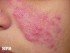
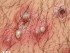
Psoriasis Skin Disease Explained, Pictures and Different Types
What is psoriasis?
Psoriasis is a chronic disorder marked by inflammation that can affect various systems throughout the body. It mainly manifests on the skin but often affects the joints as well. Although psoriasis is non-contagious, it tends to run in families thereby indicating a strong genetic component. The key features of psoriasis are associated with overgrowth of skin in the without rapid shedding leading to a buildup of skin cells. While various treatments have proven effective in the long term management and treatment of acute flare ups, psoriasis is incurable. It can cause significant physical scarring and has a major psychological impact on sufferers affecting normal functioning to varying degrees.
How does psoriasis develop?
Based on the disease mechanism, psoriasis appears to be an autoimmune disease. It shares similar traits with conditions like rheumatoid arthritis and a combination of skin and joint inflammation is therefore referred to as psoriatic arthritis.
Immune activity
The disease process (pathophysiology) of psoriasis is not well understood. It is believed that several factors play a role in the development of the condition.
Psoriasis appears to be largely an immune mediated disorder meaning that it is the body’s own immune system that “attacks” the skin. Immune cells congregate in the skin (dermis and epidermis) where it induces proliferation of the keratinocyctes – the outer skin cells. The skin becomes thickened in plaques and does not shed as fast as it should leading to the buildup of thick cells. Immune activity in the skin induces inflammation which presents as redness, itching and even swelling of the skin. The heightened immune activity within the affected sites may also lead to the formation of pustules or even large boils – pustular psoriasis.
Skin overgrowth
Normally the skin has a turnover rate of about 23 to 28 days. This means that new skin cells develop in the deeper layers and gradually move upwards until it reaches the superficial layers. It is then shed (desquamation). In psoriasis, however, keratinocyte proliferation and turnover rate is altered leading to overgrowth of the epidermis. This turnover rate is accelerated to levels as fast as 3 to 5 days. The skin cells are not able to mature as it normally would and the integrity of the skin is compromised as the cells are not able to perform its normal function.
Causes of Psoriasis
The exact cause of psoriasis is unknown but several contributing factors and possible triggers have been identified. Psoriasis is marked by periods of remission where the symptoms subside or even resolve complete. However, the condition tends to flare up again after weeks, months or even years. Psoriasis is a chronic condition and these episodes of remission and exacerbation continue throughout life.
Contributing Factors
Psoriasis is a multifactorial disease meaning that there is possibly more than one factor that causes the condition. This interplay of different factors is not always understood. The main contributing factors includes :
- Genetic factors. There tends to be a strong family history of psoriasis with certain genes and HLA antigens being associated with the condition.
- Environmental factors. Injury, infections and certain drugs may trigger the onset of psoriasis mainly in a person who is genetically susceptible.
Triggers
Many of the factors discussed below may be initial stimulus that triggers the onset and development of the disease in a person who is genetically susceptible. Other factors are usually not involved in the initial onset but play a role in the flare up later on in the condition.
- Cold climate.
- Trauma to the skin where psoriasis develops at the affected sites (lines) known as Koebner phenomenon. This includes sunburn.
- Medication like hypertensive medication (beta blockers and ACE inhibitors), lithium, NSAIDs like aspirin or indomethacin, antimalarial drugs and discontinuing corticosteroids.
- Alcohol abuse.
- Infections like HIV, streptococcal and staphylococcal skin infections.
- Psychological stress.
Obesity, cigarettes smoking and even moderate alcohol consumption can exacerbate the condition.
Types of Psoriasis
There are broadly five types of psoriasis which differ in presentation to some degree. However, all five types have common features and the disease mechanism is essentially the same.
Plaque psoriasis
This is the most common presentation and is also referred to as psoriasis vulgaris. As the name suggests, the skin lesions appear in plaques of red, raised skin with silvery-white flakes of skin on the surface. Commons sites include the major joints like the elbows and knees, lower back and scalp. Read more on scalp psoriasis.
Guttate psoriasis
In this type of psoriasis, the lesions appears as small red spots throughout the affected area. The term ‘guttate’ means drop which describes the appearance of the psoriasis lesion. The typical thickened plaques are largely absent in guttate psoriasis. It is a more common form in childhood or early adulthood.
Inverse psoriasis
This form of psoriasis appears as bright red patches of skin that is smooth and shiny. It tends to occur in the folds of the body other than the major joints such as the armpits, breasts (mainly in women), groin and buttocks. The tendency for it to arise in these areas appears to be associated with irritation from sweating, rubbing and scratching at these sites.
Pustular psoriasis
Pustular psoriasis, as the name suggests, is a form of psoriasis marked by the presence of tiny blisters (pustules) and severe scaling of the skin. These pustules are not related to a secondary bacterial infection of the skin, which can arise in psoriasis often leading to the larger abscess at the affected sites. There are three types of pustular psoriasis :
- Palmoplantar psoriasis on the fleshy areas of the palms (hands) and soles (feet).
- Von Zumbusch pustular psoriasis where there is the sudden appearance of pustules over tender reddened skin which then dry and peel away. The pustules may then recur shortly thereafter.
- Acropustulosis is a rare type of pustular psoriasis that arises at the fingertips or the tips of the toes. It may cause deformity of the nails.
Erythrodermic psoriasis
This type of psoriasis is extensive covering most of the body surface and marked by intense inflammation. The skin has an intense red hue and the skin is shed in sheets rather than flakes. The itching and pain is severe and it may overlap with Von Zumbusch pustular psoriasis at some sites. Erythrodermic psoriasis is a systemic condition accompanied by changes in heart rate and body temperature. It is often seen as the worst form of psoriasis.
Signs and Symptoms
Although the presentation can vary depending on the type of psoriasis described above, all forms share common features.
- Redness of the skin
- Scaling, flaking, peeling skin
- Dry silvery-white scales
- Itching and sometimes pain
- Pustules at times
There may be joint symptoms as well such as joint swelling, joint pain and joint stiffness
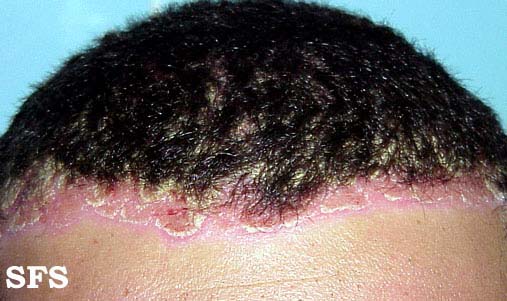
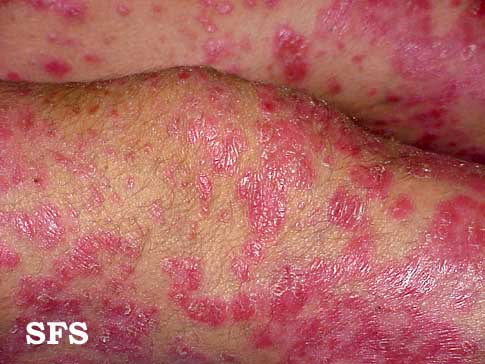
Pictures
 |
 |
 |
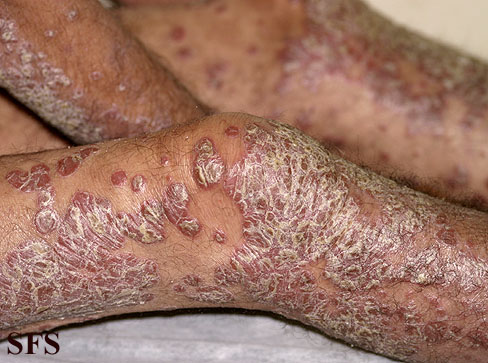 |
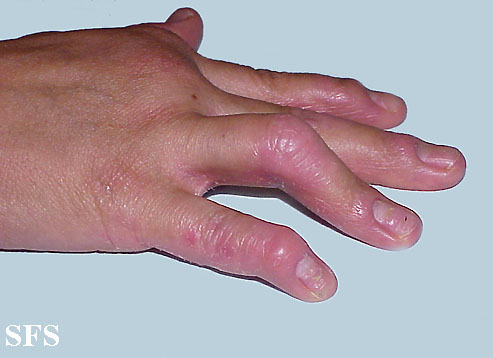 |
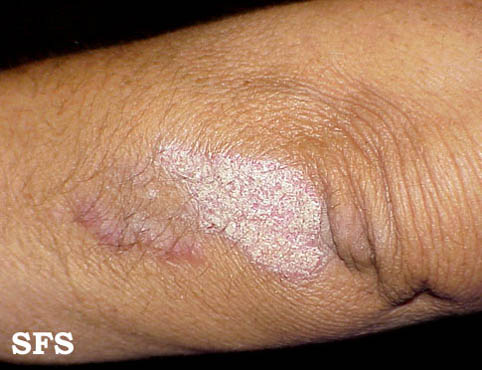 |
| Pictures from Dermatology Atlas Brazil courtesy of Samuel Freire da Silva, M.D. | |