicine.medscape.com/article/150490-overview
http://www.uptodate.com/contents/acute-aortic-regurgitation-in-adults
http://www.mayoclinic.com/health/aortic-valve-regurgitation/DS00419