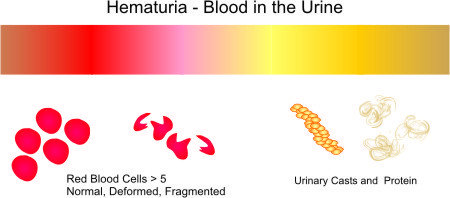
Blood in the Urine (Hematuria) – Location and Causes of Bleeding
The kidneys filter blood to remove wastes, excess water and micronutrients that are not needed by the body. These substances are passed out as urine. Although it is filtered from the blood, the blood cells itself do not enter the urine under normal circumstances. However, there are cases where blood may enter the urine. This may not always be visible to the naked eye but is instead detected by diagnostic tests.
What is hematuria?
Hematuria is the term for red blood cells (RBC’s) in the urine commonly referred to as blood in the urine. This is not a normal phenomenon. There should not be any blood in the urine under normal circumstances. The presence of red blood cells raises the concern about some kidney or urinary tract disease leading to bleeding. Hematuria will not always result in a visible reddish discoloration of the urine.
Often the blood in the urine is so subtle that a person may not be aware of any problem until the urine is tested (dipstick, laboratory urinalysis). It is also important to bear in mind that a red discoloration of the urine may not always be due to blood cells in the urine. Certain foods, drinks and supplements can cause a reddish discoloration of the urine.
Types of Hematuria
There are different terms that are used to describe hematuria depending on the visibility of the blood in the urine.
Gross Hematuria
Visibly discolored urine appearing red or bloody. Sometimes the urine may also appear dark, ranging from a orange-brown to yellow-brown in color. Black urine on the other hand is the presence of free heme (UK ~ haem) in the urine after red blood cells have been destroyed in the blood. While a cloudy urine is a sign of hematuria, it may also indicate the presence of pus in the urine.
Microscopic Hematuria
This indicates red blood cells in the urine that is not visible to the naked eye. Upon microscopic examination, more than 5 red blood cells in urine sediment per high-power field in 3 is evident thereby confirming hematuria.
Isolated Hematuria
This term is used to describe red blood cells in the urine without other urine abnormalities like protein in the urine (proteinuria) or urinary casts (kidney diseases).
Benign Hematuria
The term benign indicates a condition that is not progressing and should not cause any serious complications. Benign hematuria may mean that it is a transient condition and may resolve spontaneously and is a term often used concurrently with essential hematuria.
Benign familial hematuria refers to a genetic type of kidney disease that begins in childhood and results in hematuria because of abnormalities in the kidney’s filtration apparatus known as the glomerulus.
Essential Hematuria
Essential hematuria means blood in the urine due to no known cause. This term may also be used with benign hematuria – benign essential hematuria – to indicate blood in the urine due to unknown causes, that is not progressing or leading to any complications and may resolve spontaneously.
Asymptomatic Hematuria
This is not a term on its own but rather refers to the presence of red blood cells in the urine with no other symptoms like frequent urination, painful urination, urging or incontinence which would normally accompany a pathological urinary disturbance.
Location and Causes
It is not always possible to identify where the bleed is occurring. It could arise from the kidney, ureter, bladder or the urethra. The detection of blood alone is therefore not sufficient. Various other symptoms that may be present must be considered. However, it is more accurate to use diagnostics investigations to identify the location of the bleed.
Bleeding in the Kidney
For blood to enter the urine at the kidney, one or more of the following conditions is usually present.
- Pyelonephritis which is an infection of the kidney.
- Kidney stones.
- Glomerulonephritis in conditions like diabetes.
- Kidney diseases related to the immune system like IgA nephropathy.
- Kidney cancer.
Bleeding in the Ureter
This is an uncommon location for the bleeding but it can occur. A large stone from the kidney can enter the ureter and injure it resulting in bleeding. Another possibility is where a kidney infection may spread down to the ureter. Trauma to the flanks may also involve the ureter which could lead to the presence of blood in the urine.
Bleeding in the Prostate
Blood from the prostate is one of the common causes of hematuria in older men particularly. The prostate may be infected (prostatitis) but another more serious cause is prostate cancer. This is a common cancer among older males. Benign enlargement of the prostate in older men is a common condition and does not usually cause blood in the urine.
Bleeding in the Bladder
One of the most common sites for bleeding which leads to hematuria is within the bladder. From bladder infections (cystitis) to bladder stones, blood from the bladder wall may enter the bladder and taint the urine. The more serious and concerning cause of bleeding in the bladder is cancer. This is a common type of cancer among both older males and females.
Bleeding in the Urethra
The urethra carries urine from the bladder to the external environment. It can be easily injured and infected. In fact most urinary tract infections (UTIs) start as inflammation of the urethra and the spread to the bladder. Sexually transmitted diseases (STDs) is another possible cause. Urinary stones can also injure the urethra as it passes out.
Blood Color in Urine
Gross hematuria does not always mean that the urine will appear red in color. It can appear pink to orange or yellow-brown. Rarely, black urine may also be a sign of hematuria due to free heme in the urine. Sometimes the appearance of red urine or what appears to be blood in the urine is not due to blood. Instead it is a discoloration of the urine. A number of foods and drugs may cause hematuria or urine discoloration. It is often painless in these instances.
Read more on orange discoloration of the urine.
- Foods and Drinks
– Beetroot
– Blackberries
– Rhubarb (red or orange-brown)
– Heavily colored foods and beverages - Drugs
– Rifampicin
– Warfarin
– Metronidazole
– Levodopa (more brown-black)
– Laxative containing senna (more orange-brown)
– Certain antipsychotic drugs