Infection and Incubation Period Meaning
What Is Infection?
An infection is an invasion and multiplying of pathogenic microbes in the body tissues in which they are not usually present (1). Pathogenic means capable of causing disease. Infection does not always cause a disease.
Definitions of Infection-Related Terms
A colonization is the usual presence of non-pathogenic and even potentially pathogenic microbes on the skin, in the nose, mouth, bowel, penile or vaginal mucosa, as a part of normal human flora, in the amount not harmful for the body – this is not an infection. An example is the presence of Lactobacilus acidophilus bacteria in the colon.
A contamination is the presence of germs which do not multiply, for example, in a contaminated (not infected)wound. Infected or septic wound contains multiplying microbes. Contamination also refers to presence of pathogenic microbes on medical equipment, in the water, food etc.
A carrier state is the non-usual presence of pathogenic microbes in the body, in the way not harmful for the carrier, but potentially dangerous for others, since the carrier is usually contagious. For example, if you have Staphylococcus aureus bacteria (a common cause of skin infections) in your nose, you may infect others, even if you alone never develop an infection.
An overgrowth of microbes, non-pathogenic in small amount, but pathogenic in large amount, for example, an overgrowth of Clostridium difficile bacteria in the colon can cause life threatening pseudomembranous colitis. Small intestinal bacterial overgrowth due to invasion of otherwise non-harmful colonic bacteria into the small intestine can cause bloating and diarrhea.
Re-activation of an infection may occur; for example, a Varicella zoster virus, which has remained dormant in the roots of the spinal nerves after successfully healed chicken pox, may be re-activated during stress or certain disease, and can cause shingles.
Bacteremia, viremia, fungemia and parasitemia (the presence of microbes in the blood) may result in an infection of other organs, or sepsis.
Types of Infection
Systemic infection, like influenza, affects the whole body and causes systemic symptoms, like general malaise, muscle pains, fever, nausea, etc.
Localized infection, like cellulitis, is limited to one or few body parts and presents with localized symptoms, like redness, swelling, pain or localized (nasal, ear, etc.) discharge.
Acute infection, like common cold, appears suddenly and lasts from few days to one month.
Chronic infection, like tuberculosis or AIDS, may last from several weeks to several years.
Recurrent infection is one that frequently affects a person, like folliculitis in those who share the same sport equipment, or fungal infections in those with lowered immunity.
Asymptomatic infection causes no symptoms. Example: infection with Epstein-Barr virus (EBV), which can cause infectious mononucleosis, often triggers no symptoms in small children.
Causes of Infections
Infections are caused by microbes:
- Bacteria, like Staphylococci, Salmonella, Mycoplasma, Ricketssiae
- Viruses, like virus influenzae or HIV
- Fungi, like one-cell yeasts Candida albicans or Aspergillus
- One-cell parasites (protozoa), like Giardia or Entameba histolytica
Invasion of multi-cellular parasites, like intestinal worms or head lice, into the body is called infestation.
Bacterial infections are usually limited to one part of the body. Examples of bacterial infections: staphylococcal skin infections, pseudomonas folliculitis, streptococcal pharyngitis, osteomyelitis, pneumococcal pneumonia, bacterial meningitis, etc. (Picture 1). Bacterial infections can be treated by antibacterial drugs – antibiotics. Example of a systemic bacterial infection is bacterial sepsis.
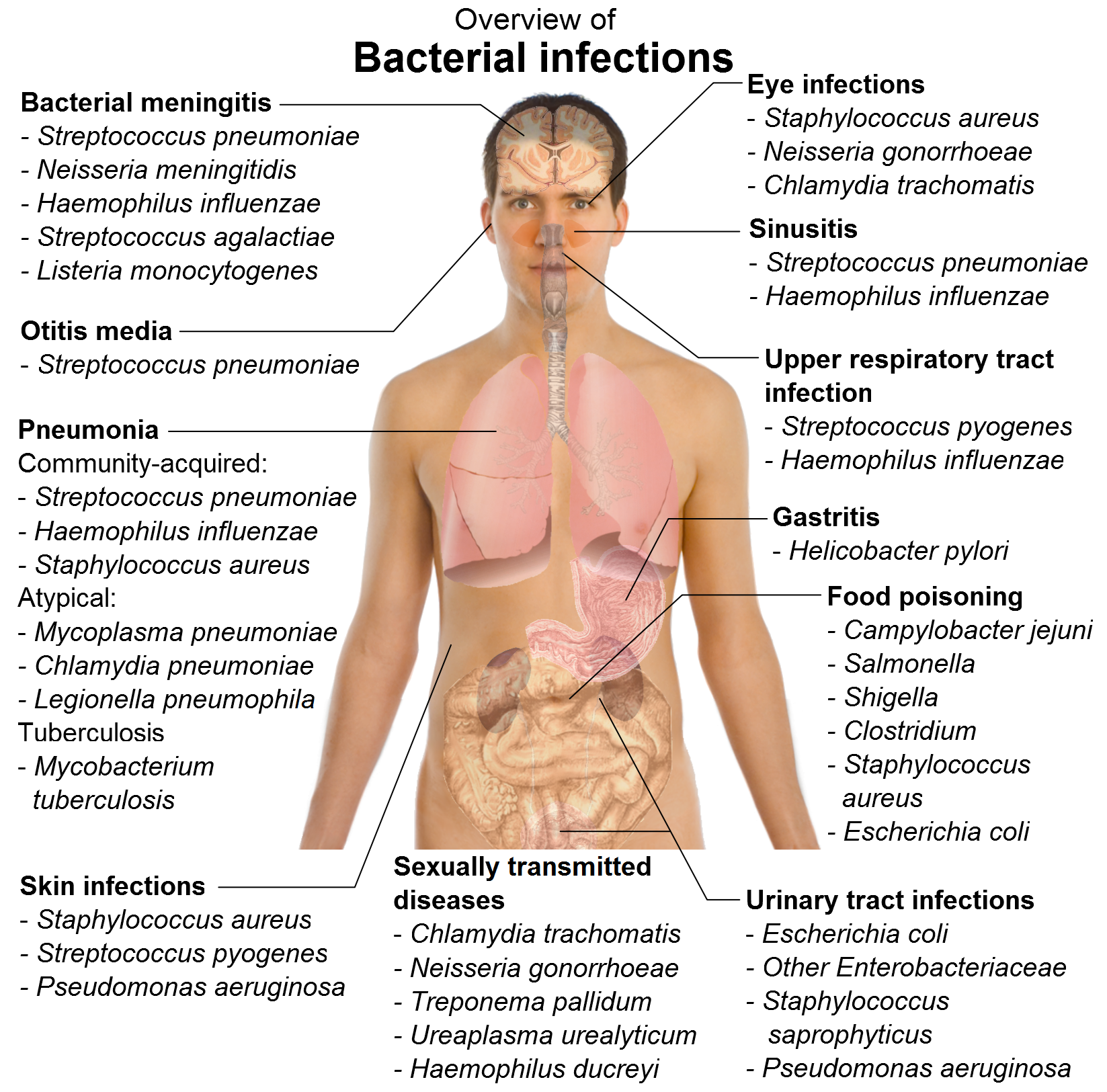
Picture 1. Bacterial infections and causing bacteria
(source: Wikimedia)
Viral infections are often systemic and may cause fever, headache, runny nose, sore throat, muscle and joint pains, diarrhea, skin rash, etc. (Picture 2). Examples of viral infections: influenza, childhood diseases like chicken pox, rubella, rubeolla and infectious mononucleosis, AIDS, viral hepatitis, viral hemorrhagic fever, etc. Examples of a localized viral infection are common cold and labial herpes. Except of acyclovir and related antiviral drugs, at present, there is not a lot of effective medicines for viral diseases available.
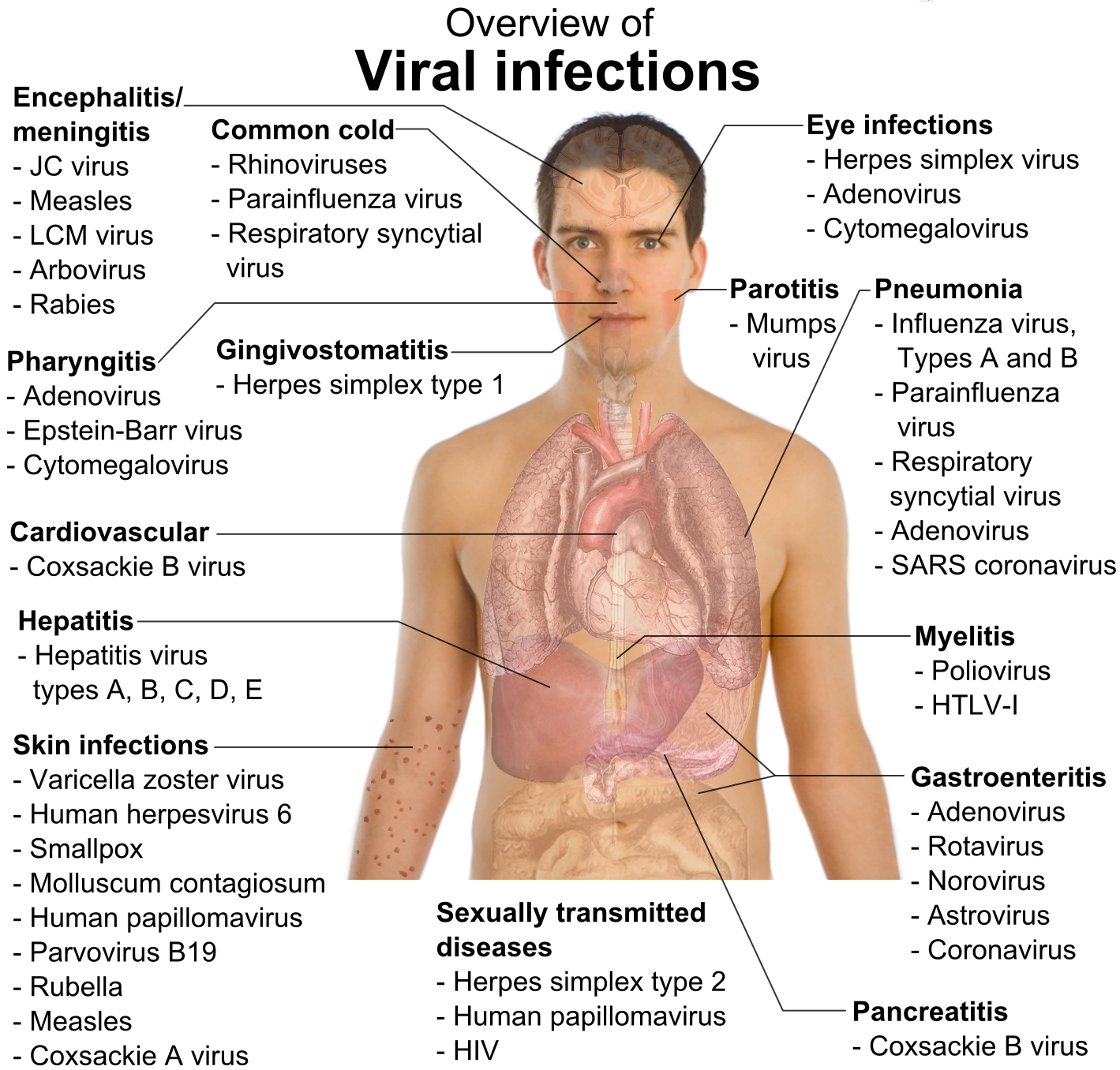
Picture 2. Viral infections
(source: Wikimedia)
Fungal (yeast) infections in a person with a healthy immune system usually affect only the skin. Patchy areas with a brownish or reddish scaly rash on the scalp (scalp ringworm), trunk, limbs or groin (jock itch), peeled skin on the hands or feet (athlete’s foot), or discolored or cracked nails are typical symptoms of a skin fungal infection. Effective over the counter or prescribed anti-fungal ointments and oral medications are available.
In a person with a weak immune system, fungal infections, commonly caused by a yeast Candida albicans, may appear in the mouth (oral thrush), esophagus, rectum or vagina; systemic candidiasis is severe and commonly fatal infection.
Parasitic infections cause different symptoms, depending on the type of parasite and organ affected. Intestinal parasites cause bloating, diarrhea, mucus in the stool and eventual weight loss. Plasmodium malariae can cause episodes of fever, chills sweating and tiredness. Head and pubic lice, and scabies cause itchy skin. Treatment is with specific anti-parasitic drugs. Surgical removal of parasitic cysts, like in Echinococcus, from the liver, bones, brain or lungs is sometimes required.
Infestation (Latin infestare = to attack, disturb) is an invasion of multi-cellular parasites, like intestinal worms (helminths) or head lice to the body. Effective anti-helminthic and other specific anti-parasitic drugs are available.
What is incubation period?
In medical terms, the incubation period is the time from when a person is exposed to an infectious agent (pathogenic microorganism) till the onset of signs and symptoms. Not every person who comes into contact with an infectious agent will become infected but once the infection is acquired, the micoorganism will take a period of time during which it multiplies and spreads within the body until the point that signs and symptoms become evident.
Why do incubation periods differ?
Incubation periods can vary significantly for a number of reasons. This includes :
- Method of transmission.
- Site of entry.
- Immune response.
- Reproduction mechanism of infectious agent.
- Action of infectious agent.
- Nature of the disease.
Incubation Periods of Some Infections
Incubation periods are approximate and may vary slightly. Refer to the guidelines from the health department in individual countries.
| DISEASE | INCUBATION PERIOD |
| Amoebiasis | 1 to 4 weeks |
| Anthrax | 9 hours to 2 weeks (direct contact through the skin) or approximately 2 days (inhalation) |
| Bird Flu (Avian, H5N1 Influenza) | 2 to 17 days |
| Brucellosis | 5 to 30 days |
| Chickenpox | 11 to 20 days |
| Cholera | 2 hours to 5 days |
| Dengue Hemorrhagic Fever | 3 to 14 days |
| Diptheria | 1 to 10 days |
| Ebola Hemorrhagic Fever | 2 to 21 days |
| Gonorrhea | 2 to 10 days |
| Hepatitis A | 3 to 7 weeks |
| Hepatitis B | 6 weeks to 6 months |
| Influenza (Seasonal) | 1 to 3 days |
| Lassa Fever | 3 to 21 days |
| Leishmaniasis | Weeks to months (cutaneous) Months to years (visceral) |
| Leprosy | 5 to 20 years |
| Malaria | 10 to 15 days |
| Measles | 6 to 19 days |
| Meningococcemia | 2 to 10 days |
| Mumps | 15 to 24 days |
| Poliomyelitis | 3 to 35 days |
| Psittacosis | 1 to 4 weeks |
| Rabies | 2 to 8 weeks |
| Rubella | 15 to 20 days |
| Rift Valley Fever | 2 to 6 days |
| SARS | 2 to 7 days |
| Scarlet Fever | 2 to 4 days |
| Swine Flu (2009 H1N1 Influenza) | 2 to 7 days |
| Trypanosomiasis | Months to years |
| Tuberculosis | 1 to 12 months |
| Typhoid | 5 to 31 days |
| Whooping Cough | 5 to 21 days |
Symptoms and Signs of Infections
Symptoms commonly appearing in all types of infections:
- Fever in localized skin infections or food poisoning may be absent, in tuberculosis or viral pneumonia it is usually low-grade, in influenza moderate, and in bacterial pneumonia or sepsis high.
- Pain in childhood viral infections and flu is usually general and vague, and in localized bacterial infections, like bacterial prostatitis, localized and intense.
- Headache in sinusitis is facial, in meningitis on the back of the head and neck, and in viral infections general
- Skin rash in bacterial skin infections is usually in the form of red bumps or patches; in viral infections, blisters and in fungal skin infections, scaly discolored patches usually appear
- Discharge from the nose, eyes, ears, trachea, bronchi and lungs (phlegm, sputum), nipples, bowel (mucus in the stool), urethra, vagina and wounds may appear in all types of infections.
NOTE: Any of above symptoms can appear in other conditions, like poisoning, allergies, etc., and not only in infections. There is no single specific symptom but a combination of symptoms and signs that speak for an infection.
Sources and Modes of Transmission of Infection
Terms explained:
- Being contagious means being capable of carrying microbes or spreading an infection. In everyday speech, only infections transmitted directly from person to person (like flu) are considered as contagious.
- A term contaminated is used for soil, water, food and surfaces that carry microbes.
- An incubation period is the time elapsed between exposure to pathogenic microbes and symptoms appearance.
Sources and modes of transmission of infection are listed below.
1. Person-to-Person Spread
Infection can be transmitted from person to person by:
- Skin-to-skin contact, clothes, towels, sport equipment, etc. (staphylococcal, including MRSA skin infections, like folliculitis; scabies, head lice)
- Droplets during coughing, sneezing (common cold, flu, swine flu, pneumonia, tuberculosis, bacterial meningitis, chicken pox, measles, rubella, mumps), or kissing (infectious mononucleosis, cold sores)
- Stool-to-mouth (fecal-oral) spread, usually via dirty hands or utensils (stomach flu, hepatitis A, Giardia, pinworms, Clostridium difficile, cholera, poliomyelitis)
- Sexually transmitted (gonorrhea, Chlamydia, genital herpes, pubic lice, genital warts (human papillomavirus – HPV), AIDS, syphilis)
- Blood-to-blood contactby:
- contaminated needles, usually by drug addicts or health workers (hepatitis B, C, AIDS)
- blood transfusion (hepatitis B,C, AIDS, viral hemorrhagic fevers)
- mosquitoes (malaria)
- Spread from mother to fetus during pregnancy (hepatitis B, C, AIDS, HSV-1, HSV-2, rubella, parvovirus, toxoplasma, varicella, syphilis, bird flu), or delivery (Chlamydia trachomatis, Neisseria gonorrheae, CMV, group B Streptococci)
- An autoinfection – the spread of an infection from one body part to another, usually by hands or clothes (folliculitis, impetigo).
2. Food-Borne Infections
- Food poisoning is an infection of the gastrointestinal tract caused by microbes from contaminated food: bacteria, like Salmonella or E.coli, toxins from Staphylococcus aureus or Clostridium botulinum, parasites like Giardia or roundworm, viruses, like Enterovirus.
3. Waterborne Infections
- By drinking contaminated water, one can contract stomach flu, cholera, dysentery, typhoid fever, amebiasis, etc. Tap water in newly opened hospitals may contain Legionella.
- By swimming in contaminated swimming or spa pools, or lakes, one can contract hot tub folliculitis, intestinal parasite Cryptosporidium, eye and middle ear infections. Certain parasites may enter through the skin.
- Water in public showers may hold Legionella; the floor may be contaminated by Staphylococci (from human skin infections)
- Flood water may contain various pathogenic microbes.
4. Airborne Infections
- Industrial cooling or hot water systems, air condition and room-air humidifiers can be a source of Legionella.
5. Soil
- During walking barefoot, Clostridium tetani, sandworms, or intestinal parasites, like Strongyloides stercoralis or hookworms can be contacted.
- Eating with soil-contaminated hands can also result in infection by parasites.
6. Hospital Acquired Infections (HAIs)
Infections acquired in hospitals can be dangerous, since causing microbes are often resistant to regular antibiotics, and patients infected are often already seriously ill. Common HAIs include:
- Urinary tract infections from urinary catheters
- Surgical-site infections
- Staphylococcal skin, lung and heart valve infections
- Fungal infections, like oral thrush in patients with low immunity system or cancer patients receiving chemotherapy
- Legionella may be sometimes found in the tap water in newly opened or poorly maintained hospitals.
What Is a Fomite?
A fomite is an inanimate object or substance capable of transmitting infectious agents (microorganisms) from one object to another. Once contaminated, fomites may carry microbes for few minutes or several weeks, depending on the type of the microbe and certain circumstances, like air humidity and temperature. Examples of fomites:
- Door knobs
- Faucets, especially in public toilets
- Bus handles
- Computer keyboards
- Phones
- Eating utensils or dishes
- Towels
- Napkins
- Used razors
- Used needles (drug addicts)
- Pens
- Sport equipment
- Clothes
- Toys
- Books
- Paper
- Money
Mechanism of Infection
Microbes may make harm by releasing toxins, for example, in food poisoning, a parasite Entameba hystolytica can release toxins, which can destroy colonic mucosa, resulting in bleeding ulcers and diarrhea.
Invasion of microbes triggers immune response of the body and attracts inflammatory cells, like leukocytes, and substances, like cytokines, which attack the microbes. Such a defense reaction regularly results in an inflammation of infected tissue, which can be observed, for example, as purulent discharge in common cold or swollen joint in bacterial arthritis. Toxins released by microbes often trigger fever.
Inflammatory response itself can be harmful. For example, Streptococcus pneumoniae , causing pneumonia, can trigger fluid collection in the lungs, impeding oxygen exchange between the air and the blood and thus reducing the oxygen supply to the tissues, what may result in death.
Infection Diagnosis
A cause of an infection can be often recognized from a combination of symptoms and signs. When in doubt, a doctor can take a sample of blood, urine, stool, sputum, nasal or other discharge and send it to laboratory, where microbes can be determined by serologic tests or a culture.
Infection Treatment
Effective anti-microbial medications for most infections, except viral ones, are available.
References:
- Definition of infection (biology-online.org)
