Cyanosis (Blue to Purple Skin Color) Meaning, Causes, Symptoms
What is cyanosis?
Cyanosis is the medical term for a blue to purple discoloration of the skin which arises from deoxygenated hemoglobin in the blood stream. It may also be seen on the mucous membranes, especially of the mouth, tongue and eyes. Cyanosis is a sign of low oxygen levels in the blood (hypoxemia). It occurs when there is an inadequacy in lung oxygenation or blood circulation.
The red blood cells carry oxygen through the blood stream by binding it to the molecule hemoglobin. It gives the blood its characteristic red color. The higher the blood oxygen saturation, the redder the color of blood. Hemoglobin molecules that do no contain oxygen (deoxygenated hemoglobin) has a dark red to purple color. This is usually not evident since the circulating red blood cells are quickly oxygenated again as it travels through the blood vessels of the lung.
However, under certain conditions, the blood may not be oxygenated fast enough and the deoxygenated hemoglobin builds up. Cyanosis is evident when the blood in the arteries contain more than 5 grams of deoxygenated hemoglobin per 100 milliliters of blood (> 5g/dL or > 50g/L). This is hypoxemia which is the decrease in partial pressure of oxygen in the blood, or simply, insufficient blood oxygenation with an oxygen saturation (SaO2) of less than 90%.
Oxygen saturation is the measure of oxygen transported in the blood stream expressed as a percentage relative to the maximum oxygen-carrying capacity. Cyanosis can be central where the bluish discoloration of the skin is evident on the face, particularly the mouth and tongue, or it may be peripheral where it is only evident in the arms and legs, particularly the fingertips and toes, and even the ears.
What does cyanosis mean?
Cyanosis is an indication of one of two disturbances – lung oxygenation is compromised or blood circulation is inadequate. The respiratory and cardiovascular components may sometimes co-exist. Cyanosis associated with hypoxia will lead to other symptoms like breathlessness, dizziness, and swelling. There are certain blood disorders that will also contribute to cyanosis although respiratory and cardiovascular functioning is intact.
With conditions like methemoglobinemia, oxygen cannot bind to the methemoglobin (oxidized form of hemoglobin) in red blood cells and due to a higher than normal concentration of methemoglobin, the oxygen saturation concentration of arterial blood is significantly reduced. In other conditions like sulfhemoglobinemia, sulfur binds to hemoglobin and prevents oxygen from bindng to it. Pseudocyanosis is a bluish tinge of the skin and mucous membranes that ocurs with the exposure to certain metals and drugs and is not an indication of low oxygen saturation.
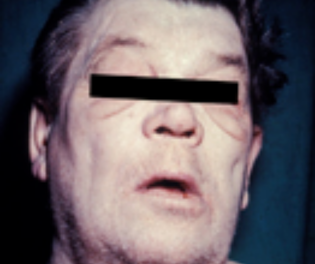
Causes of Cyanosis
There are a number of causes of cyanosis including metal toxicity, drugs and metabolic conditions like diabetic ketoacidosis. However, the more common causes arise from disorders with the respiratory or cardiovascular systems. It is a consequence of a high concentration of deoxygenated hemoglobin (greater than 5 g/dL or 50 g/L) in the arterial blood, usually with a oxygen saturation of less than 90%. If the air intake and gas exchange between the lung and blood stream is compromised, cyanosis will gradually develop as the oxygen is taken up by the body’s cells but not replenished fast enough.
Respiratory Causes
Conditions that affect the flow of air through the airways and gas exchange in the air sacs of the lung include :
- Upper airway obstruction (pharynx, larynx, trachea)
- Chronic obstructive pulmonary disease – emphysema or chronic bronchitis
- Asthma – acute attack
- Bronchiectasis
- Acute lung injury
- Acute respiratory distress
- Pulmonary edema
- Chronic interstitial lung disease
- Idiopathic pulmonary fibrosis
- Pneumonia
- Pulmonary alveolar proteinosis
- Spontaneous pneumothorax
- Lung cancer
Cardiovascular Conditions
Cyanosis in cardiac conditions may be due to various mechanisms that disrupt the blood flow through the pulmonary blood vessels thereby impairing gas exchange. Slowing of the circulation in the periphery of the body may also contribute to peripheral cyanosis.
- Acute myocardial infarction (heart attack)
- Congestive heart failure
- Congenital heart disease
- Tetralogy of Fallot
- Truncus arteriosus
- Tricuspid artresia
- Total anomalous pulmonary venous connection
- Atrial septal defect
- Ventricular septal defect
- Coarctation of the aorta
- Raynaud phenomenon
- Thrombophlebitis
- Pulmonary embolus
Cyanosis with Polycythemia and Anemia
It is the high concentration of deoxygenated blood in the skin’s blood vessels, particularly the arteries, coupled with the properties of human skin that contributes to the blue-purple skin color (cyanosis). However, with certain red blood cell disorder, cyanosis may not be present at the levels mentioned above. This applies mainly to polycythemia and anemia which are discussed under too many and too few red blood cells.
With polycythemia, the excess of red blood cells and therefore hemoglobin in circulation means that even a slight decrease in blood oxygen levels will lead to cyanosis. Patients with polycythemia can therefore become slightly cyanosed even with normal oxygen saturation. In anemia, the low hemoglobin levels means that there is insufficient hemoglobin to become deoxygenated and therefore cyanosis is rarely ever seen.
Signs and Symptoms with Cyanosis
Cyanosis is not a disease but rather a sign of deoxygenated hemoglobin in the blood. It is evident as a blue to purple discoloration of the skin and mucous membranes. With central cyanosis, this discoloration is seen on the mucous membranes lining the mouth, tongue and eyes. With peripheral cyanosis, the bluish discoloration may be seen on the hands, feet and ears and is more pronounced in cold weather.
Cyanosis may be accompanied by other signs and symptoms like :
- Breathlessness with rapid or deep breathing as the body signals the brain of low oxygen availability and the respiratory symptom responds by increasing respiration in an attempt to raise oxygen intake. In mild cases, this may only occur with exertion.
- Dizziness as the oxygen-sensitive brain tissue responds to the low oxygen availability. This may eventually progress to fainting.
- Swelling, especially peripheral edema (swelling of the legs), as the changes associated with concomitant hypercapnia (excess carbon dioxide) disrupts kidney functioning.
Other signs and symptoms that may be reported with cyanosis includes :
- Gasping / air hunger.
- Tingling or numbness of the affected areas.
- Rapid heart rate with or without elevated blood pressure.
- Easily fatigued.
- Signs of hypercapnia (excess carbon dioxide in the blood) and respiratory acidosis.
- Clubbing of the fingers and toes (hypertrophic osteoarthropathy) may occur with long-standing hypoxemia.
Last updated on August 14, 2018.