Rheumatic Fever Causes and Joint, Heart, Skin, CNS Symptoms
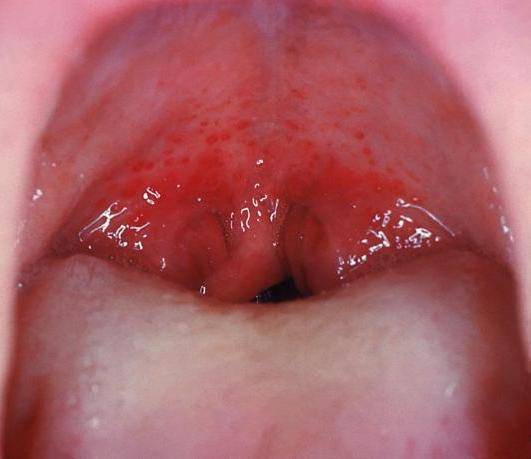
A throat infection is one of the most common upper respiratory tract conditions affecting every person at some point in life. The most common pathogens are viruses and then bacteria. Among the different types of bacteria, it is the group A streptococci (Streptococcus pyogenes) that are more commonly involved in a sore throat. The infection causes widespread inflammation of the throat (pharynx) and is therefore known as streptococcal pharyngitis or commonly as strep throat. The immune system elicits the appropriate response against the infection and antibiotics also help with fighting off the infection. Sometimes the immune activity against becomes disrupted and is then directed towards the body’s own tissues. Rheumatic fever occurs a period after the strep throat infection and affects many organs and systems.
What is Rheumatic Fever?
Rheumatic fever is a delayed immune response that causes inflammation of many tissues and organs throughout the body a few weeks after a strep throat. It is more frequently seen in children and teens between the ages of 5 and 15 years of age. While it primarily occurs after a throat infection with certain strains of group A streptococci, it may sometimes occurs with a streptococcal infection elsewhere in the body although this is very rare. Rheumatic fever is an acute reaction that often affects the heart, joints, skin and nerves. It may in sometimes cause long term damage as is the case with rheumatic heart disease.
How does rheumatic fever occur?
The immune system forms antibodies against the proteins (antigens) of an invading microorganism. The antibodies can then bind to the antigen and form an antigen-antibody complex that directs immune activity. In this way the body’s immune response is targeted and immune cells can accurately identify the invader and attack appropriately. At the same time it ensures that the immune activity is not directed at the healthy cells of the body. The same process occurs with a streptococcal infection but sometimes the antibodies formed against the antigens of the group A streptococci cross reacts with the body’s tissues (self antigens).
When does rheumatic fever occur?
Rheumatic fever tends to occur anywhere between 10 days to 6 weeks after an episode of streptococcal pharyngitis. Typically this is around week 2 to 3. The initial streptococcal infection has resolved by this time and cultures are often negative.
Causes of Rheumatic Fever
While rheumatic fever follows a streptococcal pharyngitis, there is growing evidence to suggest that genetics may play a role in susceptibility. The exact reason why rheumatic fever occurs in only some people with a streptococcal pharygitis is unclear. Most of these cases, however, are associated with an untreated strep throat and this condition is therefore more common in developing nations.
Group A streptococci are highly contagious bacteria and are easily transmitted from one person to another via droplet spread. This means that an uninfected person can contract the infection when exposed to an infected person who is sneezing or coughing or by sharing food and drink. Streptococcal infections of the throat often occurs secondary to a viral respiratory tract infections like the flu (seasonal influenza) and common colds.
Picture of Strep Sore Throat from Wikimedia Commons
Rheumatic fever often passes by undetected particularly if there is limited access to health facilities. Heart valve disease detected later in life, particularly mitral stenosis, is often attributed to a forgotten or undiagnosed case of rheumatic fever. There is an increased risk of further episodes of rheumatic fever in life after the initial episode.
Signs and Symptoms of Rheumatic Fever
Rheumatic fever presents with a fever and various clinical features associated with inflammation of the joints, skin, heart and central nervous system. These signs and symptoms are non-specific for rheumatic fever and therefore a combination of features, as laid out in the Jones are often considered for a positive diagnosis.
Joints
Rheumatic fever presents with joint inflammation (arthritis) in about 75% of patients. It tends to affect several large joints one after the other (migratory polyarthritis) and may involve the knees, elbows, ankles and wrists. The joints appear swollen, red and tender and this typically lasts for approximately 4 weeks. It may also affect the joints of the fingers and hands, hips, shoulders and feet although this is uncommon.
Heart
Inflammation of the heart in rheumatic fever is known as acute rheumatic carditis. It involves all three layers of the heart and is more accurately referred to as a pancarditis. Depending on the severity and extent of involvement, the heart wall and linings, its valves and circulation to the lungs (right side of the heart) and rest of the body (left side) may be compromised to varying degrees. This may manifest as an arrhythmia, tachycardia, palpitations, cardiac murmurs, chest pain, breathlessness, dizziness and fainting. About half of all patients who present with carditis may develop chronic heart disease (rheumatic heart disease).
Skin
The skin lesions in rheumatic fever appear as red rings that are flat or slightly raised (erythema marginatum) and is not itchy. It tends to appear on the trunk and legs but not on the face. Initially the rash in rheumatic fever appears as red blotches (macules) and the center of the rash then gradually disappears to form the red rings seen in erythema marginatum. Subcutaneous nodules are firm but painless lumps that can be felt under the skin, particularly on the extensor surfaces. These lumps are small measuring only about 0.5 fo 2.5 centimeters. Both erythema marginatum and subcutaneous nodules occur in only about 5% of patients with rheumatic fever.
Nervous System
Neurological features tend to occur late in rheumatic fever often when all other signs and symptoms have disappeared. This can be as late as 3 months after acute rheumatic fever and is more commonly seen in females. Patients initially present with emotional sensitivity, moodiness and outbursts. This is then followed by uncontrollable jerky movements and tics particularly in the face, hands and feet which is known as Sydenham’s chorea (St Vitus dance). These neurological features tend to resolve spontaneously within a few months.
Jone’s Criteria for Rheumatic Fever Diagnosis
A diagnosis of rheumatic fever is made if there is the presence of :
- two or more major features, OR
- one major and two or more minor features.
Major Features
- Inflammation in more than one joint (polyarthritis)
- Inflammation of the heart (carditis)
- Involuntary jerky movements (chorea)
- Red rings on the skin (erythema marginatum)
- Small lumps under the skin (subcutaneous nodules)
Minor Features
- Fever
- Joint pain (arthralgia)
- Raised ECR or CRP
- Previous episode(s) of rheumatic fever
- Prolonged PR interval