Forehead Pain (Headache) – Causes, Symptoms and Treatment
Headaches remain one of the leading causes for doctor visits among adults across the globe. There pain can vary in nature, intensity and location. Sometimes the pain is diffuse and felt throughout the head. At other times the pain in a headache can be localized to one specific spot or region of the head. A forehead headache or forehead pain is one such case. It is among the more common locations for pain in a headache, along with the temples and back of the head.
The location of a headache can be significant in identifying the cause. However, the majority of headaches occur for no clearly identifiable reason and muscle strain is suspected to be the leading cause. It is important to know the medical terms associated with headaches at different locations.
- Front of the head or forehead = frontal headache
- Sides of the head or temples = temporal headache
- Back of the head = occipital headache
A headache on the top of the head would technically be referred to as a parietal headache although this term is not routinely used.
Frontal Headache
A frontal headache, forehead pain or headache at the front of the head may extend across the entire frontal region, be isolated to one side or localized to one spot. It may also be associated with a temporal headache. Frontal headaches may also extend downwards to the eyes, nose or also involve the entire face. As with most headaches, it is usually short-lived but may return thereafter. Less commonly, the headache may persist for days or weeks, partially easing for short periods, but otherwise persisting unabated.
It is always important to assess a frontal headache along with other symptoms. Many of the common causes of frontal headaches are not serious. However, the intensity of pain alone is not a good indicator of whether the underlying cause is serious or not. Accompanying symptoms may therefore prove useful in isolating a possible cause. Simple factors like wearing tight heats or head bands, certain hairstyles and not using corrective eye wear for vision problems may cause headaches that can be easily prevented.
Causes
Most of the same causes for a generalized headache may also be responsible for a frontal headache. Read more on headache causes. Some causes are more likely to result in a frontal headache than others. Here are four of the more common causes of a frontal headache.
Muscle Strain
Muscle strain is by far the leading cause of acute headaches. It is due to spasm or tightness of the muscles in the area and may also cause pain to radiate or be referred to other points. Headaches due to muscle strain are also known as tension-type headaches and the forehead is one of the common sites. It typically feels like a band across the head and tends to worsen during the day and ease after resting. The muscle strain is mainly caused by stress, tiredness, poor posture, frowning and sometimes dehydration.
Eyestrain
Overuse of the eyes has become a common problem in the past two decades in particular due to the hours spent on electronic devices. However, reading for long hours and exposure to bright light without protective eye wear may also quickly lead to eyestrain. This in turn can lead to eye pain and frontal headaches. Often the pain is also felt behind the eyes and there may also be some degree of forehead muscle strain as well. Other eye conditions like glaucoma and orbital cellulitis are also possible causes of pain at the front of the head.
Sinus Pain
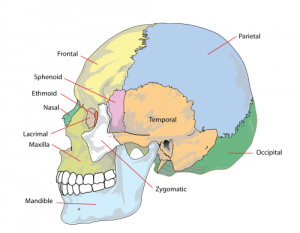
There are four pairs of hollow cavities within the skull bone known as the paranasal sinuses. It all connects with the nasal cavity. The location of the paranasal sinuses, particularly the frontal sinuses, can lead to forehead pain when the sinuses are inflamed, infected or congested. Sinusitis is a common condition and tends to cause a pressing type of pain in and around the sinuses. These types of headaches are often referred to as pressure headaches.
Migraine
Migraine headaches are another common cause of forehead pain. The exact cause of migraines is not known but it appears to be an interplay of genetic and environmental factors leading to changes in brain hormone levels. The pain tends to be worse on one side of the head although it can occur on both side. It is accompanied by visual disturbances, nausea, sometimes vomiting, dizziness and a range of neurological symptoms. The onset of the pain is typically preceded by an aura. Migraines are not usually a once off condition. It tends to recur frequently.
Symptoms
A headache is a symptom and not a disease. The nature of the pain, intensity and accompanying symptoms can vary from one episode to another. Sometimes the nature of the pain can provide clues to the possible cause. For example, a sinus headache may fee like pressure while muscle spasm may have a deep aching sensation. However, this is not always a reliable way of diagnosing the possible cause(s). The accompanying symptoms may instead be a better indicator.
- Eye redness, burning and tearing
- Blurred or double vision
- Nasal congestion
- Runny nose and sneezing
- Nasal tone to the voice
- Face pain, nose pain, cheek pain, jaw pain
- Nausea and sometimes vomiting
- Dizziness
Symptoms such as one-sided tingling or numbness, paralysis and loss of consciousness along with a headache may be due to a transient ischemic attack (TIA) or stroke. This means that the blood supply to the brain is compromised. Immediate medical attention is therefore necessary.
Treatment
The treatment of frontal headaches has to be directed at the underlying cause. Diagnostic investigations like a CT scan or MRI may be necessary to identify or exclude serious conditions. Conservative management which includes lifestyle changes, exercises and avoidance of causative/trigger factors is also important along with drug therapy.
Treatment for muscle strain and tension-type headaches include:
- Pain-relieving drugs
- Muscle relaxants
- Opiates
- Tricyclic antidepressants
- Anticonvulsants
Eyestrain usually does not require any specific drugs apart from pain-relieving medication for short periods of time. Lifestyle changes, protective eye wear and corrective lenses are usually sufficient to reduce the severity of eyestrain.
Treatment for sinusitis include:
- Nasal sprays – saline, decongestant, corticosteroid
- Oral decongestants or steroids
- Pain-relieving medication
- Antibiotics (for infections)
Treatment for migraines include:
- Painkillers (analgesics) and NSAIDs (non-steroidal anti-inflammatory drugs)
- Triptans
- Ergots
- Corticosteroids