Polyps in Uterus Diagnosis and Treatment (Surgery, Medication)
Diagnosis of Uterine Polyps
Uterine polyps often go undetected because they do not cause any symptoms. However, when symptoms such as abnormal uterine bleeding occur in a woman, especially after menopause, it becomes important to investigate further to exclude the possibility of conditions such as endometrial cancer. Uterine polyps are often detected during screening in these cases. It may also accompany and should be differentiated from other causes of uterine cell overgrowth such as endometrial hyperplasia and uterine fibroids.
Clinical History
- Women with uterine polyps typically present with postmenopausal bleeding. This may be seen more so in patients who are currently or were previously taking the drug tamoxifen used in the treatment of breast cancer.
- There may be other types of abnormal vaginal bleeding in women who have not yet reached menopause such as heavy periods, irregular menstrual cycle, bleeding between periods or bleeding after intercourse.
- Sometimes, there may be a history of infertility.
Read more on the signs and symptoms under Uterus Polyp.
Physical Examination
A physical examination, including a pelvic examination, may also reveal :
- Anemia due to excessive menstrual blood loss.
- Lumpy feel of the uterus upon pelvic examination.
- Visible polyp protruding into the vagina through the cervix.
Other Diagnostic Measures
- An abnormal Pap smear may reflect an underlying endometrial polyp.
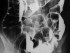
- Hysterosalpingogram (HSG) is an x-ray of the uterus taken after injecting a radio-opaque or contrasting dye into the uterus and may indicate the presence of polyps by the filling defects seen on the x-ray plate. HSG is usually done while investigating for the cause of infertility.
- Ultrasound findings of endometrial growths are often non-specific and cannot always help to arrive at a definite diagnosis. Transvaginal ultrasound, where the probe is placed in the vagina. may be more specific for a diagnosis of endometrial polyps.
- Sonohysterography may be a more sensitive and specific imaging technique for diagnosis.
- Hysteroscopy can help to visualize the uterine lining and detect polyps.
- Dilation and curettage (D and C) may be done to obtain a tissue sample.
- Endometrial biopsy can help to differentiate benign growths such as polyps and fibroids from endometrial cancer and precancerous changes such as endometrial hyperplasia. However, adequate tissue samples cannot always be obtained and there is also the risk of vaginal or cervical stenosis following biopsy.
- MRI can be helpful in differentiating these various growths.
Treatment of Uterine Polyps
The diagnosis of uterine polyp, whether single or multiple, and if associated with surrounding endometrial thickening is important in determining the type of treatment that is to be considered. Asymptomatic small polyps may not need to be removed. A “wait and watch” attitude with check-ups every six months, to monitor growth of the polyp or development of symptoms, may be sufficient. Women at risk of uterine cancer may be advised on polyp removal even in the absence of symptoms.
Uterine Polyp Surgery
- Polypectomy or polyp resection may be done if there are symptoms of menstrual abnormalities, pelvic pain, recurrent spontaneous abortions (miscarriage), or history of infertility.
- A polyp may be removed by cauterization, laser therapy, surgical excision, or in some cases by endometrial ablation therapy.
- D&C – the uterine polyp may be removed while doing a D&C procedure for diagnosis. Alternatively, a polyp associated with endometrial hyperplasia may need a D&C at the time of polyp resection. D&C may be done as a blind procedure without the aid of a hysteroscope or it may be guided by a hysteroscope to give proper visualization of the inside of the uterus.
- Hysteroscopic resection is when small uterine polyps are removed at the doctor’s office during hysteroscopy. Identification of multiple polyps by diagnostic procedures is important while doing hysteroscopic resection.
- Large polyps may be removed under general anesthesia in the operating room. This ensures proper ligation (tying) of the pedicle and adequate sutures at the site of attachment to the uterus so as to prevent possible bleeding.
- Multiple polyps may need a hysterectomy (surgical removal of the uterus) in selected cases. Hysterectomy is also the method of choice when malignancy is suspected.
Uterine Polyps Medication
Medical treatment may include the use of :
- nonsteroidal anti-inflammatory drugs (NSAIDs) to relieve pelvic pain,
- oral contraceptives (birth control pills) or progestins to control abnormal uterine bleeding,
- gonadotropin-releasing hormone (GnRH) agonists to shrink the polyps.
However, medical treatment is only a temporary measure and symptoms may recur once medication is stopped. There is also a chance of recurrence of uterine polyps even after surgical removal.