Calcified Aortic Valve and Mitral Heart Valve Calcification
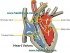
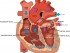
The heart valves are important structures in the heart and at its junction with the major arteries. By opening and closing at different stages of heart contraction, these valves ensure that blood flows in one direction through the heart. There are four main valves in the heart and blood vessels – one between the atrium and ventricle on each side (atrioventricular or AV valve) and one in each large artery that carries blood out of the ventricles (semilunar valve).When the valve closes, blood cannot flow backward (regurgitation) but also needs to open fully and not impair flow of blood in the correct direction.
Blood that is low in oxygen (deoxygenated blood) enters the right atrium of the heart and then empties into the right ventricle. The tricuspid valve lies between the right atrium and right ventricle. When the ventricle contracts, the blood flows to the lungs through the pulmonary artery and the tricuspid valve closes to prevent backward flow. The pulmonary valve, also know as the pulmonic valve, lies at the root of the pulmonary artery. When the right ventricle relaxes and prevents backward flow from the aorta.
The same valves lie on the left side. Oxygen-rich (oxygenated) blood returning from the lungs empty into the left atrium and then fill into the left ventricle. When the left ventricle contracts in order to push out the blood through the aorta and to the rest of the body, the bicuspid valve between the left atrium and ventricle closes. This valve is also known as the mitral valve. The blood can then flow straight out of the left ventricle and into the aorta. Once the left ventricle relaxes, the aortic valve ensures that there is no backward flow of blood from the aorta into the left ventricle.
Therefore valves ensure that all the blood flows in one direction – from the atrium, into the ventricle and then into the great artery to its destination. The valves have to be flexible to open and allow blood to flow through uninterrupted when necessary, yet be firm enough to create a seal to prevent backward flow.
What is a calcified heart valve?
A calcified valve, or valve calcification, is the hardening of the valve due to the deposition of calcium salts at the site of wear-and-tear and damage. Heart valves experience significant wear-and-tear throughout life. It opens and closes with every heart beat and has to withstand the pressure of blood traveling at force to prevent any backward flow. The pressure is greater in the left side of the heart so these valves experience more wear-and-tear. After decades, the cumulative effects of prolonged wear-and-tear damages the valves and increases the risk of calcium phosphate salts depositing on it. This is known as dystrophic calcification.
It is important to remember that any valve can become calcified. However, calcification is more likely to affect the valves on the left side of the heart – mitral valve and aortic valve – because it experiences greater pressure than the valves on the right side of the heart. Calcification is not an overnight process. It occurs over decades and is the reason why heart valve calcification is more often seen after the age of 50 years. The longer human lifespan in this day and age means that heart valve calcification is more frequently seen than it was even half a century ago. The mitral valves tend show significant calcification by 50 to 70 years while the aortic valve in the 70th to 90th year of life. It is therefore referred to as senile valve calcification but can occur earlier in life, particularly when associated with conditions like rheumatic heart disease, endocarditis and other causes of heart valve disease.
Calcified Aortic Valve
When the aortic valve is affected by calcification, it is known as calcific aortic stenosis. This valve has three cusps but in some people it may only be made up of two cusps and this is known as a congenital bicuspid valve. While both a two or three cusp valve may be affected by age-related changes and wear-and-tear, it is the bicuspid valve that bears greater stress and strain and therefore more likely to become calcified.
Studies suggest that the valves may not transform from an otherwise normal valve into a calcified valve over time as it was previously thought. Instead it may undergo several different stages of degenerative changes similar to atherosclerosis. Eventually calcification causes it to harden and narrow. However, in light of these different stages of degenerative changes, it is therefore likely that elevated levels of cholesterol and other fats (hyperlipidemia) and high blood pressure (hypertension) may also play a role in calcification of the aortic valve as is the case with atherosclerosis.
The aortic valve closes when it is filled with blood from the initial backward flow of blood at the end of ventricular contraction (systole). The free margin is usually spared of any calcification but the parts of the cusps near its point of attachment are most affected. These are the flexible parts of the valve that experience the most amount of bending when the cusps open and close. The calcific deposits are large nodular deposits that cause an obstruction to the outflow of blood.
A calcified aortic valve severely disrupts the normal heart functioning and cardiac output. The heart has to compensate by enlarging the muscle of the left ventricle (hypertrophy). The ventricle is now able to pump harder and the pressure within it increases substantially at contraction, significantly above the norm. However, the muscle wall also needs a greater blood supply but is generally deprived of sufficient oxygen particularly at times of activity leading to myocardial ischemia. Patients develop angina (pain with myocardial ischemia), signs of congestive heart (decreased cardiac output and water retention) and may have fainting spells at times of stress when a greater cardiac output is required. Once angina and/or congestive heart failure is present in a patient with aortic stenosis, heart valve replacement is required or death may occur within 5 years or less.
Calcified Mitral Valve
Calcification of the mitral valve does not have the same clinical severity as that of the aortic valve. The calcified deposits usually lie behind the leaflets of the mitral valve and do not impair valvular function. Most patients are therefore asymptomatic. It tends to develop in the peripheral fibrous ring of the valve known as the mitral valve annulus. Therefore calcification of this valve is usually referred to as mitral annular calcification.
It can cause regurgitation when the ability to contract and return to its normal position is impaired due to calcification. Furthermore there may be a narrowing as the calcific deposits may prevent the valve from opening fully when the ventricles relax. Mitral valve calcification can, however, affect other aspects of cardiac physiology and serves as a risk factor for other diseases :
- Calcific deposits may penetrate the heart wall and affect the electrical conduction system of the heart.
- Calcific deposits may provide a site for blood clot formation (thrombus) which can later dislodge (embolus) and lodge in arteries like the carotid artery thereby leading to a stroke.
- Calcific deposits may provide a convenient site for bacteria to multiply in infective endocarditis.