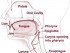
Perioral Dermatitis (Skin Rash around the Mouth)
Definition
Perioral dermatitis is a reddish skin rash around the mouth that presents with small pimples, tiny blisters and sometimes dry scaly skin. It closely resembles rosacea but is primarily isolated to the area around the mouth. The pimples are not due to acne vulgaris despite the similarity in presentation. Perioral dermatitis is a chronic skin condition that is mainly seen in women and sometimes in children. Although the cause of perioral dermatitis is unknown, it appears to be mainly linked to the use of topical corticosteroids. It does not usually affect the lips and rarely extends to the rest of the face. The inner part of the mouth is also not affected.
Incidence
Perioral dermatitis affects about 1% of the population and 9 out of 10 patients are women. The more commonly affected age group is within 20 to 45 years. Both the gender and age predilection may be due to the wider use of cosmetics in this group. However, there is an increasing incidence among men these days, possibly due to the more widely accepted use of skin care applications among males.
Pathophysiology
The mechanism behind perioral dermatitis is not well understood. It appears to be inflammatory in nature similar to rosacea and acne vulgaris but perioral dermatitis is a completely separate condition. Inflammation is the body’s response to tissue injury but can sometimes arise for other reasons when there is no injury. This causes an area to swell, become red, hot to touch and painful. It occurs due to the increased blood flow to an area, with increased permeability of the vessels and certain inflammatory chemicals that are concentrated at the specific site. The reason why this inflammation occurs in perioral dermatitis is unclear.
One proposed mechanism is that certain substances like topical corticosteroids and specific cosmetics may alter the structure of the skin. This may make the skin more sensitive to environmental factors. It is also believed that there may be an overgrowth of certain bacteria and fungi in the follicles. Whether these factors are the cause or trigger and exacerbating factors is not always obvious. Another proposed mechanism is that the inflammation may be neurogenic in origin meaning that certain nerve cells in the area release inflammatory chemicals locally.
Symptoms
Perioral dermatitis presents as a rash on the skin around the mouth. It is usually not itchy but many patients complain of tingling, burning or a taut sensation over the affected area. The rash presents as :
- Groups of red pimples or flat bumps. Some pimples are fluid-filled.
- Redness and swelling of the skin underneath and immediately around the pimples.
- Lesions are mainly isolated to the area around of the mouth but sometimes occurs on the side of nose, lower eyelids or even the forehead. Rarely similar lesions are noted on the back of the hands or vulva in young girls.
- Skin border immediately around the lips is usually clear.
- Skin lesions may appear on both sides (symmetrical) or be concentrated on one side (asymmetrical).
- Lumpy feeling of the affected skin.
- Sometimes dry and flaky skin on the affected site.
Depending on the severity and duration, patients with perioral dermatitis may suffer with emotional stress and depression. In severe cases there may be scarring and disfigurement which significantly heightens the psychosocial impact of perioral dermatitis.
Pictures
Pictures of perioral dermatitis sourced from Dermatology Atlas Brazil, courtesy of Samuel Freire da Silva, M.D.
Causes
The exact cause of perioral dermatitis is unknown. There are several factors that have been associated with the development of perioral dermatitis. This includes :
- Use of topical steroids.
- Cosmetics such as foundation make-up.
- Certain makeup removers.
- Skin care applications – various creams and ointments including sunscreen.
- Fluorinated toothpaste.
- Bacteria like Fusiform spirilla, and fungi like Candida yeasts.
- Environmental factors such as heat, UV light and wind tend to worsen pre-existing perioral dermatitis.
- Hormonal changes particularly in women like prior to menstruation.
- Oral contraceptives.
- Avoiding washing the skin with water.
Despite these known factors, the exact role it plays in perioral dermatitis is unclear. Some factors may be triggers while others tend to exacerbate the pre-existing condition.
Topical Steroids
The unrestricted use of topical steroids appears to be the main factor in perioral dermatitis. It is a global problem as people, particularly women, tend to use these creams and ointments for skin blemishes. Sometimes topical steroids accidentally makes contact with the skin on the face while being used for another skin condition elsewhere on the body. Long term or excessive use of topical steroids cause thinning of the skin and makes it susceptible to infections. These substances alter the skin structure in various ways thereby making it more sensitive to otherwise harmless environmental factors.
Sometimes over-the-counter (OTC) topical steroids are used to treat skin diseases other than perioral dermatitis. Patients may not seek medical advice and instead opt to treat the skin condition on their own with topical steroids. While it is very effective in clearing up most inflammatory skin diseases, the condition often returns as a rebound reaction after discontinuing the steroids. At times it is worse upon recurrence. Patients may then attempt to continue using topical steroids to treat the recurrence and it becomes a vicious cycle. Therefore perioral dermatitis in some cases may be a rebound effect of some underlying skin disease that was not properly diagnosed and treated earlier.
Diagnosis
Perioral dermatitis should be diagnosed by a dermatologist after a thorough examination of the skin. There are no specific tests that are useful in conclusively diagnosing the condition. However, various tests may of use to exclude other skin conditions that have a similar appearance. A skin biopsy sample examined under a microscope may appear similar to rosacea. However, it is important to note that perioral dermatitis is a separate condition from rosacea, acne vulgaris or seborrheic dermatitis.
Treatment
Perioral dermatitis is a chronic skin condition that can last for months to years if it is not treated. Attempting to mask the condition with topical steroids may offer temporary relief but should be avoided. Patients need to be made aware of the association with topical steroids and educated about misusing these skin applications.
Some of the treatments that have proven to be successful in the treatment of perioral dermatitis includes :
- Antibiotics such as doxycycline, erythromycin, metronidazole, minocycline and/or tetracycline.
- Pimecrolimus can be applied topically and is effective for the treatment of perioral dermatitis associated with topical steroid use.
- Isotretinoin which is used for the treatment of acne vulgaris may also be effective in treating perioral dermatitis.
- Benzoyl peroxide may be helpful but as a drying agent it can worsen the condition in some cases.
Prevention
Since the cause of perioral dermatitis is not fully understood, definitive preventative measures are not always clear. Some measures that may helpful includes :
- Avoiding the use of topical steroids unless it is prescribed for short term use by a doctor in order to treat a skin disease.
- Using sunscreens with a thinner viscosity – liquids or gels.
- Washing the face thoroughly without soap. Liquid cleansers can be used if necessary.
- Avoid make-up and skin care applications unless prescribed by a doctor.
- Individual trigger factors that can be identified should be avoided.
References :
emedicine.medscape.com/article/1071128-overview