Folliculitis
What Is Folliculitis?
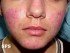
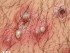
Folliculitis is an inflammation of the hair follicles, from which the hair grow. Folliculitis is not the same as acne (Picture 1). Acne primarily involve only oil (sebaceus) glands that are clogged with oil (sebum) and shed skin cells. Acne may subsequently get infected and affect the whole hair follicle, though.
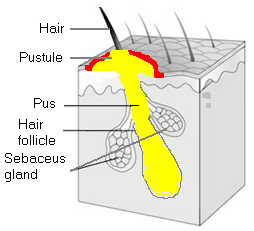 Folliculitis | 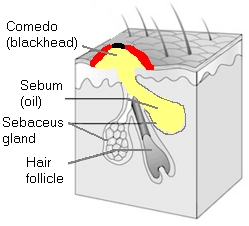 Acne |
Picture 1.In folliculitis (left), a hair follicle is inflamed;
in acne (right) a sebaceus gland is filled with oil
but the hair follicle is intact
Symptoms of Folliculitis
In folliculitis, 2-5 mm sized itchy or painful red bumps with occasional white pus-filled centres appear on the skin. A hair may still grow out from the inflamed follicle – this may help to distinguish folliculitis from other causes of skin rash. Inflamed follicles may burst, release pus and crust over.
Folliculitis most commonly appear in:
- Bearded area in men
- Scalp
- Upper trunk (chest, under breasts, in armpits)
- Buttocks
- Thighs
- Groin
Folliculitis never appears in areas without hair follicles such as palms, soles or mucous membranes.
Folliculitis Causes
A) SUPERFICIAL FOLLICULITIS
Superficial folliculitis affects only upper parts of the hair follicle.
Staphylococcal folliculitis, caused by bacterium Staphylococcus aureus
Hot tub folliculitis, caused by bacterium Pseudomonas aeruginosa
Infected acne. Treatment includes long courses of antibiotic tetracycline or vitamin A derivative isotretinoin (2).
Tinea barbae is chronic folliculitis caused by candida or other fungi. Swollen lymph nodes and fever may appear (1). Treatment is with topical antifungal or oral antifungal medication. Moisturizing creams should not be used during treatment.
Ringworm of the scalp (tinea capitis) usually results in scaling and localized hair loss, but sometimes results in folliculitis. In New Zealand, cat ringworm (Microsporum canis) is the commonest organism causing scalp fungal infection. Other organisms such as Trichophyton tonsurans are increasingly reported. Treatment is with oral anti-fungal agents for several months (2).
Pseudofolliculitis barbae or ingrown hair affects men with curly beards. After shaving, short hairs may curve back into the skin resulting in inflammation, and, in rare cases, dark raised scars (keloid scars) on the face and neck (1). Shaving with an electric razor that does not cut as closely as a razor blade does can help. If you use a blade, massage your beard area with a warm, moist washcloth or facial sponge to lift the hairs so they can be cut more easily. Use a shaving gel instead of cream and shave in the direction of the hair growth. When you are finished, rinse the face thoroughly with warm water and apply a moisturizing after-shave. If these measures do not help, you can ask your doctor for acne medication tretinoin (Retin-A).
Pityrosporum (malassezia) folliculitis is a fungal infection commonly affecting young adults. It produces chronic, red, itchy pustules on the back and chest and sometimes on the neck, shoulders, upper arms and face (1). Malassezia fungi are present on the skin of most adults (2) without causing any symptoms, but they may overgrow in pregnancy and during taking oral contraceptives. Treatment is with oral anti-fungal medications. Topical treatment is with antidandruff shampoo, ketoconazole or ciclopirox creams, or econazole foaming solution. Oral medications include ketoconazole, itraconazole and isotretinoin (2).
Herpetic folliculitis. Shaving through a cold sore (caused by Herpes simplex virus) can spread the herpes infection to adjacent hair follicles. If you are a healthy adult, herpetic folliculitis may clear without treatment in 7 to 10 days. Patients with AIDS and those frequently having cold sores can be treated with an oral antiviral medication such as acyclovir, famciclovir or valacyclovir. Although these drugs can clear the infection, they will not necessarily prevent it from recurring.
B) DEEP FOLLICULITIS
Deep folicullitis affects the entire hair follicle and surrounding skin.
Boils or furuncles occur when hair follicles become deeply infected with staph bacteria. A boil usually appears suddenly as a painful pink or red bump about 1/2 inch in diameter. The surrounding skin may be red and swollen. Within 24 hours, the bump fills with pus. Boil grows larger and more painful for five to seven days, sometimes reaching a golf ball size before it develops a yellow-white tip that finally ruptures and drains pus. Boils generally clear completely in about two weeks. Small boils usually heal without scarring, but a large boil may leave a scar. A carbuncle is a cluster of boils often occurring on the back of the neck, shoulders or thighs, especially in older men. Carbuncles cause a deeper and more severe infection than does a single boil, heal more slowly and tend to leave scars (1). Your doctor may drain a large boil or carbuncle by making a small incision in the tip. This relieves pain, speeds recovery and prevents scarring. Deep infections that cannot be completely cleared may be covered with a sterile gauze so pus can continue to drain. Sometimes your doctor may prescribe antibiotics to help heal severe or recurrent infections.
Eosinophillic folliculitis. Seen primarily in persons with AIDS, this type of folliculitis is characterized by recurring patches of inflamed, pus-filled sores on the face, back or upper arms. Sores may itch intensely and often leave areas of darker than normal skin (hyperpigmentation) when they heal. The exact cause of eosinophilic folliculitis is not known, although it may involve the same yeast-like fungus responsible for pityrosporum folliculitis (1,8). Treatment is with topical or oral corticosteroids and antihistamines. Severe folliculitis may require treatment with isotretinoin (Accutane) for several months (1,8).
Gram negative folliculitismay develop in people receiving long-term antibiotic treatment for acne. Antibiotics alter the normal balance of bacteria in the nose, leading to overgrowth of harmful gram-negative bacteria that may spread to cheeks and jaw area (1,7).
Folliculitis may appear after smallpox vaccination.
Folliculitis may appear in inflammatory skin diseases, like lichen planus, discoid lupus erythematosus and folliculitis decalvans. Treatment depends on the underlying condition. A skin biopsy is often necessary for diagnosis (2).
Occlusive folliculitis. Paraffin-based ointments, moisturisers, and adhesive plasters may all result in a occlusive folliculitis. If you need a moisturiser, choose an oil-free product.
Overuse of topical steroids and moisturizing creams may result in perioral dermatitis. Treatment is with tetracycline antibiotics for six weeks or so (2).
Oil or chemical folliculitis. Sterile acne or folliculitis, caused by oil, commonly affect forearms or thighs of road workers, mechanics, refinery workers, and sheep shearers. Skin washing, clothes changing and standard acne treatment usually helps (6).
Scalp folliculitisoften occurs on the front hairline of the scalp. Yeasts, bacteria or mites may be the cause. Antidandruff shampoos containing antifungal agents such as ketoconazole or ciclopirox are sometimes helpful. The following medications may be helpful:
- Topical antibiotics e.g. fucidin gel, clindamycin solution, erythromycin solution
- Mild topical steroid lotions or creams
- Oral antihistamines
- Oral antibiotics, particularly long term tetracycline
- Oral isotretinoin; long term low dose treatment may be required (4)
Tuffted hair folliculitis (folliculitis decalvans). Rounded or oval patches of hair loss appear on the scalp or in any other hairy area. Several hairs grow from one hair follicle. The cause is not known. Treatment with oral antibiotics, steroids or isotretionine might be worth to try (3).
Pruritic folliculitis of pregnancy is rare and occurs in 2nd or 3rd trimester of pregnancy, usually on the trunk.
Folliculitis keloidalis is rare and usually affects the nape of the neck. Inflamed follicles form scars, which may further develop into keloids.
Diagnosis of Folliculitis
Folliculitis is usually recognised by a primary doctor without any test. In doubtful cases, swabs or biopsies of skin lesions are taken and sent to pathological laboratory.
Is Folliculitis Contagius?
Staphylococcal folliculitis is very contagious; other types usually are not. It spreads by direct skin to skin contact, or by sharing razors, towels or sport equipment, mostly in athletes.
Skin Lesions Resembling Folliculitis
Some other diseases may resemble folliculitis
- Goose bumps
- Heat rash
- Smallpox
- Chicken pox
- Rubella
- Measles (rubeolla)
- Herpes simplex; labial HSV ; generalised HSV
- Herpes zoster
- Urticaria (in allergy)
- Dermatitis
- Steroid acne
Related Articles:
- Types of Skin Rashes with Pictures
- Causes of Itchy Skin
References:
- Tinea barbae (mayoclinic.com)
- Pytirosporum (malassezia) folliculitis (dermnetnz.org)
- Foliculitis decalvans (dermnetnz.org)
- Scalp folliculitis (dermnetnz.org)
- Folliculitis keloidalis (dermnetnz.org)
- Oil folliculitis (dermnetnz.org)
- Gram-negative folliculitis (dermnetnz.org)
- Eosinophilic folliculitis (dermnetnz.org)