Intestinal Polyps – Types, Causes, Symptoms, Sugery, Removal
Polyps are outgrowths of tissue from the mucosal surface of a cavity. These growths are not unique to the small and large intestine and may be see anywhere in the gastrointestinal tract like esophageal and stomach polyps and also occurs within other cavities like nasal polyps in the nose and uterine polyps in the uterus.
What are intestinal polyps?
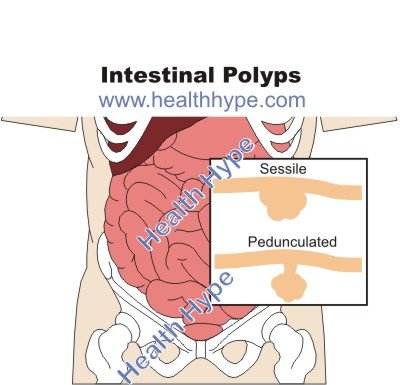
Intestinal polyps are protrusions from the mucosal surface of the intestine into the lumen. Most polyps are seen in the colon. Polyps are overgrowths of tissue and may extend along the mucosal surface (sessile) or protrude outwards into the lumen with a stalk (pedunculated). An intestinal polyp may be single or multiple and can vary in size from a few millimeters to several centimeters.
Malignant or Benign
Intestinal polyps are benign growths that can be categorized as neoplastic or non-neoplastic. Neoplastic growths occur when individual normal cells replicate independently due to genetic abnormalities and have the potential to become malignant (cancerous). Non-neoplastic polyps do not have the potential to become malignant. Neoplastic polyps of the intestine include adenomatous polyps (adenomas of the colon) and are the more common type of polyp of the intestine. Non-neoplastic polyps include inflammatory, hyperplastic, lymphoid and juvenile intestinal polyps.
Adenomas
Adenomatous polyps (colorectal adenomas) are fairly common and may occur in up to 50% of people over the age of 60 years. Only 10 to 20% of these polyps will become malignant. Adenomas can be classified by its shape – villous, tubular or tubulovillous. As the name suggest, villous adenomas are growths with multiple projections due to folding of the surface, similar to the villi seen in the small intestine. Villous adenomas secrete large quantities of mucus similar to the surrounding intestinal epithelium.
Adenomatous polyps develop when genetic damage leads to an imbalance between mucosal cell proliferation and cell death. A strong familial predisposition is seen with adenomatous polyposis syndromes. These types of polyps are very common and may occur in 50% of people over the age of 60 years. Adenomatous polyps associated with hereditary polyposis syndromes carry a significantly higher risk of colorectal cancer. Having a first-degree relative with familial polyps increases the risk for adenomatous polyps by four-fold.
Tubular Adenomas
Tubular adenomas are the most common type of adenomatous polyps accounting for about 80% of all adenomatous polyps. More than 50% of the tubular adenomas are located in the rectum and sigmoid colon and are associated with a 2% to 5% risk of cancer. Glands or cysts-like structures are usually found in the submucosa. Tubular adenomatous polyps which are smaller than 1 cm rarely become malignant.
Villous Adenomas
Pure villous adenomas are relatively rare and account for less than 5% of adenomas. These adenomas are usually sessile cauliflower-like mass, mostly confined to the sigmoid colon and rectum. Villous adenomas which are larger than 4 cm size are often associated with severe dysplasia and has a high risk of cancer. About 40% of these lesions eventually develop cancer.
Tubulovillous Adenomas
Tubulovillous type adenomas are found in 10 to 20% of the patients with adenomatous polyps. It is also known as mixed or villoglandular adenomas because it has mixed features of tubular and villous type lesions. The malignant potential of tubulovillous polyps are related to the amount of villous component of the lesions. Tubulovillous polyps have about a 20% risk for cancer development.
Non-Adenomatous Polyps
Non-adenomatous types of intestinal polyps can develop as a result of inflammation, abnormal maturation of mucosa or abnormal architecture. The non-adenomatous polyps are not as dangerous as the adenomatous polyps since most do not have the potential to become malignant (non-neoplastic). The non-adenomatous polyps can be hyperplastic, lymphoid, inflammatory, or juvenile in type.
Hyperplastic (Metaplastic) Polyps
Most of the patients with non-adenomatous polyps have hyperplastic type of polyps. Hyperplastic polyps usually result from the abnormal maturation of the mucosal cells of the intestines and are usually of small size. Hyperplastic polyps are mostly found in sigmoid colon or rectum and occur in association with hyperplastic polyposis syndrome in some patients.
Lymphoid Polyps
Lymphoid polyps are seen in association with hyperplasia (enhanced cell division) of lymphoid tissue in the intestinal mucosa. It is often benign and is seen in parts of the intestine where lymphoid tissues are concentrated like the ileum of the small intestine or rectum. Lymphoid polyps are formed of well differentiated lymphoid tissue.
Inflammatory Polyps
Inflammatory polyps are seen in patients suffering from inflammatory diseases of the intestine like ulcerative colitis or Crohn’s disease. The inflammatory polyps have areas of inflammation and ulceration. Unlike other non-adenomatous polyps, inflammatory polyps are associated with an increased risk of cancer.
Juvenile Polyps
Also known as congenital or retention polyps, these type of polyps develop in the rectum of children below 5 years of age. It is usually a result of localized abnormal development of the normal tissue. Juvenile polyps are usually found incidentally but sometimes can be found in relation to rectal bleeding or intestinal obstruction. Asymptomatic juvenile polyps do not require any therapy. Juvenile polyps can also be seen as a part of some hereditary syndromes like Peutz Jegher’s syndrome or juvenile polyposis syndrome. The latter has an increased risk of colon cancer.
Familial Adenomatous Polyposis
Familial adenomatous polyposis is characterized by development of several hundreds to thousands of adenomatous polyps in the large bowel. It is an autosomal dominant disease that usually develops at a young age (8 to 34 years of age). It results from an inherited genetic abnormality of the adenomatous polyposis coli (APC) gene located on chromosome 5.
The APC gene is a tumor suppressor gene which regulates the intestinal epithelial cell growth. When the function of this gene is lost due to a genetic abnormality, the normal growth control of the mucosal epithelium is lost and leads to development of polyps. About 30% of patients develop the APC gene mutation sporadically, without any family history.
Location of Polyps
Polyps are found throughout the large bowel in this syndrome and untreated familial adenomatous polyposis patients have a very high risk of colorectal cancer. The syndrome accounts for 1% of patients developing colorectal cancer. Almost 90% of the patients with familial adenomatous polyposis may also have polyps in stomach or duodenum. About 10% of the patients with polyps in duodenum are at risk of developing adenocarcinoma of the duodenum. The duodenal polyps close to the ampulla (ampullary polyps) are known to have high malignant potential.
Turcot’s Syndrome
Turcot’s syndrome is a variant of familial adenomatous polyposis with a strong association to brain tumors and colonic polyps. The polyps are larger but fewer in number. Majority of the patients with Turcot’s syndrome have APC gene mutations while a few have mutations in DNA mismatch repair genes like hMLH1.
Gardner’s Syndrome
Gardner’s syndrome is also a variant of familial adenomatous polyposis with similar cancer risk potential. It also results from APC gene mutation but differs from familial polyposis due to the difference in extracolonic manifestations. The extracolonic manifestations include epidermal cysts, mandibular osteomas, supernumerary teeth, soft tissue tumors (like lipomas), desmoid tumors and retinal pigment epithelial hypertrophic disorder.
Hereditary Nonpolyposis Colorectal Cancer (HNPCC)
Hereditary nonpolyposis colorectal cancer, sometimes referred to as Lynch’s syndrome, is an inherited autosomal dominant genetic abnormality that is caused by mutations in DNA mismatch repair gene. The genes commonly mutated in these patients include hMLH1 and hMSH2. These gene mutations can also lead to DNA microsatellite instability (MSI).
HNPCC is the most common type of hereditary syndrome causing colorectal cancer. About 3 to 5% of all cases of colorectal cancers are associated with HNPCC. It is usually diagnosed in the 5th decade of life. The polyps in HNPCC are predominantly found on right colon and are limited to less than 100 in number. It has an 80% risk of becoming malignant (cancerous). There is also an increased risk of cancer in the small bowel. HNPCC is often associated with other tumors like ovary, pancreas, endometrial etc.
Hamartomatous Polyposis Syndromes
The hamartomatous polyposis syndromes are rare. It includes Peutz-Jeghers syndrome, Juvenile polyposis syndrome and Cowden’s syndrome. These syndromes are associated with abnormal development of tissue and accounts for less than 1% of the colorectal cancers.
Peutz-Jeghers Syndrome
Peutz-Jeghers syndrome is a rare inherited autosomal dominant disorder. The disorder results from mutation in the serine-threonine kinase STK11 gene present on the chromosome 19. Patients suffering from the syndrome have intestinal polyps in association with some characteristic pigmentation of skin and mucosa. The syndrome is usually diagnosed in the third decade of life.
These intestinal polyps are predominantly found in the small intestine, but are not confined to it. Lesions can also be found in colon or stomach in many patients. The polyps of Peutz-Jeghers syndrome tend to have a core made of smooth muscles arising from the muscularis mucosa and hence cannot be called a true polyps.
The polyps are usually non-malignant but occasionally become malignant. The symptoms of the syndrome include bleeding and bowel obstruction. Polyps in the gallbladder, urinary bladder and nasal passages, ovarian tumors, and melanin spots on lips or oral mucosa are extraintestinal manifestations of Peutz-Jeghers syndrome.
Juvenile Polyposis
Juvenile polyposis is a rare inherited autosomal dominant syndrome. It is characterized by ten or more hamartomatous polyps throughout the small and large intestine. Juvenile polyposis has a 10% risk of colorectal cancer. It is caused by mutations in genes like the SMAD4 and PTEN. Patients usually present with rectal bleeding, anemia or abdominal pain in childhood or adolescence. Some congenital abnormalities like pulmonary arteriovenous malformations are seen with juvenile polyposis patients.
Cowden’s Syndrome
Cowden’s syndrome is a rare autosomal dominant disorder caused by genetic abnormalities in the tumor suppressor gene PTEN. The disorder is characterized by multiple gastrointestinal hamartomatous polyps which are free of malignant potential. These patients also have hamartomatous polyps of the skin and mucous membranes, papillomas in the oral cavity and keratoses of the hands and feet. Cowden’s syndrome is also associated with malignant tumors of thyroid and breast.
Signs and Symptoms
Most intestinal polyps are asymptomatic, meaning that it does not cause any symptoms. It may only be discovered upon examination for other gastrointestinal symptoms during endoscopic investigation – upper GI or colonoscopy. An intestinal polyp is more likely to cause symptoms as it increases in size. However, in some cases, even small polyps may be symptomatic. Some of the signs and symptoms include :
- rectal bleeding
- blood in stool
- change in bowel habits (diarrhea or constipation)
- abdominal pain
- fatigue
Less commonly, large polyps may lead to intestinal obstruction. Read more on blocked bowels (small and large intestine). Large polyps with long pedicles may prolapse through the anus. Villous adenomas tend to secrete copious quantities of mucus and when coupled with diarrhea, hypokalemia (abnormally low levels of potassium in the blood) may arise.
Detecting Polyps in the Intestine
Colorectal polyps may be felt during digital examination of the rectum in some patients. In the event of minor blood loss (bleeding polyp), a fecal occult blood test may confirm a the presence of blood in the stool. This is, however, non-specific for intestinal polyps and other causes of blood in the stool need to be considered.
The more accurate investigations for diagnosing intestinal polyps includes double-contrast barium radiography, flexible sigmoidoscopy and endoscopy (colonoscopy).
- Flexible sigmoidoscopy, which allows visualization of the sigmoid colon, is a useful investigation for screening for colorectal polyps and can detect 50 to 60% of polyps.
- Endoscopy is the most preferred tool for accurately diagnosing colorectal polyps as it allows simultaneous visualization and biopsy. It also allows removal of the polyps in majority of the patients along with the diagnostic procedure.
- CT-colonography, which does not require passage of any instruments through intestinal tract like in endoscopy, is emerging as a valuable alternative to endoscopic screening.
- Biopsy samples taken from polyps in patients with features suggestive of inherited syndromes should be tested for mutations. First-degree relatives should be screened for polyposis and genetic testing for familial syndromes should also be performed.
Treating Intestinal Polyps
Adenomatous polyps smaller than 0.5 cm are not usually treated. In individuals with limited number of polyps, the polyps are removed (polypectomy) during the endoscopy/colonoscopy.
Removal of Single or Multiple Polyps
The stalk of the pedunculated polyp is often cut with the help of a wire-loop or snare and the base is cauterized to prevent bleeding. Flat or sessile polyps may be removed by piece-meal snare polypectomy or by using a technique called as endoscopic submucosal resection (EMR). An EMR involves injecting fluid under the polyp, which helps to lift the lesion and thereby make for easier excision. The polyp may be removed surgically if endoscopic resection of the lesion is not possible. When numerous polyps are present polypectomy may not be practical and resection of the affected part of intestine is the preferred approach in such patients.
Follow Up After Surgery
Patients who have undergone adenomatous polypectomy are at increased risk for recurrence of adenomas and also at risk for colorectal adenocarcinoma. Such patients are usually followed up with colonoscopy in 3 years. Colonoscopy may be performed earlier in patients who had multiple large polyps while the same may be delayed as much as by 5 years in case of patients with less than 3 tubular adenomas of less than 1 cm size.
Surgery for Inherited Intestinal Polyps
In patients with familial polyposis syndromes total proctocolectomy (removal of rectum and colon) combined with ileostomy or anastomosis of ileum and anus is the primary treatment option. Patients with APC gene mutations having high-risk ampullary duodenal polyps may be treated with pylorus-sparing pancreaticoduodenectomy (removal of pancreas and duodenum) or pancreas-sparing duodenectomy (removal of the duodenum while retaining the pancreas). First-degree relatives of affected individuals should be screened with APC gene testing, followed by annual flexible proctosigmoidoscopy from the age of 12.
Patients with Peutz-Jeghers syndrome are closely monitored for any complications of the syndrome with regular physical and endoscopic examination. Large polyps or bleeding polyps are removed endoscopically. Juvenile polyposis syndrome patients with severe dysplastic polyps are treated with subtotal colectomy.
For HNPCC and related conditions, a wait and watch approach is usually taken with regular colonoscopic screening every 2 years from the age of 21 to the age of 40 and then yearly thereafter. Women with strong family history for HNPCC should also undergo screening for tumors of pelvic organs including endometrial biopsy.
Last updated on September 4, 2018.