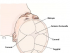
Viral, Bacterial, Fungal Meningitis Facts, CSF Results, Treatment
Meningitis or inflammation of the meninges is most often caused by viral, bacterial, or fungal infections. It may occur as complication of skull or spinal injury, cancer, or connective tissue disorders. The meninges are membranes that cover and protect the brain and spinal cord. Meningism or symptoms of meningeal irritation may be present in meningitis due to any cause. Newborns and younger children may not always have the typical symptoms of meningitis, which often makes diagnosis difficult. Antibiotics should be commenced if bacterial meningitis is suspected, even before investigations can be undertaken or without waiting for results of tests. Meningitis is contagious and may spread through coughing, sneezing, and any sort of close contact.
- Viral meningitis is the most common, especially in children and young adults, but it usually resolves on its own and does not cause serious side effects.
- Bacterial meningitis is the most severe form and unless it is treated promptly with appropriate antibiotics, it may lead to severe long term complications or even death.
- Fungal meningitis is usually caused by inhaling fungal spores from the environment. Unlike viral and bacterial meningitis, fungal meningitis is not contagious.
Viral Meningitis
Viral infection of the meninges is the most common cause of meningitis. Of the many viruses that can cause meningitis, the most common are enteroviruses such as echovirus, which are normally present in the intestine and may be spread by contaminated food or water. Viral meningitis may also be caused by the influenza, measles, and the mumps virus.
The primary infection, such as mumps or measles, is highly contagious but not all infections lead to meningitis. Viral meningitis occurs mainly in children and young adults. Symptomatic treatment is all that is necessary in most cases since viral meningitis is a self-limiting disease that does not require any specific treatment. Patients usually recover within a few days, often without any medical intervention. Long term complications are unlikely.
Causes of Viral Meningitis
- Enteroviruses such as echoviruses, coxsackieviruses, polioviruses.
- Mumps virus.
- Measles virus.
- Influenza virus.
- Herpes simplex virus.
- Japanese encephalitis virus.
- Rabies virus.
- Arboviruses.
- Human immunodeficiency virus (HIV).
- Lymphocytic chorionmeningitis virus (arena virus).
Bacterial Meningitis
Bacterial meningitis is less common than viral meningitis but prompt diagnosis is very important since it can have serious consequences if not treated as an emergency. Delay in treatment can lead to serious complications or even death. Appropriate antibiotic treatment should be started immediately on the slightest suspicion of bacterial meningitis.
Bacterial meningitis is a highly contagious disease. It usually occurs when bacteria enter the nasopharynx, colonize it, and then invade the blood stream to produce septicemia. Through the blood stream, bacteria may reach the brain and spinal cord and cause meningitis. Bacteria may also affect the meninges by direct spread from infection in ear (otitis media), nasal sinuses (sinusitis), head or spinal injury.
Risk Factors
- Overcrowded communities, schools, day care center, dormitories, and military bases.
- Infants, young children, and elderly people.
- Children who have not been given routine childhood vaccination.
- Traveling to countries where the disease is endemic.
- Head or spinal injuries.
- Brain or spinal surgeries.
- Sickle cell disease.
- Alcoholics.
- Diabetics.
- Antibody deficiency, as in premature infants or elderly patients.
- Infections such as pneumonia, otitis media, and sinusitis.
- Immunocompromised individuals, such as those suffering from and undergoing treatment for AIDS and cancer. People with sickle cell disease and those who have undergone splenectomy (surgical removal of the spleen) are also at increased risk.
- CSF shunts.
Long term complications of bacterial meningitis may include permanent neurological deficits such as :
- Mental retardation.
- Deafness.
- Brain damage.
- Cranial nerve palsies.
The bacteria most commonly involved are :
- Neisseria meningitides (Meningococcus)
- Streptococcus pneumoniae (Pneumococcus)
- Hemophilus influenzae (Hemophilus)
- Listeria monocytogenes (Listeria)
- Tuberculous meningitis
Neisseria Meningitides (Meningococcus)
Meningitis caused by this organism is highly contagious and can result in the most serious type of meningitis. Within a very short time the infection can reach dangerous proportions. It usually affects children and young adults. A person may become infected by close contact with an infected person. Coughing, sneezing, and kissing help in spread of disease. It is likely to spread rapidly in people living in cramped living conditions, day care centers, dormitories, schools, and military bases.
Complications of meningococcal septicemia may include :
- Meningitis.
- Shock.
- Intravascular coagulation.
- Kidney failure.
- Gangrene.
- Arthritis.
- Pericarditis.
Streptococcus Pneumoniae (Pneumococcus)
This is the usual causative organism for pneumonia, sinusitis, or otitis media. Pneumococcal meningitis occurs most commonly in newborns, children, and adults.
Hemophilus Influenzae (Hemophilus)
The incidence of meningitis caused by Hemophilus type b (Hib) organism has greatly reduced since the advent of Hib vaccination which is administered to children routinely as part of their immunization schedule. If it does occur, it usually follows an upper respiratory tract infection, sinusitis, or otitis media.
Listeria Monocytogenes (Listeria)
This is increasingly seen in recent years as the cause of meningitis in immunocompromised people, alcoholics, diabetics, and pregnant women. It is also a frequent cause of meningitis in the newborn. The bacteria may be found in the soil, dust, and contaminated food such as cheese and beef burgers. Animals may act as carriers.
Tuberculous Meningitis
Tuberculosis in childhood may be followed tuberculous meningitis or it may occur as part of miliary tuberculosis. The causative organism is Mycobacterium tuberculosis. Antituberculous treatment should be started. Steroids are also indicated in these patients. Prognosis is good with timely treatment. Death may occur in untreated patients.
Fungal Meningitis
This is a rare form of meningitis. It is not contagious and may be caused by inhaling spores from the environment. Cryptococcal meningitis is the most common type of fungal meningitis, caused by the organism Cryptococcus neoformans. It usually causes chronic meningitis but rarely acute symptoms may develop. People with weakened immune system are most at risk. It is a common complication of HIV infection. It can also occur in patients who have a focus of fungal infection. Recurrence is common after treatment.
The CSF findings may be similar to those of tuberculous meningitis. Diagnosis may be made by culture or recognition of spores in the CSF biopsy and serological detection of antigen. Antifungal medication should be given to avoid potentially life-threatening complications.
CSF Results
For more information refer to diagnosis of meningitis. Specific findings with respect to the type of infection is discussed here.
CSF in Viral Meningitis
The CSF is usually clear in viral meningitis. The cell count may be around 10 to 2000 and may show excess of lymphocytes. Glucose and protein levels are normal. Gram stain is negative.
CSF in Bacterial Meningitis
The CSF is usually turbid or purulent in appearance. The cell count is usually high. It may be between 1,000 and 50,000 with polymorphs predominating. Glucose may be low and protein levels normal or elevated. Gram stain is positive.
CSF in Tuberculous Meningitis
The CSF is usually clear but a fine clot or fibrin web may form on standing. The cell count may be 50 to 5000, predominantly lymphocytes. Protein level may be high but there is a marked fall in glucose level. Gram stain is often negative.
CSF in Fungal Meningitis
The cell count is low. It may be 50 to 500, with predominance of lymphocytes. Protein level may be elevated but glucose level is low. Gram stain may be positive or negative.
Treatment
For more information, refer to treatment of meningitis. Specific therapeutic guidelines for each type of infectious meningitis is discussed here.
Viral Meningitis
No specific therapy is required for viral meningitis. Symptomatic treatment for headache, fever, and other associated symptoms may be given. Complete recovery occurs in almost all cases. Antiviral drugs such as acyclovir may be given, especially in patients with signs and symptoms of meningoencephalitis.
Bacterial Meningitis
Antibiotic treatment should be started as soon as possible if there is a suspicion of bacterial meningitis. Treatment should not be delayed if tests cannot be done immediately. Appropriate antibiotics should be started without waiting for results of the tests.
Antibiotics will be given considering the most likely organism. This may be based on the patient’s age, if there is a known local outbreak of the disease, whether it is hospital or community acquired, or whether the person is immunocompromised.
- Meningococcus – benzylpenicillin, cefotaxime, or ceftriaxone.
- Pneumococcus – cefotaxime or ceftriaxone. Vancomycin may be added.
- H. influenzae – cefotaxime, ceftriaxone, or chloramphenicol.
- E. coli – cefotaxime or ceftriaxone.
- S. aureus – flucloxacillin.
- L. monocytogenes – gentamycin plus ampicillin.
Household and other close contacts, especially children, should be protected against meningococcal meningitis, which is extremely contagious. Rifampicin may be given as prophylaxis to children and adults.
- For adults, the dose is 600 mg twice a day for 2 days. Adults may also take ciprofloxacin 500 mg as a single dose for prophylaxis.
- For children under 1 year it is 5 mg /kg 12 hourly, and for those over 12 months it is 10 mg/kg 12 hourly, both given for 2 days.
Vaccination can protect against some types of bacterial meningitis.
Tuberculous Meningitis
Antituberculous regimen should be started immediately on diagnosis. The drugs used may be rifampicin with ethambutol, isoniazid, streptomycin, and pyrazinamide. The steroid prednisolone should be given to all patients. Adequate nutrition is of utmost importance during treatment. Eight weeks of intensive drug therapy should be followed by a continuation phase.
Fungal Meningitis
Antifungal medication such as amphotericin B plus flucytosine is usually prescribed.