Mastoiditis (Back of the Skull Bone Infection)
What is mastoiditis?
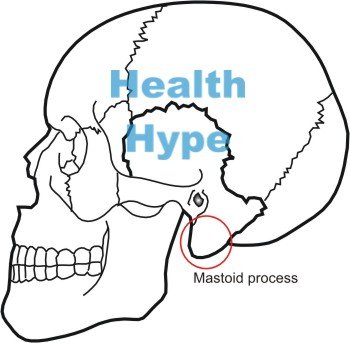
Mastoiditis is the inflammation of the bony protrusion of the skull just behind the ear canal. The mastoid process is a part of the temporal bone and has hollow air spaces known as the mastoid antrum and mastoid cells. In mastoiditis it is the mucosal membrane lining the mastoid antrum and mastoid cells system that becomes inflamed. Due to its close proximity to the ear, mastoiditis tends to arises as a complication of acute infections of the middle ear (otitis media). It is a potentially life threatening condition should the infection spread to the brain which lies near to the mastoid process.
Reasons for Mastoiditis
Mastoiditis occurs from the spread of infective organisms from the middle ear to the air cells in the mastoid process. The infection leads to pus formation within the narrow bony air spaces increasing the pressure in the air cells. The rate of pus production usually exceeds the rate of the pus drainage through the the eustachian tube and perforated eardrum. Swelling of the mucosal lining also hampers proper drainage of pus.
The impaired pus drainage increases the pus accumulation within the air spaces of mastoid antrum which can cause bone resorption and weakening of the bony walls of the mastoid air spaces. Over the course of time all the air spaces fuse to form single and irregular pus filled cavity. This pus may make its way to the subperiosteal space and it may eventually burst open through the skin to form pus discharging fistulous opening.
Causes of Mastoiditis
Since mastoiditis is usually a complication of a middle ear infection (otitis media), the causes are largely the same. Bacteria are the main pathogens that cause an infection but in some rare cases fungi may be involved. The following bacteria are more common :
- Streptococcus pneumonia (pneumococci), which accounts for about 25 to 30% of the infection, is the most common bacteria responsible for mastoiditis.
- Hemophilus influenza is responsible for about 20% of the infections.
- Moraxella catarrhalis accounts for some 10% of infections.
- Streptococcus pyogenes, staphylococci and Pseudomonas aeruginosa account for the remaining cases of mastoiditis.
- Pseudomonas, anaerobic bacteria (like peptostreptococcus) and mycobacterial species are often seen to be associated with chronic infections of the mastoid process.
- Aspergillus fumigatus is usually the fungus responsible for the rarely encountered fungal mastoiditis.
Mastoiditis is usually seen in infants and children who tend to be more prone to middle ear infections. although it can develop at any age. Other important risk factors include :
- Recurrent attacks of common cold, sinusitis, nasal infections, tonsillitis or other upper respiratory infections
- Acute infections like measles, whooping cough and diphtheria
- Malnutrition and poor hygiene
- Diabetes mellitus
- Nasal allergy
- Malformations of the palate mainly cleft palate
Mastoiditis symptoms
The patients usually present with :
- severe pain
- tenderness (painful to touch)
- erythema (redness)
- ear discharge
- swelling in the region of the mastoid bone
Some patients can also have pain in the ear and loss of hearing on the affected side. The other non-specific features accompanying mastoiditis can include fever, headache, irritability, loss of appetite and generalized weakness.
Mastoiditis diagnosis
The diagnosis is generally made on the basis of the medical history, the symptoms, the physical examination findings and the radiological findings.
The physical examination in acute mastoiditis can reveal red swollen mastoid process behind the ear on the affected side. The affected mastoid process is painful to touch (tender). A perforation of the tympanic membrane (ear drum) along with some amount of pus discharge in the external ear canal may be seen on examination of the ear.
The laboratory investigations can reveal rise in neutrophil count and ESR (erythrocyte sedimentation rate). X-ray of the mastoid area reveals cloudiness in the mastoid area due to the collection of pus and associated mucosal oedema. CT scan and MRI are better investigations compared to the X-ray in diagnosing mastoiditis. Pus then may be sent for culture and sensitivity to determine the proper antibiotic which can be used for the treatment.
Mastoiditis treatment
Antibiotics
Antibiotic therapy is the most important part of the conservative management of mastoiditis. Ideally patients should be started with an antibiotic based on culture and sensitivity report. However, any of the broad spectrum antibioticsc can be commenced until the culture and sensitivity report is available. The conservative management is often difficult in mastoiditis as drugs may not penetrate deep into the mastoid bone.
The antibiotic course often requires longer use beyond the regular duration of therapy. The common antibiotics used are ceftriaxone, amoxicillin with clavulanic acid, sparfloxacin, gatifloxacin, ofloxacin or linezolid. Anaerobic infections are treated with metronidazole. Ceftriaxone administered intravenously for 7 to 10 days is often the treatment of choice in acute mastoiditis. The initial intravenous therapy may be later switched to oral antibiotic therapy.
Alternative options of antibiotics includes :
- Fixed dose combination of amoxicillin and clavulanic acid containing 500mg of amoxicillin and 125mg of clavulanic acid administered 3 times daily for 5 to 10 days.
- Sparfloxacin or gatifloxacin 200 to 400mg administered once daily orally for about 7 days.
- Oflaxacin 200 to 400mg administered as tablets or injection twice daily for 5 to 10 days.
- Linezolid 600mg administered twice daily for about 10 to 20 days.
- Metronidazole 400 mg may be used thrice daily for 7 to 10 days to treat anaerobic infections.
Painkillers and anti-inflammatories
Analgesic anti-inflammatory drugs are generally given along with the antibiotic therapy to reduce the inflammation and relieve the pain. It will also help in reducing the temperature in those having the fever.