5 Fungi That Grow On Your Skin, Hair And Nails
Fungal infections of the outer surface of the body is not uncommon in the world. It has been estimated that 70% of the world’s population will suffer with a fungal infection of the skin at some point in life. The vast majority of cases are not serious. It may be persistent or recurrent but a fungal infection of the skin rarely leads to any serious complications. However, these fungal infections can still be quite distressing for a person – apart from the symptoms like itching which may be a bother, it can also cause unsightly skin rashes that can prove to be embarrassing.
Why do we get fungal infections?
Fungi live on and even in our body, domestic animals and the soil among other places. Some people may never develop a fungal infection of the skin and despite fungi being prevalent in the environment a skin infection is unlikely to occur unless the ideal conditions exist. A break in the skin, dampness or dryness of the skin, close contact with a person who is infected and the use of public amenities are some of the main risk factors for developing a fungal infection of the skin.
These conditions are not always avoidable and not every person exposed to it will develop a fungal infection. However, the fungi that tend to infect and grow on human skin, hair and nails have adapted to thriving on a specific organism. In other words, many fungi that infect the human skin, hair and nails have a predilection for humans. There is some evidence to suggest that certain people have a genetic predisposition to developing fungal infections.
Types Of Fungi
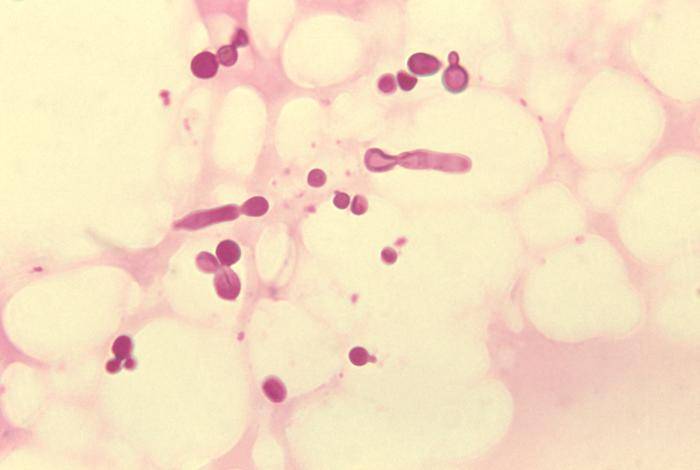
There are two main types fungi that can infect humans – dermatophytes and yeasts.
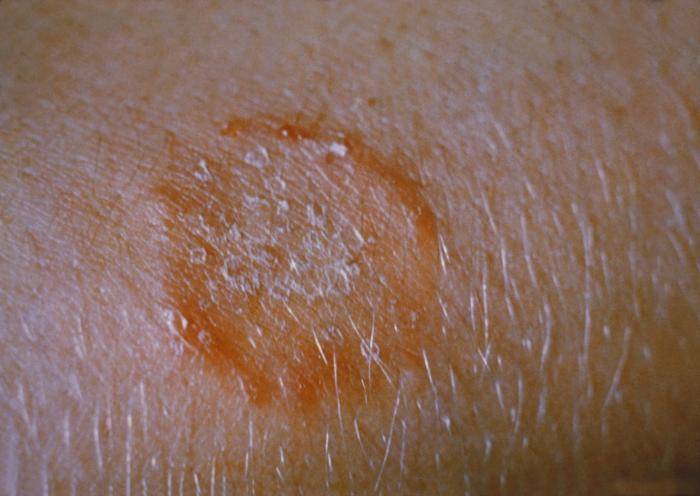
While yeasts like Candida albicans can cause skin infections particularly at areas of chaffing, it can also infect the body cavities like the vagina (vaginal candidiasis/thrush) and the mouth (oral candidiasis/thrush). Dermatophytes are by far the most common type of fungi that infects the skin, hair and nails. There are hundreds of species, all of which have specialized protein-digesting enzymes that consume the keratin in the outer skin layers. Dermatophytes often cause a circular skin rash which is the reason why it is commonly referred to as ringworm.
The two main species of dermatophytes that are responsible for most fungal skin infections are the Trichophyton and Microsporum species. These fungi can forms spores which may reside in the environment for years before infecting a person. Dermatophytes can be easily treated but are also ‘stubborn’ infections which tend to recur. In comparison, yeasts like Candida prefer the surface of living tissue and tend to thrive in the mucous membranes lining the body cavities.
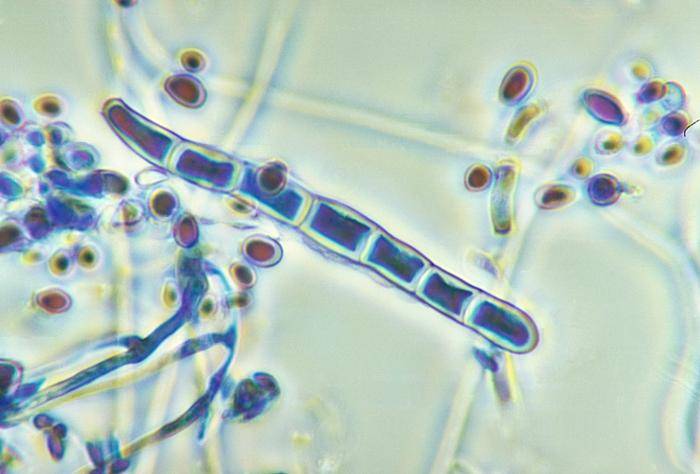
Trichophyton Species
The Trichophyton genus is the most common dermatophytes responsible for fungal skin infections in humans. Of these, Trichophyton rubrum is the main species that causes common fungal infections of the skin like athlete’s foot and jock itch. Other common Trichophyton species include T. interdigitale, T. tonsurans and T. verrucosum. T. tonsurans is very common in the United States and in some fungal skin infections in certain regions of the US, it is the primary cause.
Most of these fungi are anthropophilic meaning that it specifically infects humans and is easily transmitted from one person to another. It causes a mild but chronic inflammation of the skin. There are other Trichophyton species that may also be responsible but are far less common. T. verrucosum is a zoophilic fungus that originates in cattle but can infect humans who come into close contact with the animal on a regular basis. Some Trichophyton species are geophilic, meaning that it originates from the soil but can infect humans and animals.
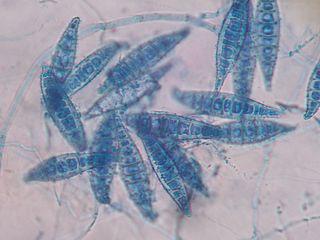
Microsporum Species
The Microsporum genus of fungi are the other common dermatophytes that responsible for fungal infections of human skin, nails and hair. Common Microsporum species include M. audouinii, M. ferrugineum, M. canis, M. nanum, M. distortum and M. gypseum. Some of these species are anthropophilic (human), zoophilic (animal) or geophilic (soil) fungi.
However, the important point to note about these fungi are the zoophilic species which have become increasingly common sources of infections. Microsporum canis originates from dogs and cats but can infect humans who are in close contact with humans. It causes a marked inflammatory reaction in humans but often it is a short lived infection that ends quickly. M. nanum originates in pigs and M. distortum is a variant of M. canis that originates in cats.
Epidermophyton Species
The Epidermophyton genus contains two species and only one, E. floccosum, infects humans. It is an anthropophilic organisms meaning that it has a predilection for humans. E. floccosum is present throughout the world and is an important cause of athlete’s foot (tinea pedis), jock itch (tinea cruris), body ringworm (tinea corporis) and fungal nail infections (onychomycosis). It does not appear to invade human scalp hair (tinea capitis). However, in people with a weakened immune system (immunocompromised), these fungi can invade deeper tissue as with most dermatophytes.
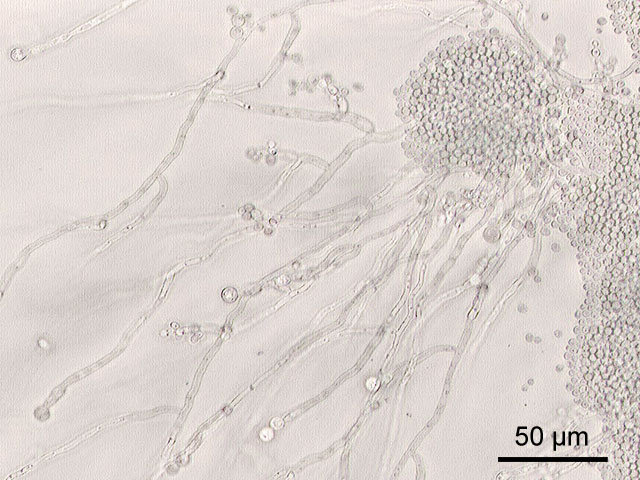
Candida Species
The genus Candida are yeasts and the most commonly known species is Candida albicans. Other lesser known species includes C. tropicalis, C. parapsilosis, C. glabrata and C. guilliermondii. It is naturally found on humans, primarily in the digestive tract, but does not usually cause an infection unless a person is immunocompromised. Sometimes an overgrowth can occur when the natural environment where it exists is altered in a way that allows it to thrive unchecked.
Candidiasis of the skin is not common when compared to fungal skin infections caused by dermatophytes (dermatophytosis). When candidal skin infections do occur, it is mainly at sites where the deeper living tissue is exposed. This may be seen at the body folds where the skin is inflamed and even eroded in severe cases. Apart from a weakened immune system as in AIDS, these candidal skin infections also commonly arises in diabetics and people who are obese. It may also be responsible for some cases of diaper rash.
Malassezia (Pityrosporum)
The Malassezia genus of fungi are naturally found on human skin, along with other yeasts and various bacteria. But in the vast majority of cases it does not cause any problems. It is the combination of other microbes on the skin (skin microflora) that keeps the Malassezia yeast in check. However, these fungi can cause skin and scalp problems like tinea versiclor, seborrheic dermatitis and dandruff. Previously the Malassezia genus was known as Pityrosporum and the term pityriasis is still used to refer to infections by these fungi.
Although Malassezia fungi can become pathogenic and infect the skin, it usually causes a very superficial infection in that it is largely restricted to the outermost layers of the epidermis. However, these fungi may also serve to cause skin and scalp problems in other ways. It is believed that an overgrowth of Malassezia fungi and an abnormal immune response to its presence on the skin may be the mechanism behind seborrheic dermatitis and dandruff. It is among one of the most common fungal skin conditions seen in people living with AIDS.
References:
dermnetnz.org/fungal/mycology.html
www.mycology.adelaide.edu.au/Fungal_Descriptions/Dermatophytes/Epidermophyton/
www.nlm.nih.gov/medlineplus/ency/article/000880.htm