Cold Injury (Freezing and Non-Freezing Damage)
What is a cold injury?
A cold injury is any disruption of internal processes, damage or death to tissue and associated complications that results from exposure to cold. This includes cold weather, cold water, snow, ice and liquid gas. Although the body has various means to tolerate and cope with cold, minimize damage and regulate the internal temperature, there comes a point where this is insufficient. Cold injury is dependent on the temperature of the environment or substance and the duration of exposure. The injury may also be determined by clothing and other other protective gear that can play a role in minimizing the severity of the injury.
Cold Injury Types
There are two ways of classifying cold injury. Firstly it is based on whether a part of the body or the entire body is affected. Secondly it is determined by the degree of cold exposure and whether the tissue fluids freeze or not.
Localized or Systemic
- Localized cold injury means that only a part of the body is affected or sometimes several parts. The extremities are obviously the most likely to be affected as it is the farthest away from the trunk where most of the body heat is generated. Furthermore heat is lost in transit to the extremities and in most instances it is the extremities that are most exposed or in contact with cold. Therefore it is also known as peripheral cold injuries.
- Systemic hypothermia is where the entire body is affected as the core temperature drops below 35 degrees Celsius or in severe cases it dips lower than 32 degrees Celsius. All organs and structures are affected and the most significant impact may be noted in the cardiovascular system (heart and blood vessels circulating blood) and the central nervous system (brain and spinal cord). Hypothermia is not discussed further in this article as it is separate and extensive syndrome.
Freezing and Non-Freezing
Freezing and non-freezing injuries depend on whether the tissue fluid freezes or not. Severe and serious damage occurs when there is freezing. Ice crystals form outside the cells in the surrounding tissue fluid thereby dehydrating the cell. Fluid is the main medium in the body for all processes and once it freezes, exchange of nutrients, gases and other biochemical processes will cease. Tissue death is inevitable.
Non-Freezing Cold Injury
The two types of non-freezing cold injuries are chillblain (pernio) and immersion foot (trench foot). Although frostnip is a milder form of cold injury than chillblains, it is discussed further under freezing cold injury as it is a form of mild frostbite.
Chillblain
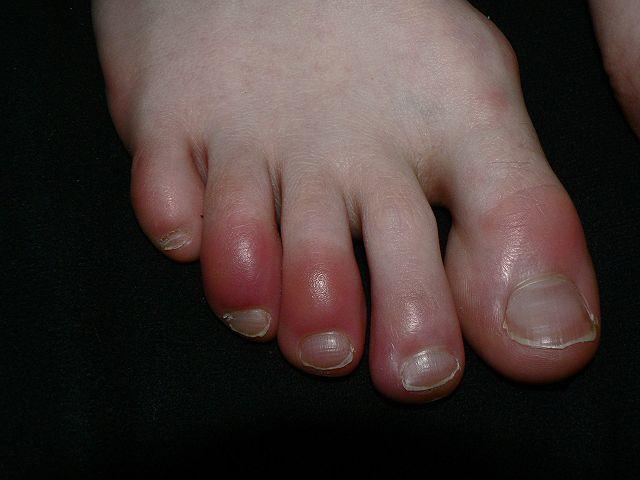
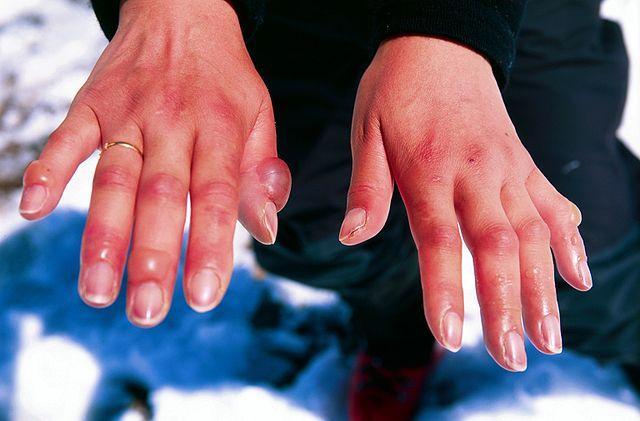
This type of cold injury arises with exposure to temperatures that do not cause freezing of the tissue fluids. It includes damp condition. The injury to the tissue is largely reversible. Blood vessels become inflamed and red raised lesions form on the skin. Sometimes blisters, erosions and ulcers may form on the skin surface.
Picture of chillblain from Wikimedia Commons
Immersion foot
Immersion foot, also known as trench foot, occurs with prolonged exposure to wet conditions although it is not freezing temperatures. The feet are most commonly affected and this condition was widely seen in the trench battles of World War I. The heat loss may reduce the temperature to almost freezing point. Blood vessels and nerves are affected.
Freezing Cold Injury
Frostnip
This type of cold injury is the mildest. It is seen as a prelude to frostbite. In frostnip the outer layers are affected and is also known as superficial frostbite. If there is intervention, then frostbite can be prevented.
Frostbite
This is the most severe type of cold injury. There are several effects that arise with this type of cold injury. The cold causes direct tissue damage, ice crystals also damages cells, dehydration of cells are seen with ice crystal formation, blood flow slows, blood clots form and there is ischemia (injury) with inadequate oxygen supply of the affected tissue. There are four stages of frostbite with the fourth being the most severe where tissue death occurs.
- First-degree frostbite – redness and swelling.
- Second-degree frostbite – large clear blisters along the length of the affected area.
- Third-degree frostbite – large blood-filled vesicles.
- Fourth-degree frostbite – tissue death (necrosis) and gangrene.
First and second degree frostbite are limited to the skin and subcutaneous tissue. Therefore it is also known as superficial frostbite. Third and fourth degree frostbite affects deeper tissue like the muscles, tendons, blood vessels and nerves. It is also referred to as deep frostbite.
Picture of frostbite from Wikimedia Commons
Cold Injury Causes
Although the causes are largely the same for all types of cold injury, there may be slight variations in that certain causative factors are more likely to cause one cold injury rather than another. The temperature exposure and duration are other factors that need to be considered in the type of injury. However, in broad terms cold injury is due to exposure to or contact with :
- Weather – cold, wet and windy
- Ice and snow
- Liquid gases like liquid nitrogen
- Immersion in running or standing water
- Freezer
- Frozen metal
Risk Factors
There is a greater risk of cold injury with a lack of protective gear, inadequate thermal clothing and inappropriate shelter with insulation. There are also various physiological (non-disease changes in the body) and pathological (diseases) factors that also increase the risk of cold injury.
- Old age
- Alcohol misuse
- Anorexia nervosa
- Arthritis
- Diabetes mellitus
- Head trauma
- Illicit drug abuse
- Immobilization
- Infections
- Malnutrition
- Peripheral vascular disease
- Prescription medication
- Psychiatric illness
- Raynaud phenomenon
- Severe exhaustion
- Stroke
- Thyroid disease
Cold Injury Symptoms
The different signs and symptoms seen with cold injury have been discussed under the freezing and non-freezing types. Some of these symptoms develop in specific stages that arise over time. However, as a general overview, the signs and symptom of peripheral cold injury includes :
- Numbness and tingling
- Burning and severe pain
- White to blue discoloration of the skin
- Redness and swelling of the affected part
- Blisters, erosions and ulcers
- Necrosis and gangrene
- Loss of function of the affected part
Cold Injury Diagnosis
Cold injuries are a clinical diagnosis meaning that it is made based on the presence of signs and symptoms indicative of a cold injury with a recent history of cold exposure. The severity of the tissue damage is indicative of the temperature and duration of exposure. Further tests may not be necessary but can be helpful in identifying the extent of the injury and biochemical changes in the body as a consequence of cold exposure.
These investigations may include :
- Blood tests – CBC count, sedimentation rate, serum protein electrophoresis (SPEP) and quantitative immunoglobulins. These tests are mainly useful for chillblains. Overall blood tests have little value in diagnosing and assessing frostbite.
- X-ray
- CT scan
- Angiography
- Scintigraphy
- Bone scans
Cold Injury Treatment
The goals of treatment for cold injuries include :
- Preventing further heat loss and exposure to cold by dressing the site, using appropriate clothing and providing insulation.
- Rewarming the area is done by the use of warm water and whirlpool baths (hydrotherapy).
- Restoring or improving blood flow by using warmth, anti-clotting and clot busting agents.
- Increasing oxygen perfusion through hyperbaric oxygen therapy.
- Preventing infections and other injuries to the damaged area by administering antibiotics, dressing the wound and avoiding use of the affected area.
- Removing dead tissue through debridement although this is limited to superficial injuries. Removal of the affected area (amputation) where there is deep necrosis and gangrene.
Cold Injury Rewarming
This is one of the single most important measures in treating and managing cold injury. Rewarming may require gentle heat and massage for non-freezing injuries while conditions like frostbite needs more controlled techniques. Warm water may be used to bathe the area thereby thawing the tissue in frostbite. Direct heat should never be applied to the skin as it can cause burns. Although warm water baths are widely used, whirlpool baths where the water is constantly circulating are preferable. This ensures that the water is maintained at a constant temperature. Passive or active rewarming may also be necessary if there is systemic hypothermia. This involves the use of thermal blankets to help the body temperature increase on its own (passive), or addition of heat to assist in restoring the body temperature (active).
Superficial frostbite may require between 15 to 30 minutes of rewarming whereas up to 1 hour of rewarming may be needed for deep frostbite. Insufficient rewarming is one of the main shortfalls in treating frostbite in the early stages. However, rewarming is not advised if there is a chance of re-exposure to cold and likelihood of frostbite recurring. Massage of the affected area should be avoided in frostbite. Rewarming will lead to pain as inflammation arises and the nerve activity gradually restores. Ibuprofen, acetaminophen and aspirin are milder drugs that may help with pain management but in severe cases, opioid analgesics like morphine may be required.
References :