Bone Infection – Acute and Chronic Osteomyelitis
What is osteomyelitis?
Osteomyelitis is an infection of the bone caused mainly by bacteria. The marrow may or may not be involved. Bone is the hardest structure in the human body and often thought to be impermeable to many of the same diseases that affect other parts of the body. However, bone is living tissue that is prone to many of the same diseases like infections as other tissues. Although it is fairly resistant to invading microorganisms, bone may become infected if pathogens reach it via the blood stream or its outer layers are compromised mainly by injury and less commonly by surgery. Although osteomyelitis can occur in any person irrespective of the age, it is more likely to occur in a person with a depressed immune system or serious underlying medical condition.
The main factor for bone to become infected is the entry of microorganisms into the deeper lying spongy bone tissue or even bone marrow. It can enter through a site of injury on the bone, infiltrate the bone directly from a neighboring site of infection or reach the inner layers from the blood stream (hematogenous). Once the inflammation involves the bone marrow, the tissue swells and this swelling is eventually restricted by the hard outer bone. Blood vessels are compressed and the blood flow to the inner bone tissue is severely impaired.This eventually leads to death of the bone tissue and the microorganisms are able to consume this dead material with little interference as the immune cells of the body cannot reach it.
Types of Osteomyelitis
Most cases of osteomyelitis are acute and associated with some preceding injury. Chronic osteomyelitis is where there a recurrent bone infections when the original infection has not been adequately treated or some underlying factor predisposes a person to repeated infections of the bone. Osteomyelitis may also be classified either by the causative organisms, the mechanism by which pathogens reach the bone tissue or by location.
- Pyogenic osteomyelitis is almost always due to bacteria and most commonly by Staphylococcus aureus.
- Tuberculous osteomyelitis is due to Mycobacterium tuberculosis which causes pulmonary tuberculosis (lung TB) from where the microorganisms spread via the blood stream to bone.
- Hematogenous osteomyelitis is a bone infection that arises from blood borne microorganisms.
- Contiguous-focus osteomyelitis is when the infection spreads from surrounding tissue into the deeper layers of the bone. The outer layer of bone is usually compromised by some mechanism for microorganisms to be able to penetrate into the deeper bone tissue. Post-traumatic osteomyelitis is when the infection is preceded by an injury.
- Vertebral osteomyelitis indicates an infection of the bones of the spinal column (veterbrae) and most commonly arises in the lumbar spine.
Causes of Bone Infections
A bone infection may be caused by any number of pathogens – bacteria, fungi or very rarely parasites. Bacteria and mycobacteria are the most common cause and less frequently fungi are implicated in infections. From these bacteria, Staphylococcus aureus is the most common causative pathogen of osteomyelitis. Other bacteria such as Escherichia coli (E.coli), Pseudomonas and Klebsiella species are also responsible for bone infections. It appears that those bacteria with a stronger ability to adhere to bone tissue are more likely to infiltrate it and cause an infection. Most cases of osteomyelitis involves the bones of the lower limbs (leg and feet) mainly in children as well as the vertebrae and pelvic bones particularly in adults.
There are various ways in which an infection of the bone may arise including :
- Fractures particularly a compound (open fracture).
- Soft tissue injury and infection.
- Puncture wounds whether due to an assault, IV drug use or iatrogenic (as part of medical procedure).
- Steel plates and metal pins for repairing fractures.
- Joint prostheses (artificial joint).
- Chronic skin ulcers – diabetic ulcer, arterial ulcer and venous ulcer.
Osteomyelitis is more likely to occur :
- in a person who immunocompromised as is seen with poorly controlled diabetes mellitus (even in the absence of ulcers) and HIV/AIDS.
- where the blood circulation is compromised as with peripheral arterial disease, venous insufficiency and sickle cell disease.
- in patients with chronic conditions that require regular invasive treatments like with dialysis and frequent catheterization.
- in IV drug users.
Symptoms of an Infected Bone
One of the main symptoms is pain at the affected site. This pain is usually felt deep and often described as bone pain. In most cases there is pain preceding the infection of the bone either due to the infected surrounding soft tissue or when there is severe injury at the site. However, in cases of hematogenous spread, there may be no pain for up to one week after the onset of the infection. Therefore pain, or the lack thereof, should not be seen as an absence of an infection. It is more specific than many of the other symptoms of osteomyelitis.
Pain is often accompanied by other localized symptoms such as redness of the skin, swelling and warmth of the area to touch. Sometimes pain is not clearly evident and a person may only experience tenderness upon firm pressure being applied to the area. Generalized symptoms of a bone infection may include :
- Fever
- Chills
- Lethargy
- Fatigue
- Irritability
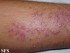
Chronic osteomyelitis can remain undetected for very long periods of times – even months or even years if fungal in origin. Apart from the symptoms above, a sinus tract may form which allows pus to drain onto the surfaces of the skin. The surrounding skin may also have a red rash-like appearance.
Diagnosis of Osteomyelitis
A medical history with symptoms suggestive of osteomyelitis and any known predisposing factors along with laboratory studies may be sufficient to reach a diagnosis. Laboratory studies include a complete blood count (CBC) and the assessment of the ESR and C-reactive protein levels. An x-ray or CT scan may allow for radiographic identification of the site of infection but this can sometimes be undetectable with these diagnostic investigations for up to 3 weeks after the onset of an infection. Collecting a sample of the surrounding tissue or even bone (biopsy) and sending the sample for cytology and culture may also be advisable.
Treatment of a Bone Infection
The treatment largely depends on the cause and since most cases are bacterial in nature, broad-spectrum antibiotics are usually prescribed. Due to the characteristics of bone, these antibiotics are often administered intravenously and later followed by oral antibiotics. Antifungal drugs are necessary for fungal infections of the bone.
Dead tissue may need to be debrided, abscesses drain and in very severe cases and as a last resort the affected limb may be amputated. Where necessary normal blood flow must be restored to the affected area as soon as possible to allow for proper healing.
Reference
- Osteomyelitis. Medscape Reference