Nerve Injury (Neuropraxia, Axonotmesis, Neurotmesis) and Healing
Acute nerve injuries are very common and may be associated with different types of trauma. Injury to the peripheral nerve (nerves outside of the brain and spinal cord) may result from blunt force, fractures, crush injuries, stretch, penetrating or cut injuries. The nerves of the upper limb are the most commonly injured. The healing process from nerve injury can take from a few weeks to a few months. Both recovery and repair depends on the type of injury and the extent of damage.
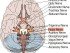
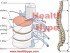
Nerve Structure
The peripheral nerve is made up of axons and Schwann cells. It can have an outer insulating layer (myelinated type) or lack this insulation (unmyelinated type). The Schwann cells form a sheath over each axon in myelinated nerves and in the unmyelinated nerves Schwann cell-sheath covers a group of axons. The Schwann cell-sheathed axons are covered in a layer of connective tissue called endoneurium.
Several endoneurial tubes form a nerve fascicle. Each fascicle (bundle) of the nerve fiber is covered by a layer of tissue known as the perineurium. Numerous fascicles of nerve are covered by a layer called as epineurium. The nourishment to the nerve is obtained from the blood supply to the nerve. The blood supply to each of the nerves is provided by the system of blood vessels called vasa nervorum that runs in each nerve.
Types of Nerve Injury
Nerve injuries can be broadly grouped into three types :
- neuropraxia
- axonotmesis
- neurotmesis
Neuropraxia
Neuropraxia is the least severe type of nerve injury. It results in complete block of nerve transmission despite intact nerve fibers. Neither the axon nor the sheath are cut. Sudden stretching of nerves in fractures and dislocations can lead to neuropraxia. It can also occur with blunt injuries and sometimes after prolonged pressure on the nerve. Neuropraxia usually recover spontaneously over a few hours to few months.
Axonotmesis
In traction injuries and crush injuries, the nerve sheath may remain intact but the axons may be divided. This is referred to as axonotmesis. Axonotmesis can result in complete loss of muscle (motor) function, sensations and autonomic functions transmitted by the affected nerve. The recovery usually takes several months to years.
Neurotmesis
Partial or complete severance (cut) of the axons and the sheath is referred to as neurotmesis. It is the most severe form of nerve injury. However, a clean cut has scope for immediate repair and faster recovery.
Healing of Nerve Damage
There may be recovery of nerve injury over weeks and months if there is no severance (cut). However, recovery of a severed nerve may never occur. The nerve repair process involves degeneration of the nerve followed by regeneration. The degeneration of nerve is called Wallerian degeneration. The process involves phagocytosis of the damaged segment of the nerve beyond the site of nerve injury. The regeneration of the nerve is guided by the presence of some important growth factors or neurotropic substances like the nerve growth factor (NGF). Many other growth factors and cytokines are also believed to affect the process of degeneration-regeneration.
Following degeneration of the nerve, the nerve begins regeneration. The regeneration starts at the proximal end of nerve at the site of injury. It progresses slowly to the distal part of degenerated nerve. Regeneration occurs at a very slow rate. It occurs at a rate of 1mm/day. The recovery takes longer time if the distance to be covered by regeneration is long. A nerve damaged closer to the muscle that it innervates recovers much earlier than a nerve which is damaged further away from the muscle.
The regenerated nerves may end up with abnormal connections. It can result in abnormal movements or sensations. An injured nerve that supplies muscles can resume its function only if the re-innervation happens within 18 months after the injury.
Mechanisms of Nerve Injury
Nerve injury can result in a variety of ways. Some of the major mechanisms behind nerve injury are discussed below.
Mechanical injury resulting from a tourniquet or other causes of external pressure can lead to nerve compression and therefore injury. The nerve may also be compressed by adjacent structures or from trauma in the body. A Compression nerve injury can result from crush injuries, pressure from fractures, hematoma, blunt injury and in compartment syndrome where swelling of tissues in a closed muscular compartment resulting in compression of the nerve or its blood supply.
Laceration injury can result from blunt or penetrating injury. The nerve injuries causes irregular patterns of nerve damage. Nerve severance (cut) can occur but the severance is often not clean division as seen in cut injuries.
Penetrating injuries can result partial or complete severance of the nerves. It can result from wounds from stabbing or cut wounds from sharp objects.
Stretch injuries are common in fractures and dislocations. The injury results from the sudden stretch of the nerves during dislocation. Almost half of all shoulder dislocations lead to nerve injury but it is significantly less with other joint dislocations. A stretch injury to the peripheral nerves can also occur during certain surgical procedures.
Direct nerve injury can result from high-velocity trauma sustained in motor accidents and in ballistic injuries. A displaced bone fracture can also cause direct nerve injury. Violent traction can result in injury to the nerve and even lead to severance.
Signs and Symptoms of Injured Nerve
Acute nerve injury is characterized by loss of its normal function. This depends on the type of nerve injured – motor or sensory. Motor nerve injury affect motor function (muscle movement) while sensory nerve injury results in impairment of the senses. The muscular function impairment may be in the form of weakness or paralysis. The sensory impairment can present as loss of sensations, abnormal sensations (parasthesias) or pain.
The symptoms of nerve injury also depend on the nerve injured and the site of nerve injury. In many patients the injury may not present with such specific or clear signs and symptoms. Some of the symptoms may develop much later after the injury while other symptoms may completely recover in few hours.