Regurgitation of Food and Fluids, Causes and Other Symptoms
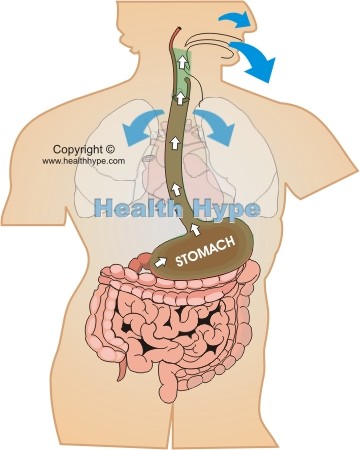
The alimentary tract extends from the mouth to the anus. Food or drink, once swallowed, should only travel in one direction – down the alimentary tract. From the mouth it passes into the throat with voluntary swallowing and then reflexes coordinate involuntary processes that transports the food or drinks down the esophagus. From here it passes to the stomach, then the small intestine and after passing through the large intestine, any remnants are eventually expelled as feces. The contractions of the muscles in the wall of the gut that facilitates the movement of substances within is known as peristalsis. Sometimes the contents of the small intestine, stomach, esophagus or throat can travel in the opposite direction which is known as antiperistalsis. If it is forcefully expelled then it is known as vomiting. However, in some cases the violent eruption as seen with vomiting is not present. Instead the contents pass out quite passively in comparison to vomiting and this is known as regurgitation.
What is regurgitation?
Regurgitation is the passing out of undigested or partially digested food or fluids that are expelled in less forceful manner than with vomiting. Although the terms regurgitation and vomiting are used interchangeably, regurgitation is synonymous with the more widely used term ‘reflux’. It is generally limited to the ingested contents within the latter part of the throat, esophagus and stomach. Usually the contents that have passed into the small intestine cannot be passed out in this passive manner and has to be forcefully pushed out through the process of vomiting. Depending on the site from where the contents are passed out, it may be mixed with mucus, water or stomach acid and enzymes. Sometimes the regurgitated contents may pass out through the nose (nasal regurgitation) or may even enter the airways (tracheal aspiration).
Vomiting occurs when there is irritation or overdistension of the gut. It may also be a result of abnormal stimulation of the muscles in the gut in a manner that allows for reverse peristalsis. The contractions can start from as low as the the first-third of the small intestine and therefore all the contents proximal to the origin can be expelled. Regurgitation is more of a ‘pouring out’ or ‘flowing out’ phenomenon and is associated with an impaired swallowing reflex, weak peristaltic contractions or poor coordination and the dysfunction of certain valves, like the lower esophageal sphincter (LES). These mechanisms normally ensure that ingested food and drinks do not pass out again through the mouth.
Regurgitation may occur frequently in infants and is not considered abnormal if the baby is healthy and thriving. This typically follows a feed and is a result of air trapped within the gut pushing up the ingested milk and immature valves that allow for reflux of the gastric contents.
Other Symptoms with Regurgitation
The characteristic ‘sick’ feeling known as nausea that typically precedes vomiting is usually absent in regurgitation. The presence of other symptoms depends largely on the cause and the site from where the material is being expelled. When food and fluids from the stomach are regurgitated, as is the case with acid reflux, the stomach acid may cause a burning sensation in the chest (heartburn). It is often accompanied by a sour taste in the mouth. If the contents are expelled from higher up in the gut, where no significant digestion has occurred the there may be some degree of gagging and choking. Difficulty swallowing (dysphagia) is a common feature that accompanies certain causes of regurgitation. When normal peristalsis is impaired, a person may also complain of pressure in the chest or a sensation of fullness (bloating) as the food is not propelled through the esophagus.
Causes of Regurgitation
The causes of regurgitation may not differ significantly from that of vomiting. Many causes do overlap and it is not uncommon for regurgitation to be reported as vomiting and vice versa.
Gastroesophageal Reflux Disease
The most common cause of regurgitation is a lower esophageal sphincter (LES) dysfunction which also accounts for chronic acid reflux – gastroesophageal reflux disease (GERD). The reflux or regurgitation is more prominent when lying flat, after eating and with activity. In more severe cases, even bending forward or even belching can cause reflux where the gastric contents enter the esophagus and may even reach the mouth.
Upper Gastrointestinal Obstruction
An obstruction can occur anywhere in the gut and may arise as a result of a mass (within or outside the gut), strictures (abnormal narrowing), excessive and prolonged contraction of the gut muscle (spasm) or a foreign body. The site of the obstruction may be i the laryngopharynx, esophagus or stomach. However, a blockage further down the gut can contribute to regurgitation as the backed up contents prevents recently ingested food and drink from passing down the gut.
Lower Esophageal Sphincter
Dysfunction of the lower esophageal sphincter, either significantly increased or decreased tonicity, can contribute to regurgitation. As discussed above under GERD, decreased tonicity allows the gastric contents to empty into the esophagus. However, with conditions like achalasia, the muscles that make up the LES remain contracted and restrict the passage of food into the stomach. Food accumulates in the esophagus as it enters the stomach very slowly. However, if there is consumption of a large meal or a dilated gut (complication of achalasia) then regurgitation will be a prominent feature.
Neuromuscular Disorders
Swallowing and peristalsis is a carefully coordinated process controlled by the nerves and facilitated by the muscles. If there is any disruption due to the disease or dysfunction of either the nerves or muscles or even both, then regurgitation may be present. These diseases must afflict the nerves and/or muscles of swallowing including the centers in the brain that are responsible for this mechanism. Certain medication may also affect the normal activity of the muscles and/or nerves. Some causes may include :
- Stroke (cerebral infarction)
- Gastroparesis
- Myasthenia gravis
- Multiple sclerosis
- Motor neuron disorders
- Muscular dystrophy
- Parkinson’s disease