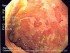
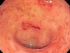
Crohn’s Disease vs Ulcerative Colitis Differences and Cancer Risk
Inflammatory bowel disease (IBD) is estimated to affect about 1 to 2 million Americans. It not only affects a person’s quality of life but one type of IBD is also be associated with an increased risk of colorectal cancer. Despite its name, inflammatory bowel disease may not only affect the bowels (small or large intestines). There is a type of IBD that can occur anywhere in the gastrointestinal tract, from the mouth to the anus.
Read more on inflammatory bowel disease.
It is important to understand the differences between the two types of inflammatory bowel disease – Crohn’s disease and ulcerative colitis. There are many similarities but also differences that account for the two distinct types of inflammatory bowel disease (IBD). It is important to note that inflammatory bowel disease (IBD) is a distinct condition and should not be confused with the various other digestive conditions that may present with similar symptoms.
How are Crohn’s and Ulcerative Colitis Similar?
Both Crohn’s disease and ulcerative colitis are types of inflammatory bowel disease (IBD). This is a chronic inflammatory disease meaning that inflammation occurs in the bowels over a long period of time. There may be episodes of remission and flareups over this time.
The inflammation causes a host of signs and symptoms as well as affects function of the affected portion of the digestive tract. It can also lead to complications including the formation of holes (perforation), narrowings (strictures), abnormal channels (fistulas) and even increase cancer risk.
Although the exact cause is unknown, inflammatory bowel disease appears to be an autoimmune condition. This means that the immune system malfunctions and attacks the lining of the bowels or other parts of the gastrointestinal tract.
Despite these similarities in the possible cause and nature of the two different types of inflammatory bowel disease (IBD), there are also several differences. The location, severity of inflammation and even symptoms may vary between Crohn’s disease and ulcerative colitis.
Differences in Crohn’s Disease and Ulcerative Colitis
Inflammatory bowel disease and the type of IBD should be diagnosed by a medical professional. This usually requires diagnostic investigations such as stool tests, imaging techniques like MRI or CT scans as well as endoscopic investigation with/without biopsy. Some of the following features need to be identified in order to differentiate between ulcerative colitis and Crohn’s disease.
Read more on ulcerative colitis and Crohn’s disease.
Location
Ulcerative colitis is isolated to the colon, the main part of the large intestine. The term colitis means colon inflammation. It is often thought that inflammatory bowel disease (IBD) can only affect the bowels – the small or large intestines. However, Crohn’s disease can affect any part of the digestive tract from the mouth to the anus.
The inflammation in ulcerative colitis is limited to the inner lining of the colon. In Crohn’s disease, this inflammation can extend through the entire thickness of the gut wall. In addition the inflammation in Crohn’s disease is patchy meaning that there are areas of healthy tissue among the inflamed tissue. In ulcerative colitis the infammation is continuous in the affected area.
Symptoms
The symptoms of both types of inflammatory bowel disease (IBD) are largely the same. However, it may vary between Crohn’s disease and ulcerative colitis depending on the location and severity. Ulcerative colitis symptoms are related to the colon whereas Crohn’s disease symptoms depend on the portion of the digestive tract that is affected.
Common symptoms of both ulcerative colitis and Crohn’s disease include:
- Abdominal pain and cramps
- Bloating
- Diarrhea (sometimes constipation)
- Mucus in the stool and sometimes bloody stool
- Nausea and sometimes vomiting
- Weight loss
Even with these common symptoms there may be some variation among Crohn’s disease and ulcerative colitis. For example abdominal pain and cramping in Crohn’s disease is more often in the right lower quadrant (RLQ) of the abdomen. With ulcerative colitis the pain is more commonly around the umbilicus (belly button) and left lower quadrant (LLQ) of the abdomen.
In addition, digestive symptoms like mouth sores, stomach inflammation and ulcers or even anal tears are more likely to be seen with Crohn’s disease than ulcerative colitis, since ulcerative colitis almost exclusively involves the colon and not other parts of the digestive tract. Complications like strictures (narrowing) and fistulas (abnormal channels) are more likely in Crohn’s disease.
Cancer Risk
Ulcerative colitis has been associated with an increased risk of colorectal cancer. This does not mean that every person with ulcerative colitis will develop colorectal cancer but the risk is greater. Previously, it was believed that this cancer risk was only with ulcerative colitis. However, studies have shown that Crohn’s disease also increases colorectal cancer.
This colorectal cancer risk is not specific to inflammatory bowel disease. Any type of chronic inflammation of the bowel can result in an increased cancer risk. It appears that the persistent inflammation may damage genetic material which is a major factor in any cancer development. Other risk factors such as family history of cancer and tobacco smoking also play a role.
Cure
There is no medical cure for either type of inflammatory bowel disease. This means that there are no drugs that will completely resolve inflammatory bowel disease so that it will not arise again. However, various drugs may be used in the treatment of inflammatory bowel disease to reduce inflammation, suppress or modulate the immune system.
Surgery also does no offer a cure in Crohn’s disease. Even if an affected portion of the digestive tract is removed in Crohn’s disease, another part of the tract may later be affected. However, surgery does offer a cure for ulcerative colitis. Removal of the colon (colectomy) means that there is no longer a target area for the inflammation to occur. The rectum may also be removed with the colon (proctocolectomy).
However, a colectomy is not without consequences but does offer a cure when other therapies fail to yield the desired results. Therefore a colectomy or proctocolectomy is only considered in severe cases of ulcerative colitis when the inflammation cannot be managed with drugs and the symptoms of ulcerative colitis are significantly affecting a person’s quality of life.