Enteritis (Small Intestine Inflammation) Acute and Chronic
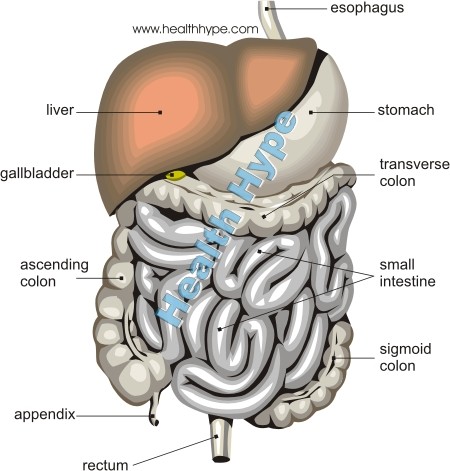
The small intestine, also referred to as the small bowel, extends from the stomach to the large intestine. It is the longest portion of the human alimentary tract and measures approximately 6 meters (20 feet). The small intestine is an important site of both digestion and absorption of nutrients. It has three parts – the duodenum leading from the stomach, jejunum and ileum which continues to the large intestine. As with any part of the alimentary tract, the small intestine may become inflamed through a number of mechanisms. When the small intestine alone is inflamed, it is then referred to as enteritis or it can be more specific like ileitis which is inflammation of the ileum of the small intestine.
What is enteritis?
Enteritis is the term for inflammation of the small intestine. It is not specific for which part of the small intestine that may be affected, either the duodenum, jejunum or ileum, or the entire small intestine. The term enteritis is not heard of frequently on its own. Instead it is associated with inflammation of the neighboring parts of the alimentary tract – gastroenteritis for inflammation of the stomach and small intestine or enterocolitis for inflammation of the small intestine and colon. However, this should not detract from the fact that inflammation of the small intestine can exist on its own and enteritis is as serious a pathology as gastritis (stomach inflammation only) and colitis (colon inflammation only).
The Small Intestine
The small intestine is longer but narrower than the stomach or colon. It communicates with several important structures of the digestive system, apart from the stomach and colon. The pancreas and gallbladder both empty its contents into the small intestine, specifically into the duodenum. While digestion and absorption begins in the mouth and intensifies in the stomach, majority of these processes occur in the small intestine.
Apart from the digestive enzymes that ‘rollover’ from the stomach, the pancreatic digestive enzymes and bile from the gallbladder, the small intestine also has its own enzymes that contribute to digestion. This originates from enterocytes in the mucosal epithelium lining the small intestine and includes lactase, sucrase, maltase and iso-maltase for carbohydrate digestion, peptidases for protein digestion and lipase for fat digestion. On a daily basis, the small intestine secretes some 2 liters of digestive enzymes, mucus and water.
However, its function of greatest importance is the absorption of most nutrients. The is facilitated by the massive surface area due to the mucosal protrusions known as microvilli and specialized structures within it for fat absorption (lacteals). When the small intestine is inflamed, it is the absorptive function that is severely impaired and largely responsible for the clinical presentation.
Swelling of the small intestine wall as a result of inflammation reduces the surface area and disrupts passive and active absorption of nutrients from the lumen. Water and electrolyte exchange between the tissue spaces and intestinal lumen is unregulated and large quantities of water and electrolytes are dumped into small intestine. In addition the epithelial cells may be destroyed and ulcers may form within the small intestine. Apart from the pathological changes to the intestinal wall, the microenvironment within the small intestine is also disturbed thereby allowing for the proliferation of pathogenic microorganisms.
Acute and Chronic Causes
Most cases of enteritis are caused by infections with bacteria being the leading pathogens. The more common of these include :
- Campylobacter jejuni
- Escherichia coli
- Salmonella spp
- Shigella spp
- Staphylococcus aureus
- Clostridium botulinum
It is important to note that these infectious agents may also involve the stomach and/or colon. Contaminated food and water accounts for the main routes of transmission. These pathogens are discussed further under gastroenteritis and infectious colitis. Infections tends to be acute with severe symptoms of sudden onset.
Small intestinal bacterial overgrowth (SIBO) may also lead to enteritis and here other underlying causes need to be taken into consideration. This is often subacute and can be chronic.
Radiation enteritis is inflammation of the small intestine due to radiation exposure. Almost all cases are due to radiation therapy in the treatment of cancer.
Autoimmune enteritis is due to a defective immune-mediated reaction that triggers inflammation without any obvious insult. Antibodies may develop against certain cell types in the lining of the small intestine and can be associated with conditions like Crohn’s disease (inflammatory bowel disease). Another link with inflammatory bowel disease is ‘backwash ileitis’ in ulcerative colitis. Eosinophilic gastroenteritis is an inherited condition that also involves the stomach. Autoimmune factors tend to lead to chronic enteritis.
Trauma, surgery and invasive investigative procedures may all contribute to inflammation although this is not specific for the small intestine. It will cause acute enteritis that can be life threatening when associated with hemorrhage.
Signs and Symptoms of Enteritis
- Severe diarrhea, which may be bloody at times.
- Abdominal pain and discomfort worse shortly after eating.
- Vomiting is uncommon but may be present if the duodenum and stomach are severely affected.
- Fever
- Loss of appetite
- Signs of nutrient deficiency (malabsorptio)
Overall the clinical presentation will depend on the extent of small intestine involvement. Considering its length, if only a small portion is affected then malabsorption may not be present or prominent. Excessive belching, burning pain similar to gastritis and change in symptoms very soon after eating may indicate that the inflammation is more prominent in the duodenum. Conversely, symptoms that tend to change with bowel movements, particularly with straining during defecation, may indicate more ileal involvement. However, diagnostic investigation is required to evaluate the areas that are affected.