Lower Gastrointestinal (Gut) Bleeding
What is lower gastrointestinal bleeding?
Lower gastrointestinal bleeding (LGIB) is loss of blood from the lower part of the gut, namely the large intestine and to a lesser extent the ileum of the short intestine. Although lower gastrointestinal bleeding is less common than upper gastrointestinal bleeding, it can lead to significant blood loss over time as many patients are not aware of the condition or do not seek medical assistance. Bleeding from the lower gut is not a disease on its own but rather a symptom of some underlying disease. It can arise with common conditions such as hemorrhoids (piles) or may be a sign of serious bowel conditions like colon cancer.
Lower Gastrointestinal Bleeding Location
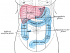
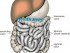
Bleeding may arise from anywhere within the the large intestine. This part of the bowel is approximately 1.5 meters (about 5 feet) long. Blood supply to the large intestine is mainly through the mesenteric arteries which are a branch of the abdominal aorta. The mesenteric veins then drain blood away. The lowest part of the colon which connects to the rectum, known as the rectosigmoid junction, is supplied by rectal arteries and veins along with the rectum itself.
Lower gastrointestinal bleeding presents with blood in the stool. If it is bright red then it is more likely to be from the lowest parts of the gut and may be severe. If it is not visible but causes the stool to be dark and tarry then it may be from higher up in the gut. There are various investigations that are needed to identify the site of the bleeding. Other symptoms are usually not helpful in identifying the site of the bleeding although it may highlight the possible cause. Bleeding is usually painless and even when pain is present, it has little significance in localizing the site of the blood loss.
Lower Gastrointestinal Bleeding Causes
In recent studies, the causes of lower gastrointestinal bleeding from most common to least common includes :
- Diverticulosis
- Hemorrhoids
- Inflammatory bowel disease (IBD)
- Cancers
Diverticulosis
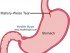
Diverticulosis is an outpouching of the bowel wall to form a sac-like protrusion. The weakened part of the bowel wall may develop tears with chronic injury and infection (diverticulitis). Diverticulosis is a fairly common bowel condition in seniors but often remains asymptomatic and goes by unnoticed for long periods of time.
Hemorrhoids
Hemorrhoids, commonly known as piles, are swollen and at times inflamed veins in the rectum. It is one of the common consequences of constipation where a person strains hard to pass out stool. Hemorrhoids may also occur with chronic diarrhea due to prolonged sitting on the toilet. Hemorrhoids are among the more common reasons that younger people find fresh red blood upon wiping after a bowel movement.
Inflammatory bowel disease
Inflammatory bowel disease (IBD) is a chronic condition where the bowel walls are inflamed usually due to an autoimmune mechanism. The inflammation becomes intense during acute episodes. There are two types of IBD – ulcerative colitis and Crohn’s disease. Lower gastrointestinal bleeding is more likely to occur with ulcerative colitis. Diarrhea is one of the main symptoms of IBD and sometimes bleeding may be from hemorrhoids and not from the underlying bowel disease itself.
Cancers
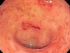
There are various different types of cancers that may affect the colon and rectum. An adenocarcinoma is the most common and gradually causes erosions and ulcerations of the bowel wall. Bleeding may also occur with a polyp but is less likely than it is with cancer. Bleeding from colorectal carcinoma is low grade and not often detected in the early stages since it does not often cause overt symptoms.
Other causes
There are a number of other causes that may also cause lower gastrointestinal bleeding. This includes :
- Infectious colitis and other causes of colitis apart from IBD
- Arteriovenous malformations
- Anal fistula
- Bleeding disorders
Lower Gastrointestinal Bleeding Symptoms
The symptoms of lower gastrointestinal bleeding can vary to some degree with the underlying cause. The main symptom that is present in every case is microscopic or gross blood in the stool.
Blood in the stool
The presentation of blood in the stool is based on the degree of the blood loss and the location. When there is significant blood loss then the stools may have a bright red color, or this may be noticed in the toilet bowl or upon wiping. However, when there is very slight blood loss then the it is often not visible to the naked eye. Usually the appearance of blood only with wiping is more likely to be due to hemorrhoids and other symptoms such as burning and itching of the rectum must be noted.
Blood loss lower down the gut is more likely to appear bright red and “fresh”. This is known as hematochezia. However, in a patient with profuse and watery diarrhea which is blood stained, the bleeding can be from as high up as the stomach. Blood that enters the bowel higher up in the colon and is retained in the bowel for long before being passed out may cause the stool to appear dark and tarry. This is known as melena. Bleeding in the upper gut without diarrhea being present will also give the stool a dark tarry appearance.
Massive blood loss
Although a massive hemorrhage is not common in most causes of lower gastrointestinal bleeding, it needs to be considered separately as it is a very serious clinical event. The most obvious symptoms will be bleeding through the rectum with stool being totally covered with blood or sometimes bloody diarrhea.
There will be other symptoms of the circulatory system that may also be present either with massive hemorrhage or significant blood loss over a long period from even minor bleeding. This includes hypotension, weak and rapid pulse, dizziness, low urine output, dehydration and nausea. Patients need immediate medical attention in order to first be stabilized and then the source of the bleeding isolated and treated.
Other symptoms
Other abdominal and bowel symptoms are not present in the majority of gastrointestinal bleeding cases. It is more likely to be seen either with acute causes and in younger patients. The presence of these symptoms are largely dependent on the underlying cause and includes :
- Abdominal pain
- Diarrhea
- Fever
- Rectal burning and pain
It is important to note that most causes of lower gastrointestinal bleeding are painless.
Lower Gastrointestinal Bleeding Diagnosis
Firstly the presence of bleeding in the gut needs to be confirmed when it is not grossly evident. This is done with a fecal occult blood test (FOBT). A complete blood count and iron profile blood test will indicate the severity of the blood loss, possible cause and any other relevant changes associated with the underlying diseases.
Other tests that may need to be conducted include :
- Clotting profile and related tests for assessing bleeding disorders.
- Computed tomography (CT) scan
- Colonoscopy
- Barium enema
- Radionuclide scanning
Lower Gastrointestinal Bleeding Treatment
Treatment of lower gastrointestinal bleeding is dependent on many different factors. It is usually directed at the cause.
Minor bleeding
In the event of very slight bleeding where the patient is stable, various diagnostic investigations as described above are undertaken. Endoscopic investigations not only provide the benefit of identifying the exact site of the bleed but treatment can be undertaken at the same time. Sclerosing therapy may be done with heat (laser or electrical) to seal the site. Less commonly it may be done chemically. The underlying disease that has caused the bleeding needs to be identified and treated accordingly thereafter.
Major bleeding
If these is massive blood loss then a patient has to be resuscitated if necessary and stabilized. The site of the bleeding then needs to be localized. Where necessary, surgery may need to be considered to seal the site of the bleed. If it is not possible to stop the bleeding in this way then a portion of the bowel may need to be surgically removed (resection). Should there be significant bleeding but the site cannot be identified then certain drugs will be administered to reduce blood loss. This is known as vasoconstrictive therapy but cannot be continued indefinitely. Ultimately more intensive investigations need to be conducted, the site of the bleeding identified and the underlying cause treated.