Congested Sinuses , Sinus Inflammation and Infection (Sinusitis)
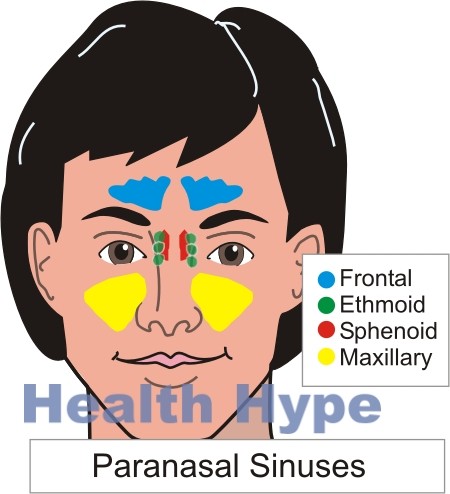
The paranasal sinuses are hollow air-filled cavities in the skull. There are four pairs of paranasal sinuses known as the frontal, sphenoid, ethmoid and maxillary sinuses. These cavities are lined with a mucous membrane and its secretions usually drain through small openings (ostia) into the nasal cavity. Since the sinuses are essentially continuous with the nasal cavities, it is prone to the same disease that affect the nasal lining. Its narrow openings, however, maintain a sterile environment within the paranasal sinuses and ensures that secretions constantly drain out without any backward flow from the nasal cavity.
What is sinusitis?
Sinusitis is the term for inflammation of the paranasal sinus. The inflamed sinus becomes congested with mucus as well as with pus in infectious cases of sinusitis. Inflammation of the nasal cavity (rhinitis) often precedes and exists along with sinusitis and it is therefore jointly referred to as rhinosinusitis.
How does sinusitis occur?
Sinusitis may occur through one of three mechanisms and are most likely due to a combination of factors.
- Inflammation of the tissue lining the sinuses, and at its opening, causes it to swell. The drainage of mucus from the paranasal sinuses are therefore hampered and collects within the sinus cavity. This obstruction may also be due to other physical causes like nasal polyp or foreign body in the nose.
- The passage of mucus out of the paranasal sinus is aided by the action of cilia – tiny hair-like projections from epithelial cells. The beating of the cilia aids the movement of mucus in one direction (unidirectional) from the sinus to the nasal cavity. Certain causes like genetic disorders, bacterial toxins and viral attachment may disturb the beating action thereby hampering normal sinus drainage.
- Inflammation of the paranasal sinus tissue may cause excessive secretion of mucus which may be thicker than normal. The mucus does not drain as fast as it normally would and are more likely to obstruct the sinus openings (ostia) thereby allowing for sinus congestion.
Despite the different mechanisms, the underlying pathophysiology indicates a blockage of the paranasal sinus openings (ostia) which allows for mucus to accumulate in the sinuses. Infections, particularly secondary bacterial infections, tend to arise in these settings.
Types of Sinusitis
Sinusitis can be classified in several ways but the most common is by duration – acute, subacute or chronic. Acute sinusitis is where the inflammation and symptoms completely subside within 30 days. Subacute sinusitis lasts for 30 to 90 days and chronic sinusitis persists for more than 90 days (or 12 weeks). A further sub-classification is recurrent sinusitis which may involve multiple episodes of sinusitis that completely resolves only to recur within 10 days. Furthermore it may be classified by etiology (cause), pathogenic (microorganism) and location (anatomical).
- Etiology – infectious, allergic or obstructive (usually leading to infection)
- Pathogenic – viral, bacterial or fungal
- Location – frontal, ethmoidal, sphenoidal or maxillary
Causes of Sinusitis
There are a number of causes of sinusitis but infections are the most common. From these cases, viral infections are the most common in acute sinusitis. With the diverse causes and predisposing factors in chronic sinusitis, secondary bacterial infections may then set in.
Infections
- Viral sinusitis is almost always associated with viral upper respiratory tract infections involving the nasal cavity (rhinitis). This may be due to a number of viruses including rhinovirus, parainfluenza, influenza A and B, enterovirus, respiratory syncytial virus (RSV) and adenovirus. It is most frequently seen with the common cold. Inflammation of the sinuses and sinus congestion predisposes the patient to a secondary bacterial infections.
- Bacterial sinusitis may be due to streptococci, staphylococci, Hemophilus influenzae, Pseudomonas aeruginosa and Moraxella catarrhalis. Both acute and chronic sinusitis are frequently associated with secondary bacterial infections. Tuberculosis may be the cause of sinusitis in patients with HIV.
- Fungal sinusitis is mostly seen in immunocompromised patients – mucormycosis in long term diabetics (diabetes mellitus) and aspergillosis or candidiasis in HIV/AIDS. Fungal infections tend to cause chronic sinusitis. More commonly fungi in the paranasal sinuses trigger an allergic reaction.
Allergies
Allergic sinusitis is more frequently seen in patients with an allergic constitution (atopy). With allergic rhinitis, it may be throughout the year (perennial) or only exacerbate during certain periods (seasonal). Inhaled allergens such as dust, pollen and animal dander are common triggers. The condition is further exacerbated by secondary bacterial infections that may require acute treatment.
The presence of fungi within the paranasal sinus may also cause an allergic reaction. In these instances, the fungi do not invade and infect the sinus as is seen in immunocompromised patients.
Other
Other causes often create conditions that eventually lead to a sinus infection. Most notable among these other causes is an obstruction caused by a nasal polyp, tumors, a deviated septum or following trauma where a fractured facial bone obstructs the opening of the sinus.
In addition, the following causes and risk factors may play a role in both acute and chronic sinusitis :
- Non-allergic rhinitis
- Hormonal factors – pregnancy, oral contraceptive
- Gastroesophageal reflux disease (GERD)
- Dental diseases
- Cystic fibrosis
- Kartagener syndrome
- Cigarette smoking
- Environmental pollution
- Occupational exposure to airborne irritants
- Cocaine inhalation (snorting cocaine)
Signs and Symptoms of Sinusitis
The most prominent feature is congestion of the sinuses which leads to similar symptoms in both acute and chronic cases. This includes :
- Nasal discharge – thick, yellow to green and often offensive
- Runny nose and nasal congestion
- Facial pain and discomfort (feeling of fullness / pressure)
- Facial swelling and redness of skin over the affected area
- Loss of smell and/or taste
- Headache
- Fever and chills is seen with an infection
- Fatigue
Other symptoms may include :
- Sore throat
- Ear pain
- Bad breath
- Snoring
Symptoms may be more specific for congestion of certain paranasal sinuses.
- Maxillary sinusitis
- Cheek pain
- Toothache
- Frontal headache
- Frontal sinusitis
- Frontal headache
- Eye pain
- Ethmoidal sinusitis
- Pain between and behind the eyes
- Swelling around the eye and may involve the eyelid
- Excessive tearing
- Sphenoidal sinusitis
- Vague headache varying from the front, back or even top of the head
- Classic symptoms of sinusitis such as a runny nose/nasal congestion may be absent
References :
Sinusitis. Merck Manuals (www.merckmanuals.com)