Pericarditis (Inflamed Heart Lining) Symptoms, Pain and Causes
What is pericarditis?
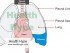
Pericarditis is the term for inflammation of the pericardium, the sac surrounding the heart and root of the great blood vessels. This protective sac has two layers, between which is a small amount of pericardial fluid that helps with lubrication. Pericarditis may arise as a result of an infection, autoimmune conditions, trauma, certain heart diseases, metabolic disorders, tumors or drugs. A significant number of pericarditis cases are due to unknown causes (idiopathic).
Pericarditis may be acute or chronic in nature. It often co-exists with myocarditis, which is inflammation of the neighboring muscular layer of the heart known as the myocardium. The pericardium is a secretory lining, contributing to the approximately 30ml to 50ml of pericardial fluid between the two linings (pericardial cavity). With inflammation, there is usually some additional fluid accumulation in the pericardial cavity and this is known as a pericardial effusion. It may contain a number of solid and fluid components that is reminiscent of the disease process or the causative factor.
Types of Pericarditis
Serous Pericarditis
Irritation of the pericardial lining gives rise to an accumulation of serous fluid in the pericardial cavity containing some inflammatory infiltrate like lymphocytes. The serous fluid is sterile and is usually not associated with infection of the pericardium itself. However, serous pericarditis may arise with irritation of the pericardium secondary to infection of surrounding structures like the pleura of the lungs (pleuritis). It may gradually progress to a serofibrinous exudate, or purulent or hemorrhagic effusions depending on the nature and duration of the cause. The effusion is often straw-colored and contains protein.
Fibrinous Pericarditis
This type of pericarditis leads to a drying of the pericardial cavity as fibrin in the serous fluid (serofibrinous) eventually becomes organized. The extent of adhesion formation may vary. Fibrinous pericardiatis is usually not related to an infection although it may arise with chronic infections. It has a number of causes, including heart disease, injury to the heart, after cardiac surgery or due to autoimmune diseases.
Purulent Pericarditis
This type of pericarditis is also known as suppurative pericarditis and arises as a result of an infection. The invading pathogens may reach the heart through a number of routes including direct spread from neighboring sites (lungs, pleura), spread through the blood stream or lymphatic system, or direct infection seen with cardiothoracic surgery or penetrating injuries of the chest wall. It is more often seen with bacterial infections.
Hemorrhagic Pericarditis
This indicates the presence of blood in the pericardial effusion and may be seen in the backdrop of fibrinous or purulent pericarditis. This means that hemorrhagic pericarditis may arise with both infectious and non-infectious causes but the concern is often about malignant conditions (cancer of the pleura, breast, bronchus or lymphoma).
Other Types of Pericarditis
Granulomatous pericarditis may be seen with certain diseases like tuberculosis (TB), fungal infections, sarcoidosis or rheumatoid arthritis. It may progress to constrictive pericarditis over time where cardiac functioning is impaired due to a thick casing forming around the heart that limits cardiac expansion during diastole.
Another type of chronic pericarditis which results in severe damage and degradation of the pericardium is known as adhesive pericarditis. Cardiac functioning is not affected in adhesive pericarditis but the workload on the heart may be increased. It may be seen after infections, persistent inflammation, following cardiothoracic surgery or exposure to radiation.
Acute vs Chronic Pericarditis
Most cases of pericarditis are acute in nature eliciting sudden and intense symptoms that requires prompt treatment as it may quickly complicate to restrict the normal pumping action. This may occur with excess fluid accumulation around the heart (pericardial effusion) leading to a condition known as cardiac tamponade or in the chronic setting, fibrous tissue develops around the heart which is known as constrictive pericarditis.
Recurrent episodes of acute pericarditis may lead to the structural changes and complications seen in chronic pericarditis. With certain causes of pericarditis, particularly those that contribute to granulomatous pericarditis like TB, fungal infections, sarcoidosis and rheumatic fever, the symptoms may develop gradually and remain mild for a prolonged period of time. Chronic pericarditis is often painless which further contributes to a delay in diagnosis.
Signs and Symptoms of Pericarditis
Pericarditis Pain
The characteristic pain in pericarditis is sharp or stabbing chest pain behind the sternum (retrosternal / breastbone pain). It may be felt in the middle of the chest (central chest pain) or slightly to the left (left side chest pain). The pain usually worsens during movement, deep breathing, swallowing, coughing, changing position and exercise. Patients often report a relief of pain when leaning forward.
Pericardial Friction Rub
This is a sound that is heard upon auscultation (listening to the heart sounds with a stethoscope). It is described as a rough or grating sound (crunching or rubbing) that is most prominent during systole, end of expiration and when the patient is leaning forward.
Other Symptoms of Pericarditis
Most of the other symptoms of pericarditis are non-specific for the condition and often not as prominent as the pain and pericardial friction rub. These other symptoms includes :
- Low grade fever, seen especially with infections and autoimmune conditions
- Dry cough which exacerbates the chest pain
- Shortness of breath, especially when lying down
- Rapid breathing and rapid heart rate may also be noted
In more severe cases, swelling of the legs and/or abdomen, malaise and weakness may also be seen with pericarditis.
Causes of Pericarditis
The causes of pericarditis can be broadly divided into infectious and non-infectious. Infectious pericarditis, particularly bacterial, can progress rapidly and lead to severe complications in a short period of time. Viral pericarditis may be just as acute but depending on the virus involved, it can resolve spontaneously with minimal treatment. Other infectious causes includes tuberculosis, fungal infections and certain parasites which tends to lead to a more chronic pericarditis.
Among the non-infectious causes, the immune mediated conditions feature prominently. This includes rheumatic fever, systemic lupus erythematosus (SLE) and scleroderma. There is often an immune component involved in other conditions like after a myocardial infarction (heart attack) known as Dressler syndrome, cardiothoracic surgery and hypersenstivity to drugs.
Other causes may include heart diseases and trauma, including a myocardial infarction with secondary inflammation of the pericardium, injury to the pericardium, blunt chest injury, surgery, exposure to radiation, uremia and mediastinal tumors.