Nephritis (Kidney Inflammation) Types, Symptoms, Complications
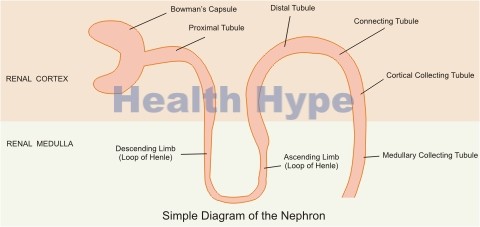
The kidneys are important filters for waste products in the bloodstream located on either side of the upper abdomen. The basic functional unit of the kidney is the nephron which receives filtered fluid from the blood at the glomerulus and the reabsorbs or secretes wastes, toxins, electrolytes and water along the course of its tubule. The end product is urine which is then passed into the renal pelvis and then drains into the ureter. From here it then empties into the bladder and is passed out through the urethra when the setting is appropriate. The functional processes of the kidney also regulate the blood pressure, blood volume and water-salt levels in the body.
What is nephritis?
Nephritis is the term for inflammation of the kidney, either one or both kidneys. If the kidney is inflamed, the functions of the kidney are disrupted to varying degrees depending on the type, cause and extent of inflammation. This disturbance is known as nephropathy. While the acute stages may cause only a temporary dysfunction, chronic inflammation and can permanently damage kidney tissue, lead to scarring within the kidney and even result in kidney failure. Both acute and chronic nephritis can be life-threatening if not treated and managed appropriately.
In order to understand the types of nephritis and its effects on the body, it is important have a basic knowledge of the structure of the kidney. The kidney is a bean-shaped organ which has blood vessels (renal artery and renal vein) that carry blood to it for filtration. The blood enters successively smaller vessels until it reaches the glomerular capillaries which are in close contact with the Bowman capsule of the glomerulus.
Fluid, electrolytes and waste products pass out of the capillary and into the capsule. Blood cells and proteins remain in the blood vessel. From here the fluid in the capsule passes along the tubules and is processed accordingly. The interstitial tissue is present throughout the kidney but it is the tissue surrounding the tubules that is of greater interest. It plays an important role in the exchange of water, electrolytes and toxins between the inside of the tubule (lumen).
Types of Nephritis
Nephritis can be classified in several ways but the most common approaches is by the part of the kidney or nephron that is inflamed or by the cause and/or underlying disease responsible for the inflammation.
- Glomerulonephritis is inflammation of the glomerulus of the nephron.
- Tubulointerstitial nephritis is inflammation of the tubule of the nephron and the surrounding interstitial tissue of the kidney. This is often referred to simply as interstitial nephritis.
- Pyelonephritis is inflammation of the kidney, usually the renal pelvis, and the urinary tract associated with a urinary tract infection (UTI).
All these types of nephritis can be either acute or chronic. When nephritis is classified according to the cause, for example lupus nephritis associated with systemic lupus erythematosus or infectious nephritis associated with an infection, the entire kidney is often affected. If left untreated and depending on the severity and duration of the inflammation, the entire kidney may be destroyed.
Glomerulonephritis
Glomerulonephritis is mainly due to immunologic disease. Immune activity is directed at the glomerulus, particularly the basement membrane, and causes localized inflammation. Read more on glomerulonephritis.
Other causes of glomerulonephritis includes :
- Infections – post-streptococcal, subacute bacterial endocarditis, viral infections, parasitic infections like malaria and less commonly fungal infections.
- Autoimmune diseases – systemic lupus erythematosus (SLE), Goodpasture’s syndrome, vasculitis (Wegener granulomatosis and polyarteritis nodosa), Henoch-Schönlein purpura.
- Immune-mediated hypersensitivity (atopy) particularly in children.
- Medication
- Diabetes mellitus
- Malignant hypertension (high blood pressure)
- Amyloidosis
- Genetic diseases
- Hodgkin’s lymphoma
Tubulointerstitial Nephritis
Tubulointerstitial nephritis is more commonly due to an infection, drug hypersensitivity, toxicity of drugs and other substances and autoimmune factors. Glomerulonephritis is usually absent or very mild. Tubulointerstitial nephritis, particularly acute forms, are at times related to pyelonephritis. Read more on tubulointerstitial nephritis.
Other causes of tubulointerstitial nephritis includes :
- Urinary tract obstruction – stones or tumors
- Atherosclerosis
- Amyloidosis
- Multiple myeloma
- Leukemia
- Metabolic diseases – hypercalcemia, hypokalemia, hyperoxaluria
- Genetic diseases
- Idiopathic – unknown causes
Pyelonephritis
Pyelonephritis is almost always due to infectious causes although underlying renal and systemic disease are frequently a predisposing factor particularly in the chronic form. Read more on pyelonephritis.
The most common cause of pyleonephritis is a bacterial infection, usually from an ascending urinary tract infection. E.coli accounts for about 90% of cases and is usually sourced locally from fecal matter (coliform bacteria). Viruses, fungi and parasites may also be responsible but are less commonly seen.
Risk factors associated with pyelonephritis includes :
- Urinary stones
- Prostate enlargement (benign prostatic hyperplasia)
- Urinary tract obstruction
- Pregnancy
- Sexually transmitted infections (STIs)
- Diabetes mellitus
- Immune deficiency
- Surgery to the urinary tract
- Urinary catheter
- Anatomical abnormalities of the kidney and/or urinary tract
Signs and Symptoms of Nephritis
The clinical presentation may vary among the different types of nephritis. However, it is characterized by urinary disturbances, changes in blood pressure and volume. Some of the common signs and symptoms includes :
- Polyuria – passing large volumes of urine in a day which presents as frequent urination.
- Hematuria – microscopic or gross appearance of blood in the urine.
- Nausea and/or vomiting
- Kidney pain
- Hypertension (high blood pressure) or hypotension (low blood pressure)
- Headaches
- Edema – swelling of the limbs, abdomen or the entire body.
Complications of Nephritis
Nephritis may eventually lead to renal failure and end-stage renal disease. This is life-threatening.
- Waste products like urea accumulate in the bloodstream (azotemia).
- Excess fluid in the body leads to high blood pressure, swelling, congestive heart failure and fluid in the lungs (pulmonary edema).
- Loss of electrolytes like sodium, chloride and potassium affects nerve and muscle function, which is dangerous when the normal heart function is affected.
- Decreased excretion of acids causes it to accumulate in the blood (metabolic acidosis) which causes neurological and muscular disturbances.
- Infections may spread throughout the body (septicemia) and lead to death.