What is Crohn’s Disease – Pain, Diet, Surgery, Living With CD
What is Crohn’s Disease?
Crohn’s disease is a type of inflammatory bowel disease (IBD) and may affect any part of the gut, especially the colon and the last part of the small intestine. It usually occurs with nausea, low-grade fever, abdominal pain and diarrhea. Crohn’s disease may be mild and may disappear completely after some time or it may be ongoing where it requires long term medical and even surgical treatment.
Crohn’s disease is a chronic condition marked with periods of aggravation and remission. There may also be complications, which involves the joints, skin, eyes or other body parts. Krone disease, Chron disease, Crone disease and so on are some common misspellings for Crohn’s disease, named by Burrill Bernard Crohn, one of the first gastroenterologists who described it in 1932. The other type of inflammatory bowel disease is ulcerative colitis, which affects only the colon.
Symptoms of Crohn’s Disease
Symptoms may differ to some degree from person to person and it also depends on the area of the gastrointestinal tract that is affected (1). Some of these signs and symptoms include:
- Nausea, poor appetite, loosing weight
- Pain or cramps, commonly in the lower right or lower left abdomen
- Low-grade temperature
- Diarrhea
- Mucus or blood in the stool
- Skin rashes
- Mouth ulcers
- Arthritis
- Eye inflammation
Complications
Complications of Crohn’s disease are common and may include (1):
- Abscesses (collections of pus) under the skin around the anus or in the bowel wall
- Bowel ulcers
- Bowel fistula – a tunnel, which usually starts in a bowel ulcer or abscess and may connect two adjacent parts of the bowel, or bowel and bladder, vagina or skin around the anus. Bowel content can drain through the fistula into other organs or to the skin surface.
- Anal fissure – a painful crack in anal mucosa
- Bowel obstruction due to inflammation or scars in the bowel mucosa
- Colorectal cancer may sometimes develop after prolonged severe disease
- Malnutrition
- Delayed growth and sexual development in children
- Kidney stones
- Gallstones or inflammation of the bile ducts
- Hepatitis
- Osteoporosis
Anal Fistula
Anal fistula is a narrow channel with internal opening in the anal canal and one or more external openings in the skin close to the anus (Picture 1). Fistula may be painful, especially during the bowel movement, and may discharge pus or stool. Anal fistula will not heal on its own. Treatment is surgical: by cutting the fistula, advanced tissue flap, fibrin glue or by using other techniques(3). It may take some weeks for fistula to heal completely.
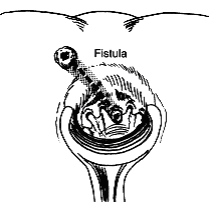
Picture 1. Anal fistula, starting in rectal mucosa,
and ending in the skin around the anus
What Causes Crohn’s Disease?
Currently, Crohn’s disease is considered as an autoimmune disease but the exact cause remains unclear. Other possible causes include: infection with Mycobacterium avium subspecies paratuberculosis (MAP), psychological stress and heredity. Some of affected people have a close relative who has/had a disease and some have mutations in a gene called NOD2/CARD15.
Changes in Bowel Mucosa in Crohn’s Disease
Crohn’s disease mostly affects the lining (mucosa) of the end part of the small intestine (terminal ileum) where the small intestine becomes continuous with the large intestine (1). Any part of the digestive tract from the mouth to the anus may be affected, though. Therefore signs and symptoms of Crohn’s disease may vary depending on the location of the inflammation. There may also be ulcer formation although not as pronounced as in ulcerative colitis (UC).
Who Can Get It?
Risk factors for Crohn’s disease include:
- Young age. Crohn’s disease may appear at any age but most commonly in young adults. Children before puberty are rarely affected.
- Smoking
- Living in urban areas
- Isotretinoin (Accutane) – a medication for scarring cystic acne
- A close relative with Crohn’s disease
- Whites of European descent and Jewish are at increased risk.
Diagnosis of Crohn’s Disease
Diagnosis of Crohn’s disease bases on symptoms and summary of results of investigations; there is no single test to confirm Crohn’s disease (1). Blood work may reveal anemia ( because of iron, folate, vit B12 deficiency), elevated white blood cells and certain antibodies (not in all cases). Lower and upper GI (x-ray with barium) mayshow inflammatory changes in the bowel; typical findings are cobblestone appearance of the colon and several bowel narrowings (strictures). Diagnosis is strongly supported by finding inflamed mucosa during colonoscopy, and microscopic investigation of a sample of colonic mucosa obtained by biopsy. To check for inflammation in the small intestine, an upper endoscopy or capsule endoscopy may be done.
Treatment of Crohn’s Disease
Anti-Inflammatory Medications
Crohn’s Disease may be treated with anti-inflammatory drugs like sulfasalazine, mesalamine or corticosteroids. For patients who don’t respond on regular treatment, adalimumab (Humira), a synthetic immunoglobulin, is available – it shortens the course of the disease but it has many side effects: severe, even deadly infections, hepatitis B reactivation, some types of cancer, fever, easy bruising, etc. (2).
Supplements and Other Medications
Iron or certain vitamins may be needed if blood tests reveal their deficiency. Anti-diarrheals or pain killers may also be needed.
Details about treatment of Crohn’s disease.
Diet in Crohn’s Disease
Dietary changes were not proven to treat Crohn’s disease. But symptoms may be lessened by:
- Small meals and avoiding problematic foods (by experience) to prevent diarrhea
- Avoiding dairy products to lessen diarrhea due to impaired lactose (milk sugar) digestion
- Avoiding high-fat foods since fat digestion may be impaired
- Drinking enough to replace fluid lost with diarrhea
- Eating foods with appropriate fiber content according to symptoms (constipation or diarrhea)
Surgery
Complications, like fistulas, bowel obstruction, severe inflammation or abscesses, commonly require surgery, and often a part of the bowel has to be removed. For some patients this may mean years of symptoms cessation but inflammation often reoccur and subsequent surgeries may be needed.
Living With Crohn’s Disease
Severe Crohn’s disease may be discouraging. Affected persons should learn how much they can fight the disease and what they need to accept as a fact. Support groups for Crohn’s disease and ulcerative colitis exist in many countries; online support is also available.
References:
- Crohn’s disease (ccfa.org)
- Anal fistula – surgery options (cookmedical.com)





