Complications After A Heart Attack (Myocardial Infarction)
About half of the deaths associated with a heart attack occurs within the first hour and these patients never reach the hospital. Not every myocardial infarction (heart attack) is fatal and the advances made in modern medicine has drastically reduced the mortality associated with a myocardial infarction. However, there is no avoiding that fact that a heart attack is a serious clinical event that permanently compromises heart function to some degree for the rest of the patient’s life. There are several complications that arise immediately after a heart attack and within days and even months thereafter, some of which may be life-threatening in the short to long term. All these complications further compromise the heart function and contribute to the overall presentation of the heart disease following a heart attack.
Overview of a Heart Attack
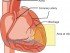
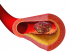
A heart attack (acute myocardial infarction) is death of a portion of the heart muscle due to inadequate blood supply. Most cases are due to coronary artery disease, where the arteries carrying oxygen and nutrient rich blood to the heart wall is partially occluded. Atherosclerosis is the most common cause and these fatty plaques gradually enlarge in size over long periods of time. During times of increased cardiac demand, the blood supply to the heart is insufficient. The heart is therefore deprived of oxygen and nutrients resulting in damage but not death of heart muscle (myocardial ischemia). A person may live for years or even decades with this type of ischemic heart disease.
Generally the atheromatous plaque or plaques in the wall of the coronary artery is stable. However, it may suddenly rupture and trigger the formation of a platelet plug and blood clot at the site. This is when the blood supply to the heart muscle is severely compromised leading to death of the area of heart tissue supplied by the occluded part of the coronary artery. There are other causes like an embolus, vasospasm and even systemic disturbances but these are less common causes of a myocardial infarction. If there is early intervention and the obstruction is not severe, then the extent of the damage and subsequent necrosis (tissue death) is not extensive. A person may not be at risk of death from the infarct. However the heart function is always compromised to some extent in the future. While the damage associated with an interrupted blood supply (ischemia) is reversible, particularly with reperfusion, death of the heart muscle is irreversible.
Consequences of a Heart Attack
A heart attack has a number of clinical consequences which arises within minutes, hours and even days after an infarct. Some of these complications may only become apparent several weeks after the infarct when it reaches a point that it leads to evident signs and symptoms. Therefore proper monitoring particularly within the hospital environment and frequent follow up consultations as advised by the attending doctor is essential.
Contractile Dysfunction
The ability of the infarcted part of the heart to contract is severely compromised and this means that the function of the left ventricle (the most commonly affected area) is hampered. Ultimately the rest of the heart has to work harder to pump out blood and this is not to the same extent as that of a healthy heart. The degree to which the contractility is affected is dependent on the size of the infarct – the larger the infarct, the more severe the contractile dysfunction.
Blood through the heart backs up and fluid escapes into the lungs (pulmonary edema). A large infarct usually involving 40% or more of the left ventricle can lead to cardiogenic shock. This means that the body does not receive a sufficient supply of oxygenated blood due to the inability of the heart to push out this blood. Majority of patients with cardiogenic shock will not survive even in the hospital setting.
Irregular Heart Beat
The heart has a natural pacemaker known as the sinoatrial (SA) node). Impulses generated here spread directly across the atrial muscle causing it to contract, and after a short delay, the impulse passes along the ventricular muscle which then contracts. These impulses need to have a healthy electrical system to be generated and distributed. However, it is also dependent on healthy cardiac muscle for its transmission. With a myocardial infarction, a portion of its normal line of transmission is affected and this leads to an irregularity in the heart beat known as an arrhythmia.
Arrhythmias are an irregular rate and/or rhythm of the heart beat that tends to occur in short periods. Some arrhythmias, like the type that arise after a myocardial infarction, is potentially lethal. It is more likely to occur if the infarct is in the area of the conduction system, typically in the lower part of the septum dividing the two sides of the heart.
Pericarditis
Pericarditis is inflammation of the lining of the sac that encloses the heart. This double-layered sac is known as the pericardium. A small quantity of pericardial fluid is contained within this sac that lubricates the two opposing layers when the heart contracts and relaxes.
Although a portion of the heart muscle dies with a myocardial infarction, other areas, particularly around the infarct becomes inflamed. The process of inflammation increases the permeability of local blood vessels and allows excess fluid, fibrin and even blood to leak into the pericardial sac which irritates the lining. This is known as Dressler syndrome and occurs two to three days after a heart attack.
Cardiac Rupture
The part of the heart muscle that dies (area of necrosis) is surrounded by inflamed heart muscle. The necrotic area weakens and softens and can rupture. The size of the subsequent ‘hole’ depends on the extent of the infarct. Blood can leak out of the heart and into the surrounding sac (pericardial sac) that surrounds the heart. The accumulation of blood within the pericardium is known as a hemopericardium and may compress the heart (cardiac tamponade).
A cardiac rupture tends to occur several days after the infarct. It does not affect every patient who has a heart attack but is more likely to occur in :
- Females over the age of 60 years
- Pre-existing hypertension (high blood pressure)
- Patients with previous infarcts
Aneurysms of the Heart
Sometimes the outer layer of the heart wall (epicardium) and the pericardial lining adhere to the area of the myocardial rupture. This prevents blood from escaping from the heart and essentially forms a type of aneurysm – ballooning. In this case it is known as a false aneurysm. Sometimes the myocardium weakens but does not rupture and then balloons outwards. It is then known as a true aneurysm.
Clot in the Heart
Blood begins to clot if it is not constantly in motion, experiences any turbulent flow or makes contact with a damaged inner lining of the heart or blood vessel. With a myocardial infarction, the disturbance in heart contraction and at times damage to the inner lining of the heart (endocardium) contributes to clot formation (thrombus). The clot known as a mural thrombus may dislodge and travel to other sites (embolus) where it can obstruct local arteries.
Expansion of the Infarct
The necrosis that occurs with the infarct may expand and involve surrounding healthy, although inflamed, heart muscles. In this way the size of the infarct increases and can further compromise heart function or even lead to death. Weakening of the necrotic area may stretch thereby increasing the size of the area although surrounding tissue does not die.
Mitral Valve Dysfunction
The mitral valve allows blood to flow from the left atrium to ventricle but prevents any backward flow (regurgitation). The leaflets of the valve are attached by the chordae tendinae to papillary muscles that holds the valve leaflets in position when under pressure. An infarct may shorten, damage or even rupture the papillary muscle and the support to the mitral valve leaflets is compromised. Blood may then flow backward (mitral regurgitation) into the left atrium during contraction of the left ventricle. Insufficiency of the mitral valve may also occur after an infarct if the ventricle dilates and the valve leaflets are spread apart.
Heart Failure
Acute heart failure may occur within minutes of severe myocardial ischemia (damage but not death of the heart muscle). Progressive heart failure is ongoing and persists for years after an infarct. The ability of the heart to pump out blood is gradually compromised further and associated with enlargement of the left ventricle. It can remain silent for long periods of time and therefore regular monitoring after an infarct is crucial.