Anthrax (Bacillus anthracis) Human Infection
What is Anthrax?
Anthrax is a serious zoonotic infection meaning that it is transmitted from animals to humans. This infection is caused by a spore-forming bacterium known as Bacillus anthracis. Although anthrax mainly affects domestic and wild animals, the bacteria can infect humans if they come in contact with sick animals.
It has been a cause for serious concern in recent years due to the possibility of anthrax being used as a biological weapon. B. anthracis enters the body through wounds in the skin, by eating contaminated meat or by inhaling the spores. In most of the cases, it is not transmitted from person-to-person and the skin lesions are rarely contagious.
Types of Anthrax
The three main types of anthrax are:
- Cutaneous (most common)
- Inhalational
- Gastrointestinal
– Oropharyngeal anthrax is a sub-type of intestinal anthrax, affecting the oropharynx (middle part of the throat, at the back of the mouth). Oropharyngeal anthrax develops after eating contaminated meat products.
Symptoms of the three types vary and could include skin sores, nausea, vomiting, or shock. Cutaneous and gastrointestinal forms of anthrax are mild and can be treated easily with antibiotics. Inhaled anthrax can be difficult to treat and is usually fatal.
How Common is Anthrax?
Anthrax affects people of all ages, genders, and races. Natural incidence of anthrax among humans is rare. B. anthracis infection is mostly an occupational hazard among farmers, veterinarians, agricultural or industrial workers, shepherds and people who handle animal wool, hides, hair, meat, or bones. Less than 1 case was reported annually in US during the last 30 years. From 1955 to 1994, there were 11 cases of inhalational anthrax and 224 cases of cutaneous anthrax, with 20 fatalities.
What Happens in Anthrax?
Anthrax mostly affects herbivore animals like cattle, goats, sheep, and horses. Animals like pigs, dogs and cats are more resistant. Birds are naturally resistant to anthrax but may carry the spores on their bodies.
Human infection
Anthrax bacteria have a capsule filled with toxins. These bacteria are very robust and can multiply quickly. The toxins of anthrax bacteria are called edema toxin and lethal toxin. Another molecule called protective antigen works like an anchor for the bacterium and helps it bind to target cells. The bacterium then releases the toxins into the cells. Edema toxin causes massive swelling. Lethal toxin affects cells of the immune system. It results in release of certain chemicals, which are responsible for the sudden death of patients or infected animals.
- Cutaneous anthrax
– Cutaneous anthrax spreads through breaks in the skin.
– A boil develops at the infection site and forms a crust.
– The site of infection becomes swollen.
– The bacteria multiply and enter the bloodstream or other organs (like the spleen).
- Gastrointestinal anthrax
– Intestinal anthrax produces lesions in the large intestine.
– Spores enter the mucus membranes of the gastrointestinal tract and cause ulcers that bleed.
– Stomach and intestine swell soon after bacteria enter the bloodstream.
– Anthrax affects the throat tissues after eating contaminated meat products.
– Ulcers are common, along with throat pain and difficulty in swallowing.
- Inhalational anthrax
– Inhalational anthrax occurs after inhaling spores into the lungs.
– The toxins cause bleeding, swelling and inflammation of the lungs.
– If untreated, inhalational anthrax results in death in most cases.
Signs and Symptoms
Symptoms usually appear within a week of exposure to the bacteria.
Cutaneous anthrax
Symptoms of this mildest and most common form of anthrax may include the following:
- Small painless bump or sore on the skin
- Itching
- Small black crust forming in the centre of the sore
- Swelling in the sore
- Swelling of nearby lymph glands
Gastrointestinal anthrax
- Severe abdominal pain
- Nausea
- Vomiting
- Vomiting of blood (during later stages)
- Loss of appetite
- Fever
- Swollen neck
- Diarrhea
- Blood in stool (during later stages)
Symptoms of oropharyngeal anthrax are throat pain and difficulty in swallowing. There are ulcer-like lesions in the mouth cavity. Upon excessive swelling, the airway may become obstructed.
Inhalational anthrax
Symptoms of the most deadly and difficult to treat anthrax form include:
- Flu-like symptoms (sore throat, fever, fatigue, and muscle pain)
- Chest pain
- Breathlessness
- Shock
- Non-productive cough
- Meningitis
- Sweating
- Bluish discoloration of skin
- Vomiting of blood
Complications
The most serious complication of anthrax is anthrax meningitis. This is a fatal condition that occurs when the bacteria reach the brain and the spinal cord through the bloodstream. The membranes covering the brain and spinal cord swell and bleed profusely.
Causes and Risk Factors
B. anthracis bacteria thrive in the following conditions:
- organic and nitrogen-rich soil
- pH greater than 6
- temperatures greater than 60F
Spores can survive in the environment for years and start multiplying once there arefavorable growth conditions. Rainfall or drought triggers spore germination. Humans usually become infected with anthrax from exposure to infected animals or their hides and meat.
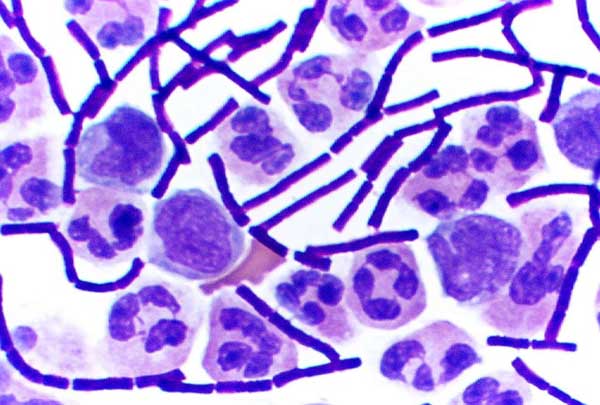
Picture of anthrax bacteria (purple rods) from Wikimedia Commons
Who is at risk?
Direct contact with anthrax spores increases the risk of anthrax. The following factors may play a role:
- Working in an endemic area
- Handling anthrax bacteria or spores in a laboratory
- Handling animal skins, meat, wool or furs
- Working in poorly ventilated rooms
- Underlying lung disease or alcoholism
Diagnosis of Anthrax
After conducting tests to rule out influenza or pneumonia, the following tests may be performed to diagnose anthrax:
- Skin testing or biopsy from the lesion on the skin may detect cutaneous anthrax.
- Blood tests can reveal the presence of anthrax bacteria.
- A computerized tomography (CT) scan of the chest or an X-ray may help in diagnosing inhalational anthrax.
- Endoscopic examination of throat and intestine can diagnose intestinal anthrax.
- Stool sample may reveal the presence of anthrax bacteria
- In case anthrax meningitis is suspected, a spinal tap (lumbar puncture) may be used to withdraw a small amount of fluid from the spinal canal using a needle.
Treatment and Drugs
Treatment depends on the type of anthrax and the age and overall health of the patient.
Medication
- Usually a 2-month course of antibiotics (ciprofloxacin, levofloxacin or doxycycline) is effective in milder cases.
- Inhalational anthrax, however, can be quite challenging to treat.
- Penicillin is preferred for treating inhalational anthrax and anthrax meningitis.
- Inhalational anthrax can also be treated by using a multidrug routine (ciprofloxacin/doxycycline along with tetracycline, rifampin, vancomycin, meropenem, imipenem, chloramphenicol, or clindamycin).
- Amoxicillin is recommended in pregnancy or breastfeeding.
- For patients with severe anthrax, intravenous antibiotics and corticosteroids are recommended.
- Depending on the symptoms, drugs called calcium channel blockers and ACE inhibitors are also recommended in some patients.
Vaccine
The anthrax vaccine does not ensure 100% protection against anthrax bacteria. It is not recommended for pregnant women, children, or elderly.
How To Prevent Anthrax
Apart from the vaccine, other measures that may help in preventing the infection includes :
- Avoiding infected animals, washing with soap and water, decontaminating materials and surfaces help in preventing the transmission and infection.
- For asymptomatic people exposed to anthrax, ciprofloxacin, doxycycline and penicillin are recommended for 2 months to decrease the risk of infection. This also helps in preventing the progression of inhalational anthrax.
References :
https://www.cdc.gov/anthrax/index.html
http://emedicine.medscape.com/article/212127-overview
http://www.merckmanuals.com/professional/infectious_diseases/gram-positive_bacilli/anthrax.html