Pancreatic Cancer Location, Types, Symptoms, Treatment, Survival
What is Pancreatic Cancer?
Pancreatic cancer is a malignant tumor that occurs in the pancreas. It is an important gland that regulates both digestive and metabolic functions in the body and these activities may be affected to varying degree with cancer. Although pancreatic cancer is not a common form of cancer and one of the leading causes of death due to cancer. Pancreatic cancer is usually detected late as it has very few early symptoms, and those that are present are usually non-specific in nature. Since this type of cancer spreads very rapidly, few treatment options are available by the time it is diagnosed. Surgery, radiation therapy, and chemotherapy are the usual forms of treatment available for pancreatic cancer, depending upon the stage at which the condition is diagnosed.
The Pancreatic Gland
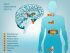
The pancreas lies transversely deep within the abdomen. It is situated behind the stomach, close to the duodenum (first part of the small intestine) and in front of the spine. The pancreas is approximately 15 centimeters (6 inches) long and is shaped like a hockey stick. It may be divided into 4 parts :
- The head of the pancreas is the broad end of the organ, on the right side of the abdomen, the portion that lies adjacent to the duodenum.
- The uncinate process is the extension of the head of the pancreas.
- The body is the mid-portion of the pancreas.
- The tail of the pancreas is the narrow portion of the organ, which lies in the extreme left of the abdomen, close to the spleen.
It is important to understand the different parts of the pancreas as it has significant implications on the location of the tumor. The pancreas is both an exocrine and endocrine gland and has different cells for these functions. The exocrine component secretes digestive enzymes that helps in the digestion of food. These enzymes reach the lumen of the small intestine by passing into the pancreatic duct which then joins with the common bile duct to form a common channel that opens into the small intestine through the ampulla of Vater. The endocrine part is ductless and secretes insulin and glucagon into the bloodstream which controls the blood glucose levels. The activity of the pancreas is discussed in further detail under pancreas function.
Location and Types of Pancreatic Cancers
Most tumors of the pancreas develop in the head of the pancreas. Cancers arising from the exocrine cells are much more common than endocrine cancers. Almost all exocrine cancers are adenocarcinomas. Endocrine cancers are very rare and are known as neuroendocrine tumors or islet cell tumors.
Majority of adenocarcinomas of the pancreas arise from the pancreatic duct. These usually involve nearby tissues and organs at an early stage and may metastasize or spread to the regional lymph nodes. Adenocarcinomas are usually detected late.
Ampullary or periampullary adenocarcinomas are rare tumors which arise from the ampulla of Vater or the adjacent duodenum. These tumors are less aggressive than adenocarcinomas.
A cystadenocarcinoma is extremely rare. It is a slow-growing tumor which usually arises from the head of the pancreas.
Causes and Risk Factors
The exact cause of pancreatic cancer is not known. The risk factors that may be associated with pancreatic cancer are :
- Age – risk of pancreatic cancer increases with age. Most cases develop in people over 60.
- Genetic factor – pancreatic cancer may occur due to inheriting an abnormal gene. About 95% have mutations in the KRAS2 gene.
- Diabetes mellitus.
- Cigarette smoking.
- Obesity.
- High fat diet.
- Chronic pancreatitis.
- Alcohol abuse, which is one of the main causes of chronic pancreatitis.
- Prolonged exposure to dyes, chemicals, and certain pesticides
Signs and Symptoms
There may be no symptoms in the early stages. Symptoms that are present are often non-specific and therefore ignored as of little consequence. The common signs and symptoms include :
- Nausea.
- Vomiting may be due to duodenal obstruction.
- Obstructive jaundice (yellowish discoloration of the skin, mucus membrane and eyes), with features such as pale stool, dark or yellow-colored urine, and generalized itching.
- Pain is usually a late feature. Painless jaundice that gradually becomes worse may be the first sign of pancreatic cancer.
- Upper abdominal pain which may penetrate to the back. The pain may be eased by sitting up and bending forwards.
- Diarrhea.
- Impaired digestion (maldigestion)
- Loss of appetite.
- Unintentional weight loss.
- Weakness.
- Fatigue.
- Depression.
- Venous thrombosis.
- Acute pancreatitis.
- Diabetes mellitus.
An abdominal mass may be felt either due to the tumor itself or an enlarged gallbladder. Jaundice with a palpable gallbladder, indicating biliary obstruction by pancreatic cancer, is known as Courvoisier’s sign. Metastasis tp the liver may also be felt on abdominal examination.
Diagnosis of Pancreatic Cancer
Diagnosis of pancreatic cancer is often late. Tests may include :
- CT scan of the abdomen.
- MRI of abdomen.
- Endoscopic retrograde cholangiopancreatography (ERCP).
- Endoscopic ultrasound.
- Pancreatic biopsy.
- Percutaneous transhepatic cholangiography (PTC).
- Complete blood count (CBC).
- Liver function tests.
- Serum bilirubin.
Staging of Pancreatic Cancer
Staging of pancreatic cancer is done to determine the extent and spread of the disease. This will help to guide the treatment options that are available. The stages of pancreatic cancer are :
- Stage 1 – cancer is confined to the pancreas.
- Stage 2 – cancer is no longer confined to the pancreas but has spread to nearby tissues and organs. Lymph nodes may also be involved.
- Stage 3 – cancer has spread to the major blood vessels around the pancreas. Lymph nodes are also involved.
- Stage 4 – cancer has metastasized or spread to distant organs and tissues such as the liver, lungs, and peritoneal lining.
Treatment of Pancreatic Cancer
The choice of treatment will depend upon the type, stage and location of cancer, age, and general health of the patient.
Surgery
Whipple procedure is the surgical procedure most commonly undertaken for early stage pancreatic cancer which is confined to the pancreas. It is also known pancreaticoduodenectomy. In this procedure, which is major surgery, the surgeon removes the head of the pancreas, the gallbladder, part of the bile duct, duodenum, and often a part of the stomach.
The other surgical procedures that may be undertaken are :
- Distal pancreatectomy involves removing the tail and body of the pancreas. Other structures such as the spleen, part of the stomach and intestine, left kidney, and left adrenal gland may also be removed.
- Total pancreatectomy is where the entire pancreas is removed. Other structures such as the gallbladder, bile duct, spleen, part of stomach and intestine, and surrounding lymph nodes may also be removed.
- Palliative surgery helps to ease symptoms such as obstructive jaundice. Bile duct obstruction may be treated with surgery and introduction of a biliary stent during ERCP.
Chemotherapy
In chemotherapy, anti-cancer drugs is administered to target and destroy the cancerous cells or to stop them from multiplying. Cancer that has spread to other organs such as the liver is best treated with chemotherapy alone. The drug commonly used is gemcitabine.
Radiation Therapy
Radiation therapy uses high-energy beams of radiation to shrink the tumor.
Combination Therapy
When the cancer is confined to the pancreas but is inoperable, a combination of radiation therapy and chemotherapy may be tried.
Adjuvant Therapy
Adjuvant therapy involves radiation and chemotherapy given after surgery.
Survival Rate of Pancreatic Cancer
Pancreatic cancer spreads rapidly and aggressively. As a result, the outlook is usually not very good since it is most often detected in the late stages, when effective treatment is not possible. Tumors developing in the head of the pancreas may be detected early since they are likely to block the bile duct and cause jaundice. Early detection and surgery to remove a small tumor increases chances of cure. In the late stages, palliative treatment can only help to cope with associated symptoms such as pain and obstructive jaundice, and will not cure the disease.
The average survival of pancreatic cancer is less than 6 months. The 5-year survival rate is less than 2%. After Whipple procedure, the 5-year survival rate may increase to 5% to14%.