Pyelonephritis (Kidney Infection) Causes, Signs and Symptoms
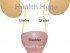
The kidneys are two bean-shaped organs lying on either side of the back of the upper abdomen. It is tucked under the ribcage. On a daily basis, the kidneys filter over 1.5 liters of blood and forms approximately 1 liter of urine containing waste products, water and electrolytes. This is then passed down the ureters into the hollow bladder which stores the urine. Once the bladder is almost full and the setting is appropriate, the urine is passed out through the urethra into the environment.
The kidney is a complex organ with three distinct layers known as the medulla, cortex and pelvis and its basic functional unit is the nephron. By filtering the blood at the head of the nephron (glomerulus) the fluid within the nephron is then processed as it passes through the remainder of the nephron (tubule). Excess water, electrolytes, toxins and metabolites are reabsorbed or secreted until the final product (urine) can be discarded. Along this process, the kidneys are also able to regulate the salt-water balance in the body, blood volume and the blood pressure.
What is pyelonephritis?
Pyelonephritis is the medical term for inflammation of the renal pelvis, tubules and interstitium most commonly associated with an infection. It is a serious complication of a urinary tract infection (UTI), typically extending from the infected bladder (cystitis) as a result of an ascending infection. A kidney infection may vary in severity but can be life-threatening and contribute to a host of other complications involving various systems other than the renal system. Although it can affect any age group and gender, pyelonephritis is more common in women who are generally prone to UTIs in comparison to men, given the shorter urethra.
Most urinary tract infections (UTIs) affect the lower tract – urethra, bladder and rarely the lower half of the ureters. Since UTIs are more frequently due to an ascending infection – pathogens gain entry to the urethra and travel higher up the tract – there is the risk of a kidney infection if treatment is poor or delayed or there are other underlying urinary tract disorders.
Typically an infection of the lower urinary tract, particularly of the urethra (urethritis) , is asymptomatic or causes very mild symptoms. Therefore treatment may be delayed. Treatment is usually sought early for a bladder infection (cystitis) due to the intensity of symptoms. However, the severity of the clinical presentation in pyelonephritis, which can vary, generally prompts a patient to immediately seek medical treatment. Failure to do so can permanently damage the kidney or even become life-threatening in a short period of time.
Causes of a Kidney Infection
Pyelonephrititis (kidney infection) can be acute or chronic. Both cases are most commonly due to a bacterial infection although viruses, fungi and rarely parasites may be responsible. In the majority of the cases, the bacteria originate from the person’s own fecal matter. It is more likely to occur in women due to a shorter urethra but personal hygiene is a significant contributing factor. The causative bacteria adhere to the urinary tract and its toxins causes localized inflammation. A kidney infection most commonly occurs when there is an obstruction within the urinary tract which prevents urine outflow to some degree.
Usually regular urination prevents an infection by the constant flushing of the urinary tract. Once the bacteria colonizes the distal urethra, it rapidly spreads up the urethra to eventually gain entry into the bladder. The vesicoureteral valve is designed to prevent backward flow of urine up into the ureter from the bladder. However, the inflammation associated with a bladder infection (cystitis) and other contributing factors allows for the backward flow (vesicoureteral reflux) which then introduces the bacteria into the ureters. From here, reflux may push urine n the ureter as high up as the renal pelvis (part of the kidney that communicates with the ureter) thereby allowing bacteria to invade the kidney.
Acute Pyelonephritis
Acute pyelonephritis is mainly due to bacterial invasion of the renal substance, and most commonly a result of E.coli (Escherichia coli) infection. As discussed, a kidney infection may arise as a complication of a UTI, therefore the modes of transmission and causative organisms are the same as the causes of a bladder infection. Less commonly, the causative organism may invade the kidney from surrounding organs or distant sites when it travels through the bloodstream (hematogenous spread).
Risk factors include :
- Urinary stones
- Prostate enlargement (benign prostatic hyperplasia)
- Urinary tract obstruction
- Pregnancy
- Sexually transmitted infections (STIs)
- Diabetes mellitus
- Immune deficiency
- Surgery to the urinary tract
- Urinary catheter
- Anatomical abnormalities of the kidney and/or urinary tract
Chronic Pyelonephritis
Chronic pyelonephritis is due to recurrent kidney infections or a persistent infection. The structural damage to the kidney in chronic pyelonephritis contributes to various other renal disorders like reflux nephropathy and even end-stage renal disease. The risk factors associated with chronic pyelonephritis may be the same as that of acute pyelonephritis and is more likely to occur in a person who is immunocompromised and/or with other urinary tract pathology.
Signs and Symptoms of a Kidney Infection
The signs and symptoms of pyelonephritis includes :
- Back pain and/or flank pain which may extend to the groin. Read more on kidney pain location.
- Urinary frequency – frequent urination
- Urinary tenesmus – constant urge to urinate
- Dysuria – pain, usually burning, when urinating
- Pyuria – pus in urine which presents as cloudy urine
- Hematuria – blood in the urine
- Fever
- Nausea and vomiting
The presentation may vary in acute and chronic pyelonephritis. The onset of signs and symptoms in acute pyelonephritis is usually sudden. Usually most, if not all, of the signs and symptoms mentioned above are present in acute pyelonephritis and are intense. It will rapidly ease and resolve within a few days if the appropriate antibiotic therapy is commenced as early as possible. Chronic pyelonephritis is generally more insidious in onset. In some cases it may remain silent for periods of time, or present with only a few clinical manifestations, until it is diagnosed by the presence of systemic disturbances. Since chronic pyelomephritis is more likely to occur in the presence of pre-existing kidney disease, this may mask the onset of the infection.