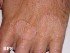
Itching and Rash Between Fingers Causes, Pictures, Treatments
While the skin on the hands is continuous with the rest of the body, it often does have to contend with greater environmental stresses as we touch a range of objects and substances throughout the day. Some can be an irritants, others can cause tissue damage and a few may also be allergens. Itchy fingers with or without a rash is not uncommon and at times may occur for short periods of time for no known reason. At other times it can be a persistent or recurrent problem that needs to be diagnosed and treated.
The area between the fingers (often referred to as the webs) is relatively delicate as it does not endure the same forces and frictions as does the other parts of the hand like the palms. These webs are skin folds that are present at joints to prevent the skin from excessively stretching during certain movements. However, it may also at times be more prone to skin irritation, damage and diseases due to its delicate nature. This may present with itching and a rash between the fingers (hand dermatitis).
Dry Skin
Dryness of the skin (xerosis) is one of the most common causes of skin itching with or without a rash anywhere on the body. However, it is often ignored as a possible cause. The hands have to weather a host of environmental factors that can easily cause the skin to rapidly dry. One of these factors is the use of antibacterial soaps or antiseptic hand sanitizers that have a tendency to dry the skin excessively as compared to other soaps and cleansers. Some people are more prone to dry skin than others due to occupational and even genetic factors.
Treatment
- Reduce the use of drying agents like antibacterial soap except when it is necessary.
- Hand sanitizers should be used in moderation.
- Moisturizers help to restore the moisture in dry skin.
- Barrier creams protect the skin from the environment and reduces drying.
Skin Irritation
Irritation of the skin arises when certain substances make contact with the skin and trigger inflammation often due to minor tissue damage. It gives rise to a rash known as contact dermatitis. When this rash occurs due to irritation and not an allergic reaction then it is known as irritant contact dermatitis. Some substances like chlorine will naturally irritate the skin even with brief exposure. Other substances like water or sweat is more likely to cause irritation with prolonged exposure.
One of the common types of irritant contact dermatitis of the hand is due to using soap or detergents. While this can affect anybody, even with domestic use, it is more likely to occur in people who wash items as an occupation, like the restaurant staff who are dish washers. It is therefore known as dishpan hands. It is not only the detergent that is a problem but also the repeated exposure of the skin to water. There are range of other domestic and industrial substances that can cause irritant contact dermatitis.
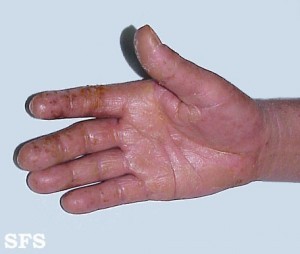
Treatment
- Remove the irritant by discontinuing making contact with the substance.
- Wash the hands thoroughly after contact with the irritant.
- Use protective gear like gloves to minimize contact between the skin and irritant.
- Corticosteroids can help reduce inflammation.
- Barrier applications protects the skin while it heals and can also block contact with the irritant to some extent.
Hand Allergies
An allergic skin reaction occurs when a person comes into contact with a substance that triggers the immune system. Inflammation is then initiated as a result of the immune activity. It only occurs in people who have a hypersensitivity to a harmless substance (allergen). Allergic contact dermatitis is where an allergic reaction is triggered at the site where an allergen makes contact with the skin. It is the other type of contact dermatitis from irritant contact dermatitis.
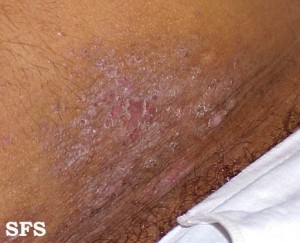
Another allergic condition where there may be a skin reaction on the hand is atopic dermatitis, also known commonly as eczema. It is more common among young children and often associated with conditions like asthma and allergic rhinitis. The allergen in atopic dermatitis can be inhaled and even ingested and not make contact with the skin as is the case with contact dermatitis. This includes foods like milk and wheat, or airborne substances like house dust mite. With atopic dermatitis, the skin folds are more often affected.
Treatment
- As with irritants, the contact with the allergens need to be minimized.
- Emollients to protect the skin while it heals.
- Antihistamines may be used to reduce the allergic reaction and ease symptoms.
- Corticosteroids (oral or topical) to reduce the inflammation and suppress the immune system.
Infections
Bacterial and fungal infections are the more common infections to involve the hand. Bacterial infections may affect the follicles (folliculitis), skin surface (erysipelas) and deeper under the skin (cellulitis). It is more likely to occur when there are breaks in the skin and particularly in people who have a weakened immune system. Under these circumstances even normal skin flora (bacteria that naturally live on the skin surface) may cause the infection.
Fungal infections are a common skin infection which is mainly due to dermatophytes, a type of fungus that has a predilection for human skin. The medical term for this infection is tinea manuum. As with the feet (jock itch / tinea pedis) the space between the digits are commonly infected as the fungus thrives in areas that are warm and moist, typically the skin folds. Sometimes yeasts can also be the cause of an infection but usually only at sites where the skin is eroded like with rubbing or chaffing (intertrigo).
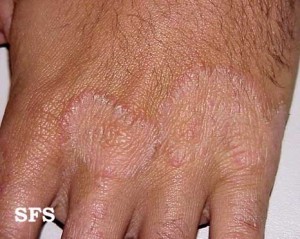
Treatments
- Keep the hands as dry as possible because fungi thrive in warm moist environments.
- Apply an antifungal topical agent to destroy the fungus and prevent recurrence.
- Oral antifungal agents (pills) are only usually necessary for severe infections that are not responding to topical treatment alone.
- Melaleuca alternifolia (tea tree oil) has been shown to be effective in treating skin fungi.
Other
- Scabies
- Drug hypersensitivity
- Neurodermatitis
- Pompholyx (dyshidrotic eczema)
- Psoriasis vulgaris
- Psoriatic arthritis
Last upated on September 3, 2018.