Calcific Tendonitis (Rotator Cuff Tendons of the Shoulder)
What is calcific tendonitis?
Calcific tendonitis, or calcifying tendonitis, is a condition where calcium deposits form in the tendons of the rotator cuff muscles. These muscles are commonly referred to as the shoulder muscles. Calcific tendonitis can affect any tendon in the body but it is the rotator cuff tendons that are most often affected. It is not the same condition as a frozen shoulder (adhesive capsulitis). Calcific tendonitis causes severe shoulder pain but usually resolves on its own within a month. Supportive measures may be all that is necessary to manage pain and discomfort although in some cases, surgery may be needed.
How common is calcific tendonitis?
Calcific tendonitis is a fairly common condition affecting up to 20% of the general population. However, it is often mistaken for frozen shoulder which is more widely known in terms of shoulder pain. Calcific tendonitis is more common among adults in the 30 to 50 year age group with people over 40 years being the most affected. It is rarely seen in younger people. Diabetics and women are more frequently affected.
Shoulder Tendon Calcification
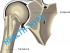
Tendons are the bands of connective tissue that attach muscles to bones. It is elastic and can stretch when a muscle contracts but recoils to its original length when the muscles relax. The rotator cuff muscles comprises four muscles that moves the arm and also provides support and stability for the shoulder joint. The four rotator cuff muscles include :
- Supraspinatus muscle
- Infraspinatus muscle
- Teres minor muscle
- Subscapularis muscle
In calcific tendonitis there are small amounts of calcium deposited in the tendons. The tendon of the supraspinatus muscle is most commonly affected and the subscapularis tendons are the least affected. More than one tendon may be affected at the same time.
Degenerative or Reactive Calcific Tendonitis
It was previously believed that calcific tendonitis arose due to age-related changes of the tendons. However, the highest incidence is noted in younger adults and age-related changes do not seem to account for all cases of calcific tendonitis. Therefore the condition is classified as degenerative or reactive.
- Degenerative calcific tendonitis is a condition where wear and tear of the tendons with age then leads to calcification.
- Reactive calcific tendonitis occurs for unknown reasons and does not seem to be related to age or wear and tear.
The type of calcification differs between degenerative and reactive calcific tendonitis. In degenerative tendonitis the deposits are just calcium and not the type of calcium phosphate (hydroxyapatite) as is seen with reactive tendonitis. Sometimes even tiny amount of calcium can deposit in an otherwise normal tendon but this is usually short lived and often asymptomatic.
Stages of Calcific Tendonitis
Calcific tendonitis can be divided into three stages – pre-calcific, calcific and post-calcific.
Pre-Calcific Stage
In this stage the tendons undergo structural changes that increase the likelihood of calcium deposits forming at the site. There is usually no pain at this point.
Calcific Stage
In this stage calcium is deposited in the tendons. The deposits gradually enlarge and reach about 1 to 2 centimeters in size. The deposits closely resemble chalk. Although the deposits are usually not painful at this point, it can cause restriction of movement. The calcium deposits remain for a period of time (resting phase) before it begins to “dissolve” (resorptive phase). Pain is usually more prominent in this resorptive phase.
Post-Calcific Stage
This is where the calcium has been resorbed and fibroblasts remodel the tendons into the normal tendon tissue that existed prior to pre-calcification. Pain and any other symptoms are usually absent at this point.
Signs and Symptoms
The main symptoms of calcific tendonitis is seen during the resorptive phase of the calcific stage. Pain is due to inflammation triggered by the presence of the calcium deposits. It is usually deposits that are larger than 1.5 centimeters in size that are more likely to elicit symptoms. These symptoms include :
- Pain, which is mild before the resting phase, and severe pain during the resorptive phase.
- Difficulty elevating the arm.
- Stiff shoulder.
- Sleep problems associated with severe pain.
- Shoulder weakness.
- Grating sound from the shoulder joint during movement.
- Rubbing or grating feeling with joint movement.
The right shoulder is more commonly affected in calcific tendonitis but up to half of all patients may have the problem in both shoulders.
Causes of Calcific Tendonitis
There is as yet not a clear understanding of what causes calcific tendonitis, particularly reactive calcific tendonitis. Although degenerative calcific tendonitis appears to be age-related, it may also develop in younger people with excessive wear and tear due to overuse. However, in reactive calficic tendonitis the condition seems to occur spontaneously. Risk factors include :
- Being female. Women are more commonly affected than men.
- Housewives and clerical workers seem to be at a higher risk.
- Diabetes mellitus appears to be a risk factor for the development of calcific tendonitis.
Despite these risk factors and a better understanding of the mechanism behind the calcification process, the trigger for the onset of calcific tendonitis is unknown.
Tests and Diagnosis
Calcific tendonitis is at times discovered during routine investigations like x-rays even when patients are asymptomatic. However, it is shoulder pain that is the main reason why patients seek medical attention and are then diagnosed with calcific tendonitis. The shoulder pain in calcific tendonitis is said to be excruciating and similar to frozen shoulder. Further tests that are warranted for the diagnosis and includes :
- X-rays
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Ultrasound
These imaging studies help visualize the calcium deposits in the tendons of the rotator cuff muscles. Seeping of the calcium into the subacromial space may also be noted.
Calcific Tendonitis Treatment
Most cases of calcific tendonitis resolve spontaneously with 1 to 4 weeks and no specific treatment is required apart from supportive measures. This includes icing the area, limiting movement of the shoulder joint and physical therapy. However, in very severe or persistent cases, surgery may be considered.
Non-Surgical
- Medication :
– Non-steroidal anti-inflammatory drugs (NSAIDs) to reduce inflammation and ease pain.
– Corticosteroids to reduce swelling and inflammation.
– Analgesics to manage severe pain. - Physical therapy :
– Ice and heat therapy.
– Electrotherapy.
– Exercises to maintain range of motion and prevent loss of muscle strength. - Lavage :
– Using needles to break up the calcium deposits.
– Injecting saline solution and aspirating the fluid to wash out the calcium. - Extracorporeal shock wave therapy :
– Using sound waves to “blast” the calcium deposits.
Surgical
- Open surgery :
– Tendon is surgically cut open.
– Calcium deposits are scraped out.
– Some of the tissue at the edge of tendon may be removed.
– After surgery, the arm is immobilized with a sling for 3 days. - Athroscopic surgery :
– Less invasive endoscopic procedure that is preferred over open surgery.
– Calcium deposits in the tendon are surgically removed (resection).
– Area is rinsed out to remove any loose calcium crystals.
References :
http://www.orthogate.org/patient-education/shoulder/calcific-tendonitis-of-the-shoulder.html