Psoriatic Arthritis (Inflamed Joints with Psoriasis) Causes, Symptoms, Treatment
Arthritis is a well known joint condition where there is inflammation of the joint. There are many different types of arthritis with osteoarthritis being the most common form followed by rheumatoid arthritis. Psoriasis is a separate condition that involves the skin. It is an autoimmune skin condition that leads to thickened skin plaques among other changes. Sometimes these two conditions, arthritis and psoriasis, can occur together and this is known as psoriatic arthritis.
What is psoriatic arthritis?
Psoriatic arthritis is an autoimmune joint inflammation that occurs in people who have the skin disease known as psoriasis. It is a type of arthritis and should not be confused with other types of arthritis such as rheumatoid arthritis (RA), osteoarthritis (OA) or gouty arthritis. However, psoriatic arthritis (PsA) is due to an immune disturbance like rheumatoid arthritis and there are many similarities between PsA and RA.
Overall psoriatic arthritis is not as common as osteoarthritis (OA) or rheumatoid arthritis. It affects about 1% of the general population and around 11% of people who have psoriasis. Apart from the features of inflammation like swelling and pain in the joints, long term psoriatic arthritis that is poorly managed can also lead to joint damage and deformity. There is no cure for psoriatic arthritis and treament focuses on relieving the symptoms and preventing deformities.
Causes of Psoriatic Arthritis
The exact cause of psoriatic arthritis is unknown as is the case with the cause of psoriasis. Certain genetic factors may increase the likelihood of a person developing psoriasis and psoriatic arthritis as well as certain environmental triggers. An infection is one such trigger but it is important to understand that psoriatic arthritis and psoriasis are not infectious diseases.
The immune system is responsible for defending the body. However, in autoimmune disease like psoriasis and psoriatic arthritis, the immune system attacks the body’s healthy and normal tissue. With psoriasis, the immune system attacks the skin and causes an overproduction of skin cells without fast enough shedding of these cells. As a result the affected areas of the skin forms thick, dry and silvery-white plaques that are characteristic of psoriasis.
In the same way, the immune system may target the joints in psoriatic arthritis. There are changes in the joint similar to rheumatoid arthritis, like thickening of the joint lining (synovium). Certain immune cells also congregate within the lesions in the skin and joint and there are also higher levels of immune mediators (chemicals) within these lesions. All of these changes are indicators of increased immune activity and inflammation.
Signs and Symptoms
In most cases of psoriatic arthritis, it is psoriasis that arises before the arthritis. Sometimes the psoriasis can be present for decades before the arthritis component sets in. At other times the arthritis precedes the onset of psoriasis. In a minority of cases the psoriasis and arthritis arise at the same time. The skin lesions may not correlate with the joint symptoms in terms of location or severity.
Psoriatic arthritis can be of varying severity. The symptoms may be persistent or occur as occasional flare-ups. Most of the time the arthritis symptoms develop gradually but in some instances it can be sudden. Psoriatic arthritis symptoms closely resemble rheumatoid arthritis and it is not uncommon for psoriatic arthritis to sometimes be misdiagnosed as rheumatoid arthritis.
In psoriatic arthritis, anywhere from 2 to 5 or more joints are affected. Sometimes this may be the joints on both sides of the body (symmetrical), especially when many joints are affected. Otherwise when fewer joints are affected then only one side of the body is involved. The signs and symptoms of psoriatic arthritis is as follows:
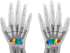
- Swollen joints, especially the joints of the fingers and toes. Psoriatic arthritis causes these joints to bulge thereby giving it a sausage-like appearance.
- Painful joints with or without obvious swelling. Usually the pain is worse when the joints are inactive like upon waking in the morning but also with overuse.
- Stiffness of the joints is prominent with inactivity, like waking up after a night’s sleep (morning stiffness). This stiffness eases as with movement of the joints.
- Deformities are more likely to occur with severe forms of psoriatic arthritis, particularly if it is left untreated or is poorly controlled and persists for a long period. It is referred to as arthritis mutilans or “pencil-in-cup” deformities.
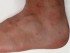
- Back and foot pain are also seen with psoriatic arthritis as the joints in these areas are inflamed. The joints of the feet, ankle, spine and between the spine and pelvis may also be painful, stiff and swollen.
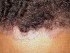
Apart from joint symptoms there may also be skin symptoms typical of psoriasis. This includes patches of thickened skin with a silvery-white appearance, that is dry and there is shedding of skin. The skin lesions are usually itchy.
Read more on psoriasis pictures.
There is no specific tests for psoriatic arthritis. Therefore a diagnosis of psoriatic arthritis depends on the presence of some or all of the symptoms mentioned above along with the findings of imaging studies such as x-rays, CT (computed tomography) scans and MRI (magnetic resonance imaging). The latter two investigations are useful in diagnosing psoriatic arthritis in the early stages.
Treatment of Psoriatic Arthritis
Always consult with a medical professional about the treatment options for psoriatic arthritis. Some of the drugs can have serious side effects but may not affect every person using these drugs.The treatment of psoriatic arthritis is not significantly different from rheumatoid arthritis or other forms of non-infectious arthritis. The focus of treatment is to reduce inflammation as well as managing and preventing flare-ups as far as possible. Drug therapy is the main approach although more invasive procedures may be considered for more severe cases.
- NSAIDs (non-steroidal anti-inflammatory drugs) to reduce inflammation and control symptoms.
- Immunosuppressants to suppress immune activity.
- DMARDS (disease-modifying anti-rheumatic drugs) to slow the progression of the disease.
- TNF-inhibitors to block inflammatory substances secreted by immune cells.
Read more on arthritis drugs.
In severe cases and particularly during acute flare-ups, corticosteroid injections in the affected joint may be considered. Oral (systemic) corticosteroids are not as often used these days. In these event of extensive joint damage, joint replacement surgery may become necessary.