Morphea (Hardened Skin Disease)
Definition
Morphea is a rare condition where patches of thick, hardened and discolored patches occur on the skin. Morphea also spelled as morphoea is a form of localized scleroderma, an autoimmune condition of the connective tissue of the body. In morphea, it is only the skin that is affected whereas in other forms the blood vessels, muscles and even internal organs are involved. Although morphea in some cases can affect the flexibility of joint at the affected areas, it does not cause any other significant complications about from aesthetic impact. Morphea is incurable but can sometimes resolve on its own without any treatment.
Pathophysiology
Fibroblasts are a type of cell in the body that is responsible for producing components of connective tissue like collagen. These structures give strength and flexibility to different parts of the body. Fibroblasts may remain in an inactive stage, where it is referred to as fibrocytes. When stimulated, it becomes active and plays an important role in restoring the connective tissue that may be weakened or damaged. Fibroblasts play an essential role in wound healing.
Connective tissue is present throughout the body. It is an important component in providing support and strength for other types of tissue and organs in the body. In conditions like scleroderma, the connective tissue can be affected at many sites throughout the body. Collagen is overproduced and this leads to a thickening that can affect the surrounding tissues and organs. Systemic scleroderma means that sites throughout the body is affected. Localized scleroderma means that only certain sites in the body are affected.
Morphea is a type of localized scleroderma where only the skin is affected. It mainly occurs on the limbs. The build up of collage occurs in the skin or the tissue just under the skin known as the subcutaneous tissue.The production of collagen by fibroblasts is a carefully regulated process. Fibroblasts are stimulated by certain factors like with tissue injury. In morphea, it is unclear as to exactly what causes the stimulation of collagen production. It is possible that the immune system attacks healthy tissue and the resulting injury then stimulates the fibroblasts into action.
Furthermore certain chemicals and hormones can stimulate fibroblast activity and these substances may be abnormally secreted as part of some disease process. The problem may then not lie with the fibroblast itself but rather the factors that regulate the activity of fibroblasts.
Symptoms
The symptoms of morphea are mainly present on the skin but in some cases of morphea there are other symptoms that do not involve the skin. However, morphea is differentiated from other types of localized scleroderma by its skin symptoms which include :
- Linear or oval-shaped patches on the skin.
- Hardening and thickening of the skin leading to the visible patches.
- Discolored patches that may be lighter or darker in color. Oval patches usually have a lighter center which may even be white in color. Even if the skin returns to normal, the discoloration may still persist.
- Loss of hair on the patches and lack of sweating at these sites.
Other symptoms that may be seen in morphea beyond the skin includes :
- Fever
- Enlarged lymph nodes (lymphadenopathy)
- Joint pains (arthralgia)
- Fatigue
- Headaches
- Seizures
These extracutaneous symptoms (outside of the skin) are not always present in morphea.
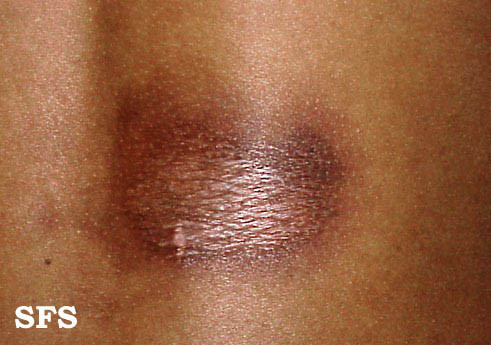
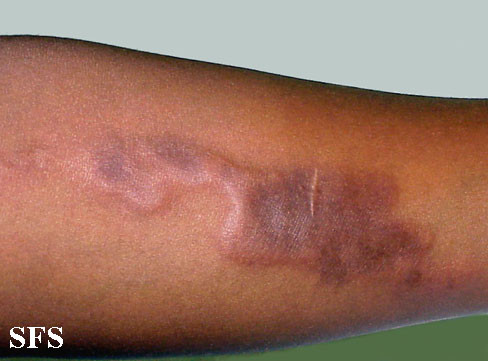
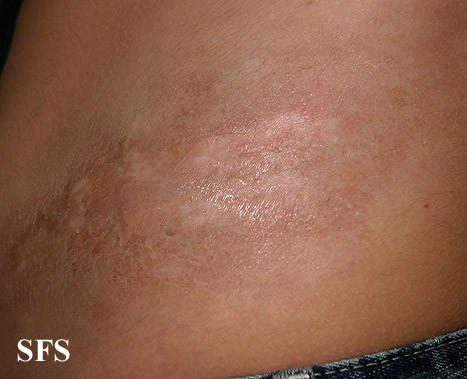
Pictures
Morphea pictures sourced from Dermatology Atlas Brazil, courtesy of Samuel Freire da Silva, M.D.
Types
Based on the appearance and location of the lesions, morphea can be distinguished into different types.
Circumscribed morphea
- Three or less separate patches localized to one part of the body.
- Mainly oval patches that are between 1 to 20 cm in diameter.
- Superficial or deep circumscribed morphea are the more common variants.
- Less common variants of circumscribed morphea include guttate, keloidal (nodular) and bullous morphea.
- Seen mainly on the trunk, and in particular on the hips and breasts.
Generalized morphea
- Widespread and severe form.
- Four or more patches on two or more regions of the body.
- Lesions are larger than 3 mm.
- Patches are dark to silvery in color.
- Rare cases can involve almost every part of the body from head to toe.
Linear morphea
- Lesions are elongated streaks.
- More commonly occurs on the limbs but can affect the trunk, face or scalp.
- Thickening is deep within the skin, involving anywhere from the dermis and underlying fat to as deep as the muscles and bones.
- Can affect the nerves and brain presenting with neurological symptoms.
Pansclerotic morphea
- Seen mainly in children.
- Extends from the bone to the dermis of the skin.
- Can affect the entire body although the fingertips and toes may be spared.
- Very debilitating form of morphea.
- Leads to the formation of contractures and ulcers.
- May be linked with squamous cell carcinoma.
Mixed morphea
- Occurs in about 15% of morphea patients.
- Combination of two or more types of morphea.
Causes
The exact cause of morphea is unknown. It is believed to be due to a genetic predisposition which may be familial. The onset of the disease may be determined by environmental factors which act as a trigger. It appears that morphea is an autoimmune condition whereby the body’s immune defenses are directed at its own tissue. The blood vessels seem to be the most likely site that is affected and the injury then prompts the formation of scar tissue. Overactivity of fibroblasts leads to overpoduction of collagen that appears as the thickened and hard indurations seen in morphea.
Triggers and Risk Factors
Although the exact triggers and risk factors have not been conclusively identified, morphea appears to arise with or following :
- Trauma. Localized injury to the skin including injections.
- Radiation exposure.
- Certain drugs like antibiotics such as bleomycin.
- Tick bites as is seen with contracting Lyme disease (Borrelia burgdorferi infection).
- Viral infections – measles, chickenpox, hepatitis B and Epstein-Barr virus.
- Vaccinations – BCG, MMR, tetanus.
- Pregnancy
- Other autoimmune diseases.
- Family history of morphea.
Diagnosis
A physical examination with the characteristic appearance of the hard indurations should warrant further investigations to confirm a diagnosis of morphea. A skin biopsy should be conducted to verify the thickening of collagen. Blood tests are useful to detect the presence of antibodies directed at the body’s own tissues (autoantibodies). Scans such as an ultrasound or MRI (magnetic resonance imaging) determines the depth of the thickenings and can identify any involvement of deeper structures and internal organs.
Treatment
Morphea can resolve on its own within months although there may be some degree of skin discoloration. There is no specific treatment for morphea and mild cases may be left untreated. At most topical corticosteroids may be prescribed to reduce the fibroblast activity at the site. There are several other treatments that may be considered for more severe cases. Most of these treatments have severe side effects and the implementation of these measures have to be carefully weighed out before it is commenced.
- Oral corticosteroids along with topical steroid treatment reduces immune activity.
- Topical tarcolimus is an immunosuppressant but the exact way in which it works is not clearly understood.
- Topical calcipotriene is a synthetic form of vitamin D that reduces inflammation and inhibits the action of fibroblasts.
- Oral chloroquine and hydroxychloroquine are antimalarial drugs that reduce inflammation and helpful for slowing the progression of the disease.
- Oral or parenteral methotrexate reduces inflammation and suppresses immune activity.
- Phototherapy (light therapy) using ultraviolet (UV) light to ease the severity of the condition.
References :
dermnetnz.org/immune/morphoea.html
emedicine.medscape.com/article/1065782-overview
www.mayoclinic.com/health/morphea/DS00718