Why Frozen Shoulder Exercises ?
What Is a Frozen Shoulder Syndrome?
Frozen shoulder or adhesive capsulitis (Latin adhere = to stick; capsulitis = inflammation of the (shoulder) capsule) is a condition causing pain and stiffness of the shoulder joint leading to profound disability and discomfort. This is a chronic condition, frequently associated with sedentary lifestyle and lack of exercise. It generally affects the non-dominant shoulder of women in the 4th to 6th decade of life. In diabetics, adhesive capsulitis often both shoulders.
Shoulder Anatomy
The shoulder joint is a highly mobile ball and socket type of joint, permitting movement in all directions . These movements are critical for the extensive usage of the upper limb.
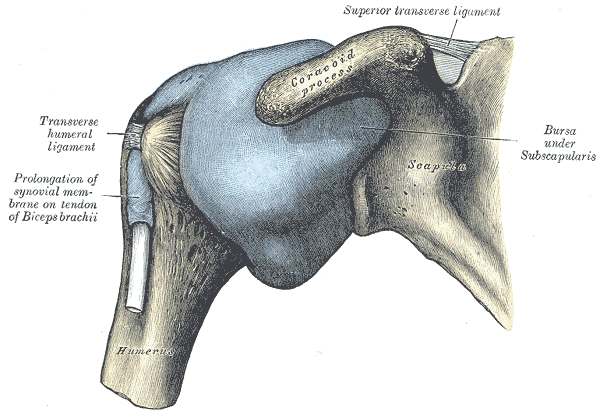 Picture 1: Shoulder Joint Capsule (blue)
Picture 1: Shoulder Joint Capsule (blue)
(source: Wikimedia << click to enlarge image)
The capsule of the shoulder joint (Picture 1) is loose, compared to other ball and socket joints in the body, so as to allow free movement of the joint. Though, this comes at the cost of stability, often making the shoulder joint vulnerable to injuries, like dislocations and muscle tears.
Pathophysiology
The disease can be primary or secondary. The primary adhesive capsulitis occurs without any known specific cause. The secondary adhesive capsulitis occurs due to old fractures near the shoulder joint, surgery involving structures near the shoulder joint, e.g. breast surgery, rotator cuff repair surgery, etc., or immobilization of the shoulder joint.
The loose capsule of the shoulder joint is frequently inflamed; this, coupled with inactivity or immobilization, leads to adhesions of the joint capsule, causing severe pain at the extremes of the range of motion. Stiffness and joint pain lead to more inactivity, further increasing the adhesions and making it a vicious cycle. With time, the adhesions organise into thick fibrous bands of scar tissue furtherly aggravating the stiffness.
The pathological process in diabetic patients is no different; however, the slower healing process and the deficient circulation in small blood vessels alters the inflammatory response. Thus, predisposing them to develop frozen shoulder more commonly and bilaterally.
Self treatment with painkillers reduces pain completely, but it does not stop a disease process, which continues to restrict joint motion. Thus, by the time a person visits a doctor, the joint movements are often barely possible, and the symptoms no longer respond to conservative treatment because of advanced adhesions.
Symptoms
Pain and stiffness of the shoulder joint are main symptoms. Symptoms may appear in a specific shoulder movement, e.g. reaching a high object, hair combing, or taking the hand behind the back (most frequent). The most important symptom in frozen shoulder is that it affects active as well as passive movements of the shoulder; it means that even someone else cannot move your shoulder beyond the restricted range of motion, no matter how hard you try to relax. This is unlikely in other causes of shoulder pain and it signifies something (hardened capsule) is physically obstructing shoulder joint movements.
Diagnosis
The diagnosis of frozen shoulder begins with ruling out other diseases with similar symptoms. Though frozen shoulder does not have any specific signs, a few investigations are routinely done in all patients:
- An X-ray of the shoulder does not show any changes, but are necessary to look for old fractures, neglected dislocations, arthritis, etc., which can be the root cause of symptoms.
- Blood sugar estimation helps to rule out diabetes.
- MRI, CT or bone scan may be done, if additional disorders, like rotator cuff disease or osteoporosis are suspected.
Treatment of Frozen Shoulder
Once a diagnosis is established, the patient is started on painkillers and light range of motion exercises for a period of 2-3 weeks. During this period, a patien often feels better and neglects the exercise regimen which is a bit painful and difficult initially. Exercises should never be skipped, as the painkillers only give temporary relief. Exercises are the ones that break the adhesions in the joint capsule giving permanent abatement of symptoms. In case, exercises are causing severe pain and discomfort, a physician should be re-consulted and better painkillers started, so that the exercise regimen is not compromised. Starting the exercises one week after starting the painkillers is more effective in securing patient compliance for the exercise regimen.
In some patients, local steroid injections or Depo-medrol injections may be used for effective pain relief, but have no significant role in altering the disease process. They can also weaken the rotator cuff and make it more susceptible for tearing, so they should be avoided.
Frozen Shoulder Manipulation
Frozen shoulder not responding to the above treatment is called refractory frozen shoulder. This frequently occurs in diabetics with poorly controlled blood sugar levels. Diabetics have poor healing along with deficient small vessel circulation, what are main reasons for a failure of the exercise regime. Hence, they are candidates for manipulation, in which a person is given general anesthesia and the shoulder is forcibly moved in all planes of motion to break the adhesions of the joint capsule.
Frozen Shoulder Surgery
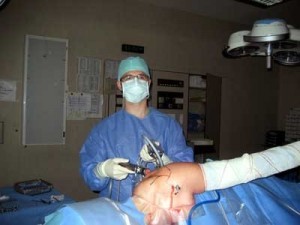
Picture 2: Shoulder Arthroscopy
(source: Wikimedia)
Arthroscopic adhesiolysis is an advanced technique in which adhesions are surgically released by visualizing the joint capsule through a fiber-optic cable passed into the shoulder joint (Picture 2). The procedure has an advantage of exactly releasing adhesions rather than simply tearing them with manipulation.
Prevention of Frozen Shoulder
Regular free arm exercises help to keep the joint active and prevent frozen shoulder. Apart from this, diabetics should take special care to keep their blood sugar levels under control, so as to stay away from this painful and disabling disease.
