Pneumonia (Inflamed Lung) Types, Cough, Symptoms, Risks
What is Pneumonia?
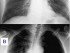
Pneumonia is any disease that causes inflammation of the lung tissue, particularly the air sacs (alveoli) of the lung. It is a fairly common respiratory disease that can be life threatening. Most cases of pneumonia are due to infectious causes, with bacterial pneumonia being the most common, followed by viral and fungal pneumonia. However, other non-infectious causes of pneumonia like mechanical or chemical injury can be equally devastating if left untreated.
Pneumonia is commonly seen after respiratory tract infections, especially in older patients or young children. People with chronic debilitating conditions and systemic infections like HIV are at risk of acquiring pneumonia, often with life threatening consequences. In pneumonia, a lobe, segment or the entire lung may be affected. It results in significant damage to the epithelial lining of the air sacs (alveoli) known as diffuse alveolar damage (DAD).

This affects gas exchange and eventually lead to death unless the appropriate treatment is commenced. Sometimes only a small part of the lung tissue is affected but there is significant inflammation and damage of the distal parts of the respiratory tract. This is known as bronchopneumonia and is often a complication acute bronchitis, tracheitis or seasonal influenza (flu).
Types of Pneumonia
There are different types of pneumonia that are classified according to :
- mechanism of injury
- area and extent of the inflammation (anatomical distribution)
- setting in which the condition was acquired
- microorganism involved in the infection
Broadly, pneumonia can be categorized as :
- Infectious pneumonia – this can be further categorized according to the causative microorganisms which is discussed below.
- Non-infectious pneumonia – this is caused by a number of mechanisms that trigger inflammation.
- Chemical pneumonia
- Inhalation of toxic gases or fumes
- Aspiration of stomach acid, toxic chemicals (usually liquid) or solid particles like organic/inorganic dust
- Aspiration pneumonia is chemical or infectious pneumonia that is a result of the following entering the lung :
- Foreign objects
- Gastric (stomach) contents
- Aspirated fluids
- Neurogenic pneumonia occurs with injury to the brain, spinal cord and surrounding nerves.
- Chemical pneumonia
Anatomical Distribution
- Lobar Pneumonia
- One of more lobes of the lung may be affected, with the infection being very localized to these areas.
- Most cases are infectious and frequently arises as a secondary bacterial infection following a viral respiratory infection like influenza.
- Bronchopneumonia
- Affects the terminal parts of the airways (bronchi and bronchioles) with the inflammation involving small areas of lung tissue around these parts of the respiratory tract.
- Often due to infectious causes complicating from acute bronchitis, tracheitis or influenza.
- Interstitial Pneumonia
- Affects the connective tissue and lining of the alveolar septa (walls between the air sacs) often resulting in widespread inflammation at multiple locations in the lung.
- May be triggered by known infectious and non-infectious factors although the cause is often related to immune-mediated disorders. Frequently, no known cause can be identified (idiopathic).
Setting of Infection
The causes of pneumonia are usually due to an infection acquired within a clinical or institutional setting and often spread among patients or residents. Multi-drug resistant (MDR) bacteria are often implicated.
- Community-acquired pneumonia (CAP) arises :
- After an outpatient visit
- Within 48 hours of hospital admission
- Health Care-Associated Pneumonia (HCAP) includes :
- Hospital-Acquired Pneumonia (HAP)
- Develops after 48 hours or more of being admitted to hospital.
- Ventilator-Associated Pneumonia (VAP)
- Develops after 48 hours or more of being on a ventilator / endotracheal intubation or within 48 hours after being off a ventilator /extubation.
- Institution-Acquired Pneumonia
- Develops in patients within institutions, like mental health institutions, or residents of a nursing home (NHAP).
- Hospital-Acquired Pneumonia (HAP)
Pathogenic Microorgansims
Most cases of infectious pneumonia are bacterial in origin. Viral or fungal pneumonia may also occur with the latter often being associated with immunocompromised patients, particularly as opportunistic infections in HIV/AIDS patients.
- Bacterial Pneumonia – common bacteria :
- Streptococcus pneumoniae (pneumoccocal pneumonia)
- Staphylococcus aureus
- Enterococcus (Enterococcus faecalis, Enterococcus faecium)
- Pseudomonas aeruginosa
- Klebsiella pneumoniae **
- Haemophilus influenzae
- Escherichia coli **
- Mycobacterium tuberculosis
- Streptococcus pneumoniae (pneumoccocal pneumonia)
** New strains may be NDM-1 superbug.
- Viral Pneumonia – causative viruses :
- Influenza including H5N1 (bird flu) and severe acute respiratory syndrome (SARS)
- Parainfluenza
- Adenovirus
- Rhinovirus
- Herpes simplex virus
- Respiratory syncytial virus (RSV)
- Cytomegalovirus (CMV)
- Fungal Pneumonia – causative fungi :
- Candida spp
- Aspergillus spp
- Mucor spp
- Cryptococcus spp
- Coccidioides spp
- Blastomyces spp
- Atypical pneumonia (walking pneumonia) includes less common microorganisms (mainly bacteria) that may cause pneumonia, which is usually mild.
- Mycoplasma pneumoniae
- Chlamydophila pneumoniae
- Legionella pneumophila
- Bordetella pertussis
Pneumonia Risk Factors
Pneumonia is the inflammation of the lung tissue most often due to an infection. A number of microorganisms may cause pneumonia although bacteria are the most common pathogen.
Pneumonia can affect any person of any age and health status. However, in patients who are chronically ill, debilitated, young children or elderly patients, the possibility of a contracting is significantly high if exposed to the causative pathogen.
Known Risk Factors for Pneumonia
- Age
- Elderly > 65 years
- Infants < 2 years
- Lifestyle
- Cigarette smoking
- Alcohol use (excess)
- Medication
- Corticosteroid therapy
- Diseases
- Respiratory tract infections, particularly lower tract but also upper
- HIV
- Pre-existing lung disease
- Environment
- Air pollution (indoor, work exposure)
- Health Care Facilities and Institutions
- Outpatient visits (clinics)
- Hospitals
- Nursing homes
- Other health care institutions
Many of the risk factors relate to impaired or low immune functioning, as seen with age, chronic illnesses and particularly conditions like HIV infection.
Any dysfunction of the cough reflex also increases the risk for contracting pneumonia as mucus containing pathogens cannot be cleared from the respiratory tract effectively. An impaired cough reflex is often seen in cigarette smokers, heavy alcohol consumption, use of sedatives (especially in sedated patients within a hospital/institution setting), and stroke patients.

How does pneumonia occur?
Pathophysiology
Most cases of pneumonia are due to infectious causes i.e. pathogenic microorganisms, particularly bacteria. The pathogen usually reaches the lung tissue through the respiratory tract when it is inhaled. However, some cases of pneumonia are due to pathogens that reach the lung via the bloodstream or an infection of a neighboring site.
The pathogen causes injury of the alveolar epithelial cells and capillaries of the alveolar septa. The microvascular injury increases vessel permeability thereby allowing proteins, blood cells and fluid from the blood to empty into the interstitial spaces causing alveolar edema (swelling). This then leaks into the alveoli.
As the infection spreads to neighboring alveoli, the same process occurs resulting in the entire lung or a part of it becoming congested with cells, fluid and cellular debris (microorganism, blood cells and lung parenchymal cells). Once large areas of the lung is congested in this manner, it is said to be consolidated.
During the course of pneumonia, the lung’s gas exchange function is impaired. The edema and exudate reduces the surface area of he lung and hampers gas exchange between the air and blood in the lung, although there is normal blood flow to the lung. This causes a drop in oxygen within the blood (hypoxemia) with a simultaneous elevation in blood carbon dioxide (hypercapnia). Although the healthy lung will still be functioning as normal, the combined oxygen saturation is still below normal.
If left untreated or if the body is unable to cope with the disease process, the condition will spread to affect an entire lung or even both lungs. Inability to respond to treatment may lead to death. However, with proper treatment and in healthy patients, the consolidated exudate is essentially ‘cleaned’ out of the lung. This may occur by digestion and resorption, consumption by macrophages, coughing up the exudate or it undergoes fibrosis.
Pneumonia Cough and Sputum
The typical symptom associated with infectious pneumonia, similar to other lower respiratory tract infections like bronchitis, is a productive and persistent cough. It is usually described as a deep cough that is nagging with sputum being expectorated into the throat or mouth. However, in the early stages, a pneumonia cough may not present in this manner. Initially it is dry and non-productive with pain in the center of the chest. This is similar to the cough in tracheitis.

Coughing up blood or bloody sputum becomes evident as the condition progresses although this may not be present in every case of pneumonia. Typically the cough lasts for less than 3 weeks (acute) although a chronic dry cough associated with lung inflammation (evident on x-ray) is seen in interstitial pneumonia.
The color and nature of expectorated mucus may provide some indication of the type of infection :
- Yellow mucus is seen in the early stages of a productive penumonia cough
- Green mucus is seen in more chronic infectious pneumonia
- Rusty red-colored mucus is seen in pneumococcal pneumonia (Streptococcus pneumoniae)
- Deeper red-colored mucus may be seen in Klebsiella pneumoniae infection
- Bad tasting and foul smelling mucus is seen in infectious pneumonia caused by anaerobic bacteria like S.pneumoniae, S.aureus and K.pneumoniae
Signs and Symptoms
Apart from the cough mentioned above, the other symptoms of pneumonia may vary greatly depending on the cause and type of pneumonia.
- Chest pain
- Centrally located early in the disease and progresses to the affected side, although the unaffected side may experience some discomfort as well.
- May be associated with pleuritis that is often associated with lung diseases like pneumonia.
- Pain pronounced on coughing or breathing in deeply. Refer to lung chest pain for other causes of chest pain associated with respiratory diseases.
- Pain may be referred to shoulder or upper abdomen.
- Upper abdominal tenderness may be a sign of lower lobe pneumonia.
- Shortness of breath (dyspnea)
- Difficulty breathing (‘not getting enough air’) is reported in most cases to varying degrees.
- In milder cases, shortness of breath may only be reported after activity, which is uncharacteristic for the patient’s usual exercise tolerance.
- Rapid, shallow breathing may be present in severe cases (ARDS = acute respiratory distress syndrome) and may be accompanied by pallor (infrequent) or cyanosis (very rare).
- Abnormal breathing sounds
- Bronchial breathing, whispering pectoriloquy and crackles my be present in pneumonia.
The other signs and and symptoms of pneumonia are non-specific and may be seen in many infectious diseases, particularly respiratory tract infections.
- Fever and chills
- Sweating
- Fatigue
- Nausea and/or vomiting
- Loss of appetite
- Headache
- Diarrhea (sometimes)
Pregnancy Pneumonia
The hormonal changes that occur during pregnancy may hamper immune functioning and aggravate pre-existing nasorespiratory allergic conditions that are marked with mucus hypersecretion, like hay fever. Contracting a viral infection such as a cold or influenza (including H1N1 swine flu) during pregnancy can lead to complications such as pneumonia.
Bacterial pneumonia can occur secondary to a viral respiratory tract infection or it can occur without any prior viral infection. Any person with mucus hypersecretion is at an increased risk of contracting bacterial respiratory infections and this is more pronounced in pregnant women.
There is also evidence to suggest that adverse outcomes like a spontaneous abortion (miscarriage) following viral respiratory tract infections are more likely to occur in cases that complicate into pneumonia. Early antiviral treatment in pregnant women is often considered these days especially after the 2009 H1N1 swine flu pandemic. In this outbreak, fatalities among pregnant women who contracted H1N1 was often linked to pneumonia, among other complications.
Read more on Influenza, Swine Flu and Common Cold during Pregnancy.
Hospital Pneumonia
Health care-acquired pneumonia (HCAP) and hospital-acquired pneumonia (HAP) has received much attention in recent years. Previously, ventilator-associated pneumonia (VAP) was the main concern for contracting pneumonia in the hospital setting.
However, with widespread multi-drug resistant (MDR) strains of bacteria, which are more frequently seen in health care facilities, HCAP and HAP have also become a concern even for patients who visit facilities on an outpatient basis. The risk significantly increases with hospitalization, especially after 48 hours. MRSA (methicillin-resistant Staphylococcus aureus) and the more recent NDM-1 strains of Klebsiella pneumoniae and Escherichia coli (E.coli) are of particular concern, especially since the latter is very resistant to new age antibiotics and antibiotic cocktails.
Nursing Home Pneumonia
Pneumonia contracted by patients or residents within homes for the elderly, frail care institutions and health institutions is broadly referred to as institution-acquired pneumonia. Nursing home-acquired pneumonia (NHAP) is often seen because the residents are living in close quarters (a risk for outbreaks) but are also older than 65 years of age (a high risk group). Patients who are heavily sedated, as seen in those who are terminally ill (hospices), addictions (rehab centers) and mentally ill are also at risk due to living in close quarters in addition to being debilitated (weak immune system) and having a suppressed cough reflex.
References
- Bacterial Pneumonia. Medscape
Last updated on August 19, 2018.