Hyphema (Blood Inside Front of the Eye)
Hyphema Definition
Hyphema is a condition where there is a collection of blood inside the front of the eye (anterior chamber). The accumulation of the blood within the anterior chamber is usually visible. It occurs with injury to the eye, during or after surgery and in rare cases it may arise as a consequence of certain diseases. Depending on the extent of the bleeding, a hyphema may block the vision either partially or completely. The sight of blood in the front of the eye is often the most distressing symptom, along with the pain. However, the lack of visible blood does not mean that there is no bleeding as is the case with a microhyphema.
Hyphema Meaning
The inside of the eyeball has two chambers – the anterior chamber at the front of the eye and the posterior chamber behind it. The anterior chamber is smaller. It lies between the cornea and the iris and is filled with a fluid known as aqueous humor. The fluid in the anterior chamber is constantly circulated. New fluid is released and old fluid drains out. Since the anterior chamber lies in the front of the eyeball, most of it can be seen from the exterior. The clear aqueous humor that fills it allows us to see the iris and pupil through the anterior chamber.
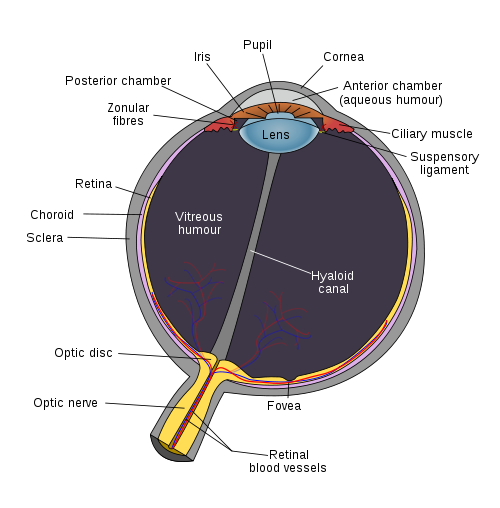 Picture of the internal structure of the eye from Wikimedia Commons
Picture of the internal structure of the eye from Wikimedia Commons
Location of the bleeding
The central parts of the inner eyeball do not contain blood vessels within it. Instead the structures around it and the walls of the eyeball are highly vascularized. Oxygen and nutrients are carried by the aqueous humor to nourish all the structures in the front of the eye which do not have blood vessels. When a blood vessel ruptures, the red blood cells leak into the aqueous humor and are carried to the front of the eye. The most common site of injury which leads to a hyphema is at the ciliary body. It is a triangular section at the front of the eye made up of the ciliary muscle and ciliary process. Bleeding usually occurs on the anterior (frontal) surface of the ciliary body to then cause a hyphema.
Reasons for bleeding
Injury to the eye can damage the inner tissues of the eyeball and its blood vessels. This can then lead to bleeding. However, not every injury and eye disease will lead to bleeding within the front of the eyeball. It is more likely to occur with blunt force where the impact causes the pressure within the eyeball (intra-ocular pressure) to suddenly rise. Other eye problems like glaucoma where the eye pressure also rises is unlikely to lead to bleeding as there is usually a gradual increase in the intra-ocular pressure in these cases. Surgical injury to the blood vessels within the eye may also lead to hyphema. Bleeding is sometimes not obvious and may only occur after the procedure.
Hyphema Causes
Most cases of hyphema are due to an injury (traumatic hyphema). However, hyphema associated with disease (spontaneous hyphema) may occur in a minority of cases and needs to be considered.
Traumatic Hyphema
- Blunt force injury to the eye
- Sharp penetrating eye injury
- Surgery – during, immediately after or a short while after the procedure
Spontaneous Hyphema
- Formation of new tiny blood vessels (microvasculature) which occurs with reduced oxygen supply to parts of the eye and conditions like diabetes mellitus.
- Eye tumors, especially cancers
- Eye infections like infectious uveitis
- Artificial lens implants
- Blood clotting disorders
- Blood vessel defects
Idiopathic Hyphema
In very rare cases, a hyphema may occur for no known reason. This is known as an idiopathic hyphema. These hyphemas often resolve on its own and may never occur again.
Hyphema Symptoms
Blood inside the eye
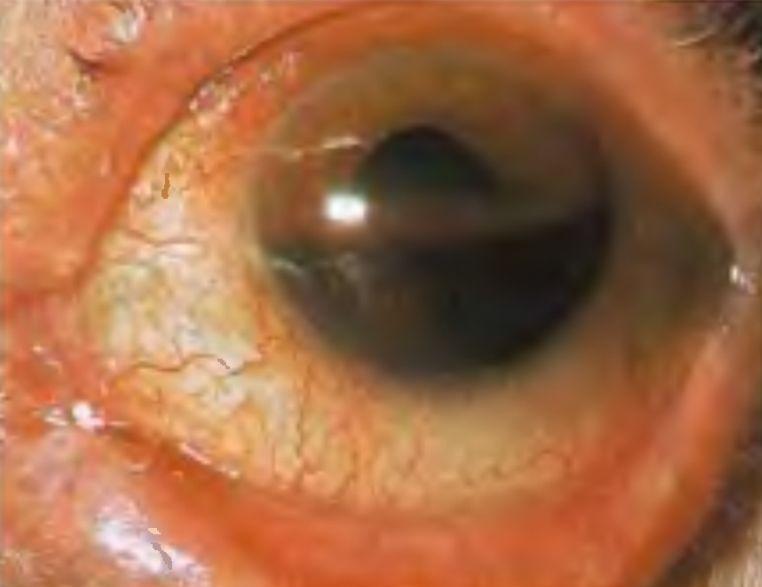
The most obvious sign of a hyphema is the accumulation of blood in the eye. In a microhyphema, there may not be any visible blood accumulation. The severity of the blood accumulation in traumatic hyphema is graded as follows.
- Grade 1 – Blood filling one-third (33%) of the anterior chamber.
- Grade 2 – Blood filling half (50%) of the anterior chamber.
- Grade 3 – Blood filling between half but just less than the total anterior chamber.
- Grade 4 – Total blood clotted giving the cornea a black appearance (blackball hyphema)
Picture of hyphema from Wikimedia Commons
Secondary bleeding
Sometimes the filling of blood in the anterior chamber stops for a few days an starts again. This may be a secondary hemorrhage. In severe cases, like grade 3 and 4 hyphema, the blood may become dark as it clots. Bright red blood may then be seen a few days afterwards around the edges of the clot. This is not necessarily a secondary hemorrhage but possibly a sign of the clot breaking down.
Eye pain and sensitivity
Hyphema is a painful condition. The presence of pain is one of the differentiating features from another condition with bleeding in the eye, known as a subconjunctival hemorrhage, which is painless. Light sensitivity is another typical symptom of hyphema which varies based on the severity of the condition.
Loss of vision
The disturbances in vision may vary to some degree. Patients may report :
- Blurred vision
- Cloudy vision
- Obstructed vision – partial or complete
Hyphema Diagnosis
The findings of a clinical examination, with visible accumulation of blood inside the anterior chamber, and a medical history are often sufficient for diagnosis. Examining the eye with a split lamp, testing the visual acuity and checking the intra-ocular pressure are the usual investigations that are undertaken. However, additional tests may be necessary in cases of a spontaneous or idiopathic hyphema where there is no evidence or history of trauma. These tests include :
- Sickle cell tests
- CT (computed tomography) scan
- Ocular ultrasound (B-scan)
- Iris fluorescein angiogram
- Gonioscopy
Hyphema Treatment
Mild cases of hyphema may resolve on its own with no treatment necessary. However, the course of treatment should be decided by a medical professional and preferably by an opthamalogist (eye specialist). A person with a hyphema should not avoid seeking medical attention in the hope that the condition will heal spontaneously. An untreated hyphema can lead to serious and permanent complications.
The following treatment measures may be necessary :
- A patch and protective shield over the injured eye only, although in the past both eyes were covered.
- Strict bed rest or at the very least minimal physical activity.
- Patients should lie with the head side slightly elevated by about 30 to 45 degrees to allow for drainage.
- Sedation may be considered in a patient who is extremely apprehensive or agitated.
- Anti-inflammatory drugs like acetaminophen to relieve the pain. Aspirin should not be used as it can worsen the bleeding.
- Topical medication may help with drainage but must only be used when or if prescribed by a medical doctor.
- Surgery for drainage of the blood is necessary if the intra-ocular pressure is rising to very high levels which may lead to glaucoma and cornea damage.
References :