Endocarditis (Infective and Non-Infective) Causes and Symptoms
What is endocarditis?
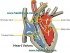
Endocarditis is the medical term for inflammation of the inner heart wall (endocardium) and heart valves. The middle muscular layer of the heart known as the myocardium may also be affected (myocarditis). When the endocardium and myocardium are both inflamed, the condition is known as endomyocarditis. Most cases of endocarditis are due to an infection, therefore the term endocarditis is almost synonymous with infective endocarditis. However, certain non-infectious causes may account for a minority of endocarditis cases.
The endocardium is the inner lining of the heart that is in contact with the flowing blood It constantly experiences wear and tear. The endocardium’s regenerative properties ensure that the endothelial lining is constantly replenished and any damage is quickly repaired. Microorganisms that may be able to enter the chambers of the heart are unlikely to attach to the inner heart lining due to the structure of the endothelium and the rapidly flowing blood.
An infection tends to arise at a site of damage on the endocardium although it can affect a normal healthy heart. Even without endocardial damage, there may be congenital defects of the heart valves. This may prove to be an ideal environment for an infection to arise should the necessary conditions be present. This damage or defect allows the causative microorganisms to adhere to the heart lining and lead to inflammation. Other disease processes not linked to an infection includes blood clots in the heart, particularly on the heart valves, either due to thrombus formation or emboli from distant sites.
Causes of Endocarditis
Infective Endocarditis
Bacteria are the most common cause of infective endocarditis. Staphylococci, streptococci and enterococci are the most common causative pathogens and may gain entry for various reasons.
- Staphylococci, particularly Staphylococcus aureus, that causes endocarditis are usually from the surface of the skin and gain entry into the bloodstream by the use of needles and catheters.
- With streptococci, spread is often from the upper respiratory tract and associated with poor orodental health. The bacteria may enter the blood stream while brushing of the teeth, chewing food and during dental procedures.
- Enterococci, particularly Enterococcus fecalis, enter via the bowels or urinary tract.
- Pneumococci seen with respiratory infections and gonococci associated with sexually transmitted infections may also be responsible for infective endocarditis.
Other causative organisms include ricketssia, chlamydia or fungi. Endocarditis may arise in patients with valvular prosthetics (heart valve replacement) and the infection may occur immediately after surgery (early onset) or a period after the procedure (late onset). Q fever (Coxiella burnetii) and brucellosis are two infectious diseases that may cause endocarditis and is associated with animal contact.
Non-Infectious Endocarditis
This type of endocarditis is not as common as infective endocarditis. It may arise as a result of trauma to the heart lining or heart valves as is seen with the insertion of a catheter into the heart. It often causes damage that can be a point for an infection to set in. Endocarditis may also be associated with other conditions like systemic lupus erythematosus (SLE) indicating an immune-mediated reaction that leads to endocardial inflammation. A similar type of inflammatory reaction may be seen with heart valve damage in rheumatic fever which is a consequence of an infection.
Various other causes, particularly those that give rise to blood clot formation, may also lead to endocarditis. In these instances non-infective endocarditis may be seen in association with a miscarriage, stroke, and other causes of thrombosis. Less frequently, it is seen with certain types of cancers, chronic infections (although the endocardium is not infected), chronic wasting diseases and disseminated intravascular coagulation.
Signs and Symptoms of Endocarditis
The clinical presentation is usually the same in both infective or non-infective endocarditis but there may be some difference in symptoms. Many cases of non-infective endocarditis are asymptomatic until the endocardium is severely inflamed or other complications arise.
- Abnormal heart sounds (murmurs)
- Easily fatigued
- Shortness of breath with activity (exertional dyspnea)
- Swelling of the lower extremities
- Malaise and weakness
- Persistent dry cough
- Unexplained weight loss
- Fever and chills
- Night sweats
- Joint pains and muscle aches
- Janeway lesions – red, painless spots on palms and soles
- Osler’s nodes – red, painful nodes on toes and fingers