Inflamed Parotid Gland (Parotitis) Causes, Symptoms, Treatment
Salivary glands are responsible for producing and secreting saliva. This fluid is responsible for moisturizing the mouth cavity, lubricating chewed food as it passed down the throat and it may also contain digestive enzymes to help chemically breakdown food. The parotid gland is the largest salivary gland, located on either side of the face. Like any part of the body, it can become injured, diseased and inflamed.
What is Parotitis?
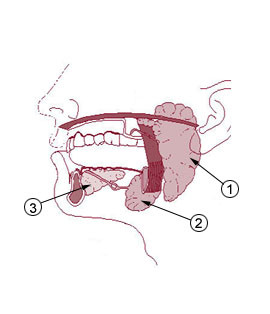
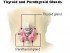
Parotitis is the term for inflammation of the parotid gland. These glands ((refer to gland 1 on diagram below) are located near the angle of the jaw and just below the ear. Symptoms are usually localized to this area, either on one side or both sides of the face. Most acute cases are due to an infection, particularly bacterial or viral, whereas chronic cases may be due to various other causes like an infection, autoimmune disorders, medication or even tumors.
Parotitis may arise on one or both sides (unilateral or bilateral). It may result in swelling of the parotid gland, dry mouth, drooling and pain. There are various causes of parotid gland swelling or enlargement that may not be related to inflammation. Therefore a swollen parotid gland may not always be parotitis and all the possible causes need to be investigated.
Read more on swollen salivary glands.
Causes of Parotitis
The causes of parotitis can be divided into infectious and non-infectious causes. Most infections are acute but chronic parotitis may be associated with underlying factors like immune deficiency and malignancies. Any condition that affects the parotid gland like salivary stones or narrowing of the salivary duct can lead to parotitis for various reasons. Sometimes parotid gland inflammation can arise for unknown reasons.
Infections
Most infectious cases of parotitis are due to bacteria or viruses. Fungal infections are extremely rare and more likely to be seen in HIV infection and less frequently in uncontrolled diabetes mellitus. Infectious parotitis can be acute, where it arises suddenly and is short lived, or parotitis can be chronic, where it is persistent or recurring.
Acute bacterial parotitis is the more common infectious causes of parotid gland inflammation. It is often associated with acute causes of mouth dryness, particularly with dehydration, or may arise as a complication of an orodental condition. These bacteria, Staphylococcus aureus, is one of the more common causes of bacterial parotitis.
Chronic bacterial parotitis is more common in the elderly, with the use of chronic medication that causes a pronounced dry mouth, It s also more likely to affect people with a weakened immune system, like HIV positive patients and diabetics. In the chronic setting, it is more often a case of recurrent bacterial infections rather than a persistent infection. Tuberculosis (TB) may also be a cause of long term infectious parotitis.
Mumps is the most common viral cause of parotitis and is usually acute. Although once considered as a common childhood disease, it is seen less frequently with the introduction of immunization in children. Parotitis associated with mumps is typically acute in nature. However there are cases where parotitis arises with mumps-like symptoms occurs repeatedly. The exact cause of this type of chronic parotitis is not known.
Trauma
Injury to the parotid gland may be either mechanical or chemical. Mechanical trauma may be seen with a blow especially if there is a fracture of the mandible, following surgery to the mouth or face and with certain dental procedures. Chemical trauma is more often drug induced where certain medication is toxic to the parotid gland tissue. Alcohol abuse may also be a cause although enlargement of the parotid gland may be unrelated to inflammation in long term alcoholism.
Autoimmune
Autoimmune parotitis is due to the action of the body’s immune system against the parotid gland tissue. It may be related to Sjogren’s syndrome where other glands and tissues are also involved, leading to characteristic symptoms like dry mouth, dry eyes and conjunctivitis (inflammation of the conjunctiva of the eye) along with parotitis. Not every case of autoimmune parotitis is associated with Sjogren’s syndrome but the disease process affecting the parotid gland is often the same.
Other Causes of Parotitis
- Salivary stone (sialolithiasis)
- Medication
- Tumors
- Salivary duct defects or strictures
- Eating disorders like bulimia
- Certain spicy food
- Psychological stress
- Excessive caffeine intake
Signs and Symptoms
The parotid gland is one of the major contributors to saliva in the mouth. This is achieved by nerve impulses to the salivary gland as well as pressure on the gland by the muscles of the face during chewing. As with any organ, inflammation can cause pain, swelling, heat, redness and affect functioning. The heat and redness may not be detectable with parotitis. However, the following symptoms are often present:
- Swelling on one or both sides of the face.
- Pain and/or tenderness on the affected side.
- Mouth dryness due to the reduced saliva.
- Headache may or may not be present.
- Fever, in the event of an infection.
- Enlarged local lymph nodes depending on the cause like swollen neck lymph nodes.
Read more on one side facial swelling.
There may also be other symptoms like loss of appetite, difficulty swallowing and malaise. However, mild cases may present with very minimal symptoms. It is important to note that there are many salivary glands apart from the parotid gland. These other salivary glands, like the submandibular and sublingual glands, can therefore compensate for reduced saliva production when both parotid glands are affected. There are also hundreds of small salivary glands (minor salivary glands) that are also present in the mouth cavity.
Treatment of Parotitis
The choice of treatment for an inflamed parotid gland depends on the underlying cause. However, there are certain measures that may provide symptomatic relief irrespective of the causative condition. These measures may include:
- Drugs to relieve pain and inflammation like NSAIDs (non-steroidal anti-inflammatory drugs).
- Drugs to promote saliva secretion (sialogogues).
- Gentle massage of the gland.
- Hydration (drinking more water).
The degree of symptomatic relief may vary. The underlying cause of parotitis must be treated and the symptoms will subsequently resolve. For example, antibiotics are prescribed to treat bacterial parotitis while corticosteroids may be used for autoimmune causes. Surgery is not usually necessary for parotitis but may be considered for chronic cases where there are repeated episodes.