Drug-Induced Photosensitivity (Medication and Sun Sensitivity)
Drug-Induced Photosensitivity Definition
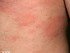
Drug-induced photosensitivity (light or sun sensitivity) is defined as skin inflammation caused by the combination of sunlight and certain medication. Drug-induced photosensitivity causes redness (erythema) and sunburn-like appearance of the skin. Both drug and light are required to cause drug-induced photosensitivity. It is the ‘photoactivation’ of the chemicals in the skin that causes the rash. The reaction between the light source and the photosensitizing chemical or medication can be divided into two types – phototoxic reaction and photoallergic reaction. Compared to photoallergic reactions, phototoxic reactions require larger amounts of the drug agent to cause sensitivity.
Drug-Induced Photosensitivity Types
Phototoxic reaction
In phototoxic reactions, exposure to sunlight activates the drug, which then damages the membranes or DNA of skin cells. Phototoxic reactions give the skin a sunburn-like appearance. These reactions have a rapid onset with the skin showing symptoms within minutes.
Ultraviolet A (UV-A) radiation present in sunlight is most commonly associated with phototoxic reactions. However, visible light and ultraviolet B (UV-B) radiations may also contribute to phototoxic reactions.
Usually only the sun-exposed areas of the skin develop rash from a phototoxic reaction. Once the medication causing the phototoxic reaction is discontinued and cleared from the body, the reaction also resolves. A re-exposure to light does not cause further episodes of phototoxic reactions.
Photoallergic reaction
In these reactions, UV radiation changes the structure of the drug, which is then recognized by the body’s immune system as a harmful invader (antigen). The immune system then launches an allergic response to fight the invader. This causes inflammation in the sun-exposed parts of the skin.
Photoallergic reactions give skin an eczema-like (reddish) appearance. These reactions are generally long-lasting (chronic) and symptoms appear within 1 to 3 days of exposure.
Many topical drugs can cause photoallergic reactions. These reactions may even recur upon sun exposure even when the medicines have been cleared from the system. Also, if the photoallergic reactions are severe or prolonged, they can sometimes affect the skin areas unexposed to the sun.
Drug-Induced Photosensitivity Incidence
Drug-induced photosensitivity reactions can affect persons of any age and race. Though phototoxic reactions are much more common than photoallergic reactions, the latter tends to affect men more often than women.
Drug-Induced Photosensitivity Pathophysiology
Many chemicals are sensitive to light. However, it is based on the duration of exposure to the light source, the intensity of the source and the type of light. In drug-induced photosensitivity, the exposure to light either :
- activates the chemical which then shows tissue toxicity and triggers inflammation, OR
- causes the chemical to breakdown or convert into compounds that triggers the body’s immune system and inflammation follows.
Th activation of the chemical is known as phototoxicity while the breakdown or conversion is referred to as photoallergy. A person does not necessarily have to have a predisposing sensitivity or allergy to experience this reaction. However, such individuals are more likely to experience drug-induced photosensitivity.
Drug-Induced Photosensitivity Symptoms
Phototoxic reaction symptoms includes :
- Burning and stinging of skin
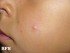
- Redness of sun-exposed areas of the skin (like the forehead, face, nose, arms, hands, and lips)
- Redness of sun-protected areas (in severe cases)
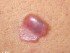
- Swelling or blisters (in severe cases
- Darkening of the skin (in severe cases)
Photoallergic reaction symptoms may not appear immediately or may be very mild during first exposure. The subsequent exposure, however, can cause a faster and more severe reaction. These symptoms include :
- Itching of the skin
- Redness
- Swollen patches on the exposed area or of the entire skin in that region
- Various different types of skin eruption
Drug-Induced Photosensitivity Complications
The most serious (though very rare) complication of drug-induced photosensitivity is death. Overdose of a particular group of drugs called psoralens can result in death in very few cases. However, photosensitivity can generate extreme reactions in some individuals, enough to limit their exposure to natural or even artificial light.
Drug-Induced Photosensitivity Causes
Drug-induced photosensitivity is a result of light reacting with chemicals that are derived from medication or topical application used by the person. Some drugs that can cause phototoxic reactions include the following:
- Various antibiotics like quinolones (ciprofloxacin, levofloxacin), tetracyclines (doxycycline), and sulfonamides (sulfamethoxazole, sulfamethoxazole, trimethoprim, cotrimoxazole)
- Malaria drugs (quinine, chloroquine, hydroxychloroquine)
- Antihistamines (diphenhydramine)
- Cancer chemotherapeutics (5-fluorouracil, dacarbazine, vinblastine, 5-aminolevulinic acid, methyl-5-aminolevulinic acid)
- Diabetic drugs (sulfonylureas, glyburide)
- Drugs for heart disease (amiodarone, nifedipine, quinidine, diltiazem)
- Diuretics (furosemide)
- Analgesics (painkillers)
- Non-steroidal anti-inflammatory drugs (naproxen, piroxicam)
- Psychiatric drugs (phenothiazines, tricyclic antidepressants like desipramine and imipramine)
- Skin and acne medications (isotretinoin, acitretin)
Drugs and chemicals that may be responsible for photoallergic reactions include :
- Sunscreens with para-aminobenzoic acid (PABA), oxybenzone, cyclohexanol, benzophenones, salicylates, cinnamate
- Antimicrobials (chlorhexidine, hexachlorophene, dapsone)
- Painkillers (celecoxib)
- Cancer chemotherapy drugs (5-fluorouracil)
- Fragrances like musk and fragrances with 6-methylcoumarine
Drug-Induced Photosensitivity Risk Factors
The susceptibility to these medications differs in different people. Some medical conditions that can increase sensitivity to sun exposure are:
- Systemic lupus erythematosus (SLE) causes a facial rash on the nose and cheeks, which can be very sensitive to sunlight.
- A hereditary condition called porphyria causes rashes and blisters upon exposure to sunlight.
- Vitiligo causes white, melanin-less patches in skin, which are very sensitive to UV light
- Inherited hypersensitivity disease called xeroderma pigmentosum, which increases the susceptibility of skin to cancer-causing effects of UV light.
- People suffering from oculocutaneous albinism have no melanin in the skin and eyes, which become highly sensitive to UV light.
Drug-Induced Photosensitivity Diagnosis
A detailed history of medication consumed, topical applications applied to the skin and the time spent in the sun helps in the diagnosis. Further tests that may be considered includes :
- Lab tests: Urine samples are checked for porphyrin levels to rule out similar conditions like porphyria cutanea tarda. Levels of antibodies like anti-nuclear antibody (ANA) and anti-Ro (SS-A) antibody are also checked.
- Photopatch test: To determine the causes of a photoallergic reaction, suspected photoallergens are applied to the back in 2 sets, one of which is removed after 24 hours and exposed to UV-A light. After 48 hours, both sets of patch tests are checked. If only UV-A exposed site shows redness, swelling and blisters, a photoallergic reaction is confirmed. If both sites show the same symptoms, it is a case of allergic contact dermatitis.
- Histological tests: In sudden phototoxic reactions, dead skin cells are seen. In some cases, swelling and blue-gray discoloration of the skin are also present.
Drug-Induced Photosensitivity Treatment
Treatment is aimed at identifying and discontinuing the medication that is causing photosensitivity. Using sunburn prevention methods like sunscreens and avoiding long exposure to sun are frequently advised. However, certain sunscreens may contain chemicals that are the main factor in these reactions. Applying wet dressings or cool compresses on skin eruptions may help relieve the symptoms.
- Steroids modify the body’s immune response. Topical steroid creams are given to decrease the redness. Oral steroids are recommended only in severe cases.
- Antihistamines help in decreasing the itching.
- Sunscreens lotions with avobenzone, zinc oxide, and titanium dioxide are recommended as they block UV-A rays effectively. Sunscreens are not recommended in people who are allergic to the constituents of sunscreens.
References :
http://emedicine.medscape.com/article/1049648-overview
http://dermnetnz.org/reactions/drug-photosensitivity.html
http://www.uch.edu/pdf/WISH_Drugs_and_Photosensitivity.pdf