Bilirubin Levels (High and Low), Blood Test in Adults, Infants
What is Bilirubin?
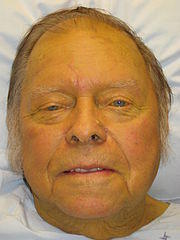
Bilirubin is a byproduct of red blood cell destruction and are conjugated in the liver and excreted in bile. It is the main pigment which is responsible for the color of bile, feces and urine. If the bilirubin in the blood is too high (hyperbilirubinemia), it leads to jaundice or icterus, which is the yellowish discoloration of the skin, sclera, lining of the mouth and other tissues.
Unconjugated Bilirubin
Bilirubin in the Blood
Red blood cells (RBC’s or erythrocytes) are an important component of blood which carry oxygen to cells in the body. These blood cells are destroyed when they become fragile or reach the end of their lifespan which is approximately 120 days. New cells are produced by the bone marrow and replenish the RBC’s in the blood.
When an RBC bursts, it releases hemoblogin into the blood. This is quickly consumed by macrophages, particularly those in the liver (Kupffer cells), spleen and bone marrow. The hemoglobin is further broken down into iron and porphyrin by the macrophages. The iron is released into the blood and stored in the liver as ferritin or used by the bone marrow to produce new red blood cells.
The porphyrin component is converted by the macrophages into bilirubin and this is passed out into the blood. Bilirubin in the blood is unconjugated and is also referred to as free bilirubin. It travels through the blood by binding to the blood protein albumin.
Conjugated Bilirubin
Bilirubin in the Liver
The liver cells, hepatocytes, take up the unconjugated bilirubin and convert it into conjugated bilirubin. It does this by binding the unconjugated bilirubin with glucuronic acid by the action of the enzyme glucuronyl transferase. The hepatocytes then release the bilirubin into the bile which passes out through the hepatic duct and either enters the gallbladder, where it is stored, or enters the duodenum of the small intestine.
The way the liver handles bilirubin and any defect in this process may lead to the different types of jaundice. Sometimes the rapid breakdown of red blood cells as seen in hemolytic syndromes results in a flood of bilirubin in the blood. The liver is unable to cope and the free bilirubin remains in the blood causing jaundice. This is known as hemolytic jaundice.
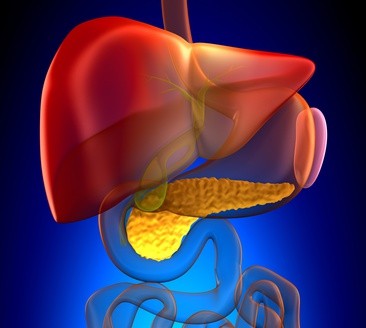
If there is a deficiency or absence of the enzyme glucuronyl transferase the liver cells cannot conjugate the bilirubin and it builds up in the blood stream. This results in non-hemolytic jaundice. When the liver cells are damaged and unable to take up bilirubin from the blood or pass it out into the bile, it results in hepatocellular jaundice.
A backflow of bile due to an obstruction like gallstones or the failure of the liver cells to pass out the bilirubin may also result in an increase in bilirubin within the blood. This will cause cholestatic or obstructive jaundice.
Bilirubin Types
Bilirubin in the Urine, Gut and Stool
Once bilirubin is passed out into the intestine with bile, bacteria in the gut can break down the conjugated bilirubin thereby forming urobilinogen. This is a highly soluble form of bilirubin and can be easily absorbed back into the blood stream from the gut.
The liver takes up most of this urobilinogen and passes it back into the gut. A small amount of urobilinogen is taken up by the kidneys and passed out in the urine where it is oxidized to form urobilin. It gives urine its typically yellow color. The urobilinogen in the gut is also oxidized to form stercobilin. This is passed out in the feces. Bilirubin, along with bile and decomposed food, is responsible for the brown color of feces.
Bilirubin Tests
A bilirubin test assesses the quantity of bilirubin in the bloodstream by measuring the content within a blood sample. Bilirubin is a byproduct of red blood cell destruction and exists in a free form (unconjugated or indirect biliruin) until it is taken up by liver cells. Here it is converted into a soluble form (conjugated or direct bilirubin) by binding with glucuronic acid which is catalyzed by the enzyme glucuronyl transferase.
It is then passed out with bile into the gut and eventually expelled with the stool. A complete bilirubin test will indicate the total bilirubin (direct + indirect) and direct bilirubin. From these two results, the indirect bilirubin levels can be calculated. Depending on regional differences in values and testing methodology in the laboratory, the results may be expressed as mg/dL or mmol/L.
Bilirubin Levels, Values and Readings
The reference range may vary among laboratories. Bilirubin levels higher or lower than the normal values may not require immediate treatment unless it is persistent and reaches levels which are dangerously high.
Adults
- Total Bilirubin
- mg/dL Normal (Reference Range) = 0.3 to 1.0 mg/dL
- mmol/L Normal (Reference Range) = 5.1 to 17 mmol/L
- Direct Bilirubin (Conjugated)
- mg/dL Normal (Reference Range) = 0.1 to 0.3 mg/dL
- mmol/L Normal (Reference Range) = 1.7 to 5.1 mmol/L
- Indirect Bilirubin (Unconjugated)
- mg/dL Normal (Reference Range) = 0.2 to 0.8 mg/dL
- mmol/L Normal (Reference Range) = 3.4 to 12.0 mmol/L
Elevated bilirubin levels in the blood (hyperbilirubinemia) will result in jaundice. Different types of jaundice indicates whether the causative disorder lies before bilirubin enters the liver cells (pre-hepatic), within the liver cells (hepatocellular) or after it leaves the liver cells (obstructive jaundice).
Newborns (Infants)
- Full-Term Baby
- 1 day old (less than 24 hours) = Less than 6.0 mg/dL or 103 mmol/L
- 2 day old (less than 48 hours) = Less than 10.0 mg/dL or 170 mmol/L
- 3 to 5 days = Less than 12.0 mg/dL or 205 mmol/L
- 7 days or older = Less than 10.0 mg/dL or 170 mmol/L
- Premature Baby
- 1 day old (less than 24 hours) = Less than 8.0 mg/dL or 137 mmol/L
- 2 day old (less than 48 hours) = Less than 12.0 mg/dL or 205 mmol/L
- 3 to 5 days = Less than 15.0 mg/dL or 256 mmol/L
- 7 days or older = Less than 15.0 mg/dL or 256 mmol/L
Neonatal jaundice (jaundice in newborns) is not uncommon. The immature liver coupled with rapid destruction of unneeded red blood cells after birth causes an elevation of bilirubin levels in most newborn babies. However, this may not always lead to visible yellow discoloration of the skin and eyes as would be expected in jaundice.
Apart from physiologic jaundice, breastfeeding and breast milk jaundice are other non-pathological causes of jaundice in newborns. Treatment will depend on the cause of the jaundice and bilirubin levels.
References
- Bilirubin. University of Michigan
- Neonatal Jaundice. Medscape