Bursitis (Inflamed Bursa) Causes, Symptoms, Treatment, Surgery
There are several areas in the body where certain organs and structures may move against each other thereby causing friction. Where two bones meet to articulate, the area has specialized cartilage and fluid within a capsule to reduce friction. This is known as a joint. At other sites like between between muscles, tendons, bones and skin, there are specialized flattened sacs of fluid to reduce friction of the movement of the opposing structures. These specialized sacs are known as bursa (singular) or bursae (plural). There is some 160 bursae found at several locations throughout the body and especially around the major joints. In fact the bursae are not extremely dissimilar from the joints in the type of tissue and fluid within it. The bursae are lined with a synovial membrane and secrete a a synovial fluid as is the case in the joint.
What is bursitis?
Bursitis is the medical term for inflammation of the bursa or bursae. It can affect the superficial or deep bursae in the body. Apart from the pain or tenderness, redness of the skin and swelling at the affected site, bursitis also affects normal movement of the structures in the region. Over time if left untreated and should bursitis persist, there may be severe restriction of movement over a long time thereby hampering the quality of life. Eventually it can cause permanent deformity at the site. The most commonly inflamed bursae includes :
- subacrominal bursitis (shoulder bursitis)
- olecranon bursitis (elbow bursitis)
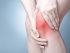
- trochanteric bursitis (hip bursitis)
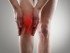
- prepatellar and infrapatellar bursitis (knee bursitis)
How does bursitis occur?
Bursitis may be acute or chronic and there are several causes of inflammation of the bursae. The most common cause of chronic bursitis is trauma usually related to repeated use and strain. Normally there is only minute amounts of synovial fluid within the bursae. However, in response to ongoing inflammation, the number of synovial cells increases. This therefore increases the amount of collagen and fluid in the bursae. In addition, the inflammatory process increases the permeability of capillaries in the area allowing more high protein fluid within the bursa. Depending on the severity of the condition there may be some bleeding. Over time, the lining of the bursae can develop scar tissue.
Bursitis Video
Bursitis Causes
Some of the more common causes of bursitis includes :
- Acute injury like falls or knocks.
- Repetitive trauma and strain
- Infection (acute or chronic) known as septic bursitis most commonly caused by Staphylococcus aureus.
- Crystal- induced like gout or pseudogout
- Inflammatory systemic diseases like rheumatoid arthritis, psoriasis and systemic lupus erythematosus (SLE)
The causes may be more specific for certain common locations.
Shoulder Bursitis
Shoulder bursitis may arise with an injury like after lifting a heavy bag or in professional sportsmen and sportswomen particularly with throwing heavy weights.
Elbow Bursitis
Olecranon bursitis (elbow bursitis) may arise with a sharp blow to the ‘elbow bone’ and with repeatedly leaning on the elbow. The latter is more commonly seen in students who tend to lean on one elbow when studying or in classes. It is therefore known as student’s elbow.
Hip Bursitis
Activities like running, cycling and climbing stairs can strain the bursa. Falls especially in the elderly and previous hip surgery are also other possible causes of hip bursitis.
Knee Bursitis
Knee bursitis may occur with constant kneeling (clergyman’s or housemaid’s knee) due to the occupational hazards. Another type of knee bursitis known as jumper’s knee occurs with jumping injuries and is more likely to be seen in athletes.
Bursitis Symptoms
There is usually a history of injury, repetitive movements or other inflammatory diseases. The characteristic symptoms of bursitis includes :
- Redness of the overlying skin (more likely in superficial bursitis).
- Swelling just under the skin (also more prominent in superficial bursitis).
- Tenderness isolated to the affected site.
- Pain which is more prominent with movement.
- Decreased range or motion.
- Difficulty bearing weight.
Fever is a non-specific symptom that is more likely to be seen with septic bursitis (infection).
Bursitis Treatment
The treatment of bursitis depends on the underlying cause and even the affected site to some degree. Conservative measures that may be helpful includes :
- Resting the limb.
- Immobilizing the limb.
- Hot and cold therapy.
- Occupational therapy to ease strain on the bursa.
Medication
- Non-steroidal anti-inflammatory drugs (NSAIDs) are usually the first line of treatment in non-infectious (aseptic) bursitis. It helps to reduce inflammation and pain until the bursa can rest and repair.
- Intrabursal steroid injections where corticosteroids are injected into the bursa. It rapidly reduces inflammation and pain.
- Antibiotics for septic bursitis with the appropriate antibiotic for Staphylococcus aureus, the most common infectious agent.
Surgery
- Aspiration is the withdrawal of fluid or pus in the bursa. Fine needle aspiration is a minor procedure that is the first choice for draining the bursa. Should this fail, incision and drainage may then be considered.
- Excision of the bursa (surgical removal) is only considered once other treatment measures fail to yield the desired results in chronic or recurrent bursitis, particularly once there is scar tissue formation or deformity.