Multiple Sclerosis (MS) – Demyelinating Nerve Disease
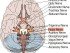
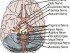
The myelin sheath covering the nerves fibers of the brain and spinal cord is composed of several layers of a fatty substance known as lipoprotein. In addition to acting as a protective covering for the nerves, the myelin sheath also allows rapid conduction of electrical impulses along the nerve fibers. When the myelin sheath is damaged, there may be a slow down of electrical impulses traveling along the nerves. The condition may be further exacerbated when the nerve fibers are also damaged.
Destruction of the myelin sheath is known as demyelination. Although the myelin sheath may be able to repair and regenerate itself in some cases, severe damage to it may cause the enclosed nerve to die. Since regeneration of nerve fibers in the brain and spinal cord is rarely possible, the nerve damage is usually permanent. Some disorders may affect the nerves of the central nervous system (brain and spinal cord) while others may affect the nerves in other parts of the body.
What is multiple sclerosis?
Multiple sclerosis (MS)is an autoimmune disease which is caused by inflammation and damage to the protective sheath that covers the nerves (myelin sheath). It is therefore also known as demyelinating disease. This damage and destruction slows down the impulses traveling along the nerves. As the disease progresses, the nerves itselfs may be damaged leading to problems such as loss of muscle control and difficulties with functions such as walking, talking, vision. The symptoms may occur intermittently, with periods of remission alternating with periods of relapse. Over time, there is usually gradual but relentless deterioration of the condition with worsening of symptoms. Multiple sclerosis is incurable (cannot be cured) but medication may relieve or control symptoms.
Primary demyelinating disorders are those conditions which cause demyelination in the central nervous system without any known cause. Multiple sclerosis is the most common type of primary demyelinating disorder, where there is usually patchy degeneration of the myelin sheath and enclosed nerve fibers in the eyes, brain, and spinal cord. The resultant multiple areas of scarring or sclerosis give rise to the term “multiple sclerosis”. The symptoms will vary according to whether the sensory or the motor nerves are involved.
Causes and Risk Factors
The exact cause of multiple sclerosis is not known but an autoimmune reaction is suspected to be the mechanism by which the myelin sheath is destroyed. Some of the possible risk factors may include :
- Exposure to a virus (such as herpes virus or retrovirus) in early life may trigger the autoimmune reaction.
- Sex – women are more likely to be affected than men.
- Age – the peak age of onset is in the 40s. Onset of MS before puberty or after the age of 60 is extremely rare.
- Genetic factor – people with certain genetic markers on the surface of their cells, known as human leukocyte antigens, may be more prone to developing MS.
- Family history – more common in first-degree relatives.
- Climate – more likely in people who have spent the first 15 years of their lives in a temperate climate than in those who have lived in a tropical climate. This may be related to vitamin D, which is formed when the skin is exposed to sunlight.
- Cigarette smoking.
- Having certain other autoimmune diseases – such as thyroiditis, type 1 diabetes, or inflammatory bowel disease – may increase the risk of developing MS.
Signs and Symptoms
There may be a wide and varied range of symptoms depending on the nerves involved. Patients usually go through periods of remission alternating with periods of relapse. The symptoms usually come on gradually over days or weeks, and resolve over weeks or months. Fever, hot baths, exposure to the sun, exercise, and stress may bring on or aggravate an attack. In some patients, the symptoms become progressively worsem and cause significant disability.
The signs and symptoms will depend upon the site of demyelination. A combination of spinal cord and brain-stem signs are common. Demyelination of the sensory nerves will give rise to sensory symptoms while that of the motor nerves will give rise to motor symptoms.
Patients with MS usually present with a single symptom, such as :
- Optic neuritis – pain on eye movement, with rapid deterioration of central vision. Visual changes may be the first symptom of MS.
- Tingling or numbness in the limbs.
- Leg weakness.
- Double vision (diplopia).
- Ataxia – lack of muscle coordination during voluntary movements, such as walking.
Presentation with more than one symptom is less common.
The other signs and symptoms of MS are :
- Sensory symptoms such as sensory dysesthesia or distorted sense of touch. A light touch may be perceives as painful, burning, pricking, or itching.
- Lhermitte’s sign is an electric shock-like sensation passing down the back to the legs in response to flexion of the neck. It is a common feature of MS but may be present in other conditions such as spondylosis.
- There may also be tingling, numbness, pins and needles sensation, and facial pain (trigeminal neuralgia).
- Motor symptoms may include muscle weakness, spasm, tremor, hyperreflexia (exaggeration of reflexes in response to normal stimuli), and trouble with coordination and balance.
- Difficulty in swallowing (dysphagia).
- Constipation.
- Visual disturbances.
- Hearing loss.
- Speech difficulties.
- Urinary problems like urgency or retention of urine.
- Erectile dysfunction.
- Fatigue is a common problem.
- Depression.
- Cognitive problems, such as impairment of memory, learning, planning, and judgment. However, significant intellectual impairment is usually rare until late stages of the disease.
Diagnosis of Multiple Sclerosis
Diagnosis of MS may be difficult since many of the symptoms are common to other nervous system disorders. The diagnosis will be based on the history and physical examination, including a neurological and eye examination. A diagnosis of MS should show lesions in more than one anatomical site at more than one time for which there is no other explanation. In other words, there should be 2 or more attacks with 2 or more clinical lesions.
There is no specific test for MS. The history and clinical features, along with test reports, may point to the diagnosis. It may be necessary to rule out other conditions that produce similar symptoms.
Tests may include :
- Lumbar puncture for cerebrospinal fluid (CSF) tests. Oligoclonal bands of IgG may be found in the CSF of about 70-90% of patients between attacks.
- MRI of the brain and spine.
- Nerve function study – evoked potential test.
Treatment of Multiple Sclerosis
MS cannot be cured. Treatment can only help to slow down the progression of the disease and help relieve symptoms as far as possible. Corticosteroids may be given to reduce the severity of attacks.
Drugs that may help to slow the progression of the disease are :
- Interferons, glatiramer acetate, and natalizumab.
- Fingolimod.
- Methotrexate, azathioprine, intravenous immunoglobulin (IVIg), and cyclophosphamide.
Drugs to control symptoms may include :
- Lioresal, tizanidine, or benzodiazepines to reduce muscle spasms.
- Cholinergics to reduce urinary symptoms.
- Antidepressants for mood or behavior symptoms.
- Amantadine for fatigue.
Physical and occupational therapy may help an MS patient cope with the disease.
Complications of Multiple Sclerosis
- Difficulty in walking and maintaining balance.
- Problems with swallowing.
- Problems with memory and thinking.
- Depression.
- Dementia.
- Mania.
- Problems in carrying out day to day activities.
- May need constant care.
- May need continuous catheterization for passing urine.
- More chance of urinary tract infections.
- Pressure sores.
- Osteoporosis.
- Paralysis, typically in the legs.
- Various side effects of drugs used for treatment.
Outlook or Prognosis
It is difficult to predict the outcome of MS. The disease may go through phases of remission and exacerbation. There may be long periods without any problems but the disease will almost always relapse. It may progressively worsenwith time. Although MS is not curable, a large number of patients continue to lead a relatively normal life without significant disability for 20 years or more. Initially the period in between attacks may be symptom free, with time there may be increasing loss of function. In the later stages, the patient may become wheelchair-bound and may need more support in carrying out day to day activities.
Poor outcome may be predicted in :
- Older male patients.
- Motor signs at onset of disease.
- Many relapses in early stage of the disease.
- Many MRI lesions.