First Aid in Sudden Cardiac Death (SCD)
What Is Sudden Cardiac Death (SCD)?
Sudden cardiac death is an unexpected death due to cardiac causes occurring within 1 hour of symptom onset in a person in whom no previously life threatening heart condition was diagnosed. Typical SCD victim is an adult, collapsing without obvious reason during regular activity and dying in few minutes from a heart failure. Over 300,000 persons dye in US each year from SCD. More than half of all heart deaths are due to SCD. SCD has a peak at 45-75 years of age, children are rarely affected (1).
Most cases of SCD are related to ventricular fibrillation or other types of arrhythmia.
Ventricular Fibrillation (VF)
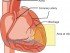
In a healthy heart, stimulus for a contraction originates from the wall of the right upper heart chamber (atrium) and propagates through the conducting system toward the apex of the heart. This electric flow triggers repeated and organized contractions of the heart muscle, normally at 60-100/min at rest. In ventricular fibrillation (VF), heart excitation starts in lower heart chambers (ventricles) and causes non-organized heart contraction at rate beyond 300/min (2). Ventricles thus do not have time to fill completely before the next contraction, so they can not push enough blood to the arterial system. Blood pressure falls, the brain does not get enough oxygen, and unconsciousness follows. Ventricular fibrillation rarely stops spontaneously so a defibrillation by use of a defibrillator is usually required.
Underlying Diseases in SCD
In 80% of SCDs, coronary atherosclerosis can be found, and heart ischemia (angina pectoris) or heart attack may develop from it. The risk for SCD can persist for up to 24 month after the heart attack (1).
Other causes of SCD: dilating or thickening of the heart wall in cardiomyopathy, ventricular tachycardia, congenital heart disease, aortic stenosis, low blood serum potassium, heart surgery, digoxin, tricyclic antidepressants, cocaine, antiarrhythmic drugs, and so on. The strongest predictor of SCD is left ventricular dysfunction from any cause (1).
Symptoms of SCD
Affected person may experience chest pain or breathlessness from 20 minutes to many hours before SCD (3). Dizziness, fainting or vomiting are less commonly observed. The victim collapses, falls on the ground and may grasp for the air. There is no palpable pulse of carotid artery on the neck, and breathing may cease. Consciousness may be lost in few minutes.
How Can We Say Is It SCD?
Absent or irregular pulse in suddenly collapsed person without known heart disorder speaks for SCD.
Other causes of sudden unconsciousness, but with present breathing and pulse, include: fainting from heat or fear, epileptic seizures, hypoglycemia (common in diabetics), alcohol, drug or other poisoning, head injury, heart attack, brain stroke, renal or liver failure, heat shock, allergic anaphylactic shock after taking medications or food.
How to Help a SCD Victim?
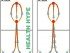
When someone collapses, doctor has to be called at once! If the patient shows no noticeable chest moving, artificial breathing mouth to mouth must be given immediately. If there is no palpable pulse on the carotid artery or pulse is totally irregular, another person must start with heart massage by pressing repeatedly on the chest wall. One breathing/massage cycle consists from two breaths and then 30-50 chest pressings in 30 seconds (4). This should be continued until breathing and normal pulse are restored, for up to one hour, if necessary, or until a doctor arrives and starts with defibrillation.
Defibrillation
Defibrillation (electrical cardioversion) is restitution of normal heart rhythm from ventricular fibrillation by use of a defibrillator, which delivers electrical shock to the heart. Direct current is used, typically 750 volts for implantable defibrillators and several thousand volts for external ones (5). Starting energy used is usually 200J and can be raised up to 360J.
Types of Defibrillators (6):
Manual external defibrillator is portable device with inbuilt ECG reader. It is mainly used by clinicians in hospitals. Clinician will check ECG and decide which voltage to use.
Manual internal defibrillators are used on an open heart in operating sales.
Semi-automated external defibrillators are combination of AED and manual defibrillators. They are mostly used by emergency medical technicians.
Automated external defibrillators (AED)are available in US, Japan, and other countries in certain crowded public places, like airports or stadiums, where cardiac arrests are likely to occur. AEDs are pre-programmed to recognize VF; even amateurs can use them successfully.
Defibrillation success decreases 5-10% for each minute after onset of VF, so quick start is needed. 10-20 seconds are necessary for AED to recognize a type of arrhythmia. Recommended energy for the first and subsequent shocks is 200J or 2J/kg for children. A patient must be dry and not in contact with any metallic object. AED’s pads are placed directly on the skin, one below the right clavicle and the other over the apex of the heart.
Resuscitated patients must be admitted to an intensive care, because of high risk of a recurrence; they need to be monitored for possible complications. Evaluation of ischemic injury to the brain, heart and other organs is essential. Patients typically have an underlying (heart) disease that requires treatment.
After successful defibrillation, the heart may need some minutes to hours to recover to its original output capability. Intubation, oxygen and intravenous drugs to support heart function, and electrolytic balance may be needed.
Implantable Cardioverter – Defibrillator (ICD)
People with high risk for SCD – those who survived SCD or have unstable arrhythmia – can get implantable cardioverter – defibrillator (ICD) (7). This is an electronic device of a matchbox size, surgically implanted beneath the skin under the clavicle. Its electrodes are pushed through veins into the heart and attached to the apex of the right ventricle. While constantly monitoring the heart rate, ICD can return irregular heart beat back to normal with bursting electric impulses. ICD has a great value in appropriate patients, but in 1/3 of patients no benefit is gained. After experiencing ventricular fibrillation and shock delivered by ICD, patient has to visit a clinic to evaluate what exactly has happened.
Is Defibrillation Safe?
According to Gaston Emergency Medical Services (GEMS), automatic external defibrillator (AED) detects fibrillation in 90%, and in 99% recognizes rhythm that should not be defibrillated. It means that defibrillator will not deliver electric shock to a person with normal heart rhythm, or rhythm other than fibrillation. So, it is not likely that a misuse of a defibrillator on or by a healthy person would cause this person’s death, but can cause burns or one-time or recurrent arrhythmia. Medical personel should never test defibrillators at themselves!
Burns are common complications, especially on repeated defibrillation (8). They are mostly mild, but may be uncomfortable for the patient.
Another complication is post-defibrillation arrhythmia.
Defibrillation may damage implantable electronic devices like pacemakers.
How to Prevent SCD?
Every time when a heart patient feels chest pain or breathlessness, he should stop with all activities and sit down. Lying down is not recommended, since increased venous input would put additional burden to the heart. If symptoms persist, a sublingual nitroglycerin should be taken and repeated if pain does not vanish in 5 minutes. If no relief after three tablets of nitroglycerin, an onset of a heart attack as a possible cause must be considered and doctor called.
Complications of SCD
Possible complications due to diminished oxygen delivery during ventricular fibrillation are brain stroke or heart muscle injury. A victim, while unconscious, may inhale his own vomit and develop aspiration pneumonia. Complications of vigorous first aid procedure are spinal injury or broken rib(s).
Prognosis of SCD
Up to 90% of patients survive SCD, if first aid and defibrillation were performed in the first minute – usually in a hospital (9). General surviving rate is poor, though: 3-50% depends on time elapsed between ventricular fibrillation onset and defibrillation (1). Only few patients that did not get help within 8 minutes survived.
SCD and Sport
A study in Italy, performed between 1970-1990, has shown that young athletes between 12-35 age were twice as prone to SCD as opposed to their non-sport fellows. Sport itself does not represent a risk for SCD, but it acts as a trigger at those who have some underlying heart disease or abnormality.
Below age 35, the problem is usually an undiscovered congenital heart abnormality in the heart muscle, valves or coronary arteries, which may not cause any symptoms, allow full athletic development, but then suddenly causes death during exercise. From this reason, every athlete should have a thorough physical exam prior to engaging in training.
Hypertrophic Cardiomyopathy (HCM)
Although rare (0.1% to 0.2% prevalence), HCM is the most common cause of SCD in young athletes, like 33 years old sportsman Hank Gathers, who died in 1990 in the middle of a basketball game (10,11).
For athletes over age 35, the usual cause of SCD is a coronary artery disease.
In the younger population, most cases of SCD occur while playing team sports; in about 1/100,000 – 300,000 athletes. In older athletes, SCD occurs more often during running: in approximately 1/15,000 joggers and 1/50,000 marathon runners (12).
Hard physical exertion increases the risk of a sudden death from cardiac causes, especially in people who do not exercise regularly (13). Men over 40 and women over 50 years should have an exercise stress test made to see if they can engage sport activity safely (14).
Related Articles:
- Heart Disease – Types and Symptoms
References:
- Ventricular fibrilation: causes, epidemiology, treatment (emedicine.com)
- Images: Normal heart beat and ventricular fibrilation (wo-pub2.med.cornell.edu)
- Symptoms preceding VF (healthday.com)
- Cardiopulmonary resuscitation (CPR): First aid (mayoclinic.com)
- High voltage charge storage array for an implantable defibrillator (patentstorm.us)
- Types of defibrillators (edinformatics.com)
- Burns after defibrillation (ncbi.nlm.nih.gov)
- Survival rate of SCD (medicinenet.com)
- Basketball player Hank Gathers dies from SCD on the playground (en.wikipedia.org)
- Hypertrophic cardiomyopathy and SCD in young athletes (pubmedcentral.nih.gov)
- Incidence of SCD in sport (clevelandclinic.org)
- Risk of vigorous exercise for SCD (webmd.com)
- Exercise stress test (americanheart.org)
This article is the property of http://www.HealthHype.com
Copying and publishing any article from our site is strictly NOT allowed.