Skin Hypopigmentation and Hyperpigmentation Restore Treatment
The treatment of pigmentation disorders involves the management of hyperpigmentation and hypopigmentation skin disorders. Hyperpigmentation refers to the darkening of the skin due to increased production of the melanin which is the skin pigment synthesized by melanocytes. Hypopigmentation is lightening of the skin due to reduced production of the melanin.
Hyperpigmentation
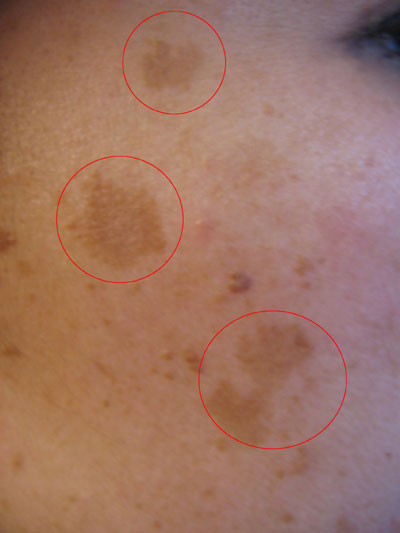
Hyperpigmentation of the skin may be seen in various local and systemic diseases. The causes for hyperpigmentation are chronic exposure to UV rays of the sun light, inflammatory conditions of the skin, and physical injuries like accidents and other forms of trauma. Common conditions associated with hyperpigmentation are :
- melasma (hyperpigmented patches on the forehead, nose, cheeks and chin occurring during pregnancy)
- Addison’s disease
- Cushing’s disease
- linea nigra (straight line of hyperpigmentation extending from the umbilicus till the lower abdomen occurring in pregnancy)
- acanthosis nigricans (hyperpigmented patches seen in conditions associated with insulin resistance)
- acne especially with scarring
- fungal infections – chronic fungal skin infections particularly with long term scratching or infections like tinea nigra marked by darkening
- smoker’s melanosis
- hemochromatosis (elevated serum iron levels with secondary deposition of the iron in skin and other organs)
- mercury poisoning.
Hypopigmentation
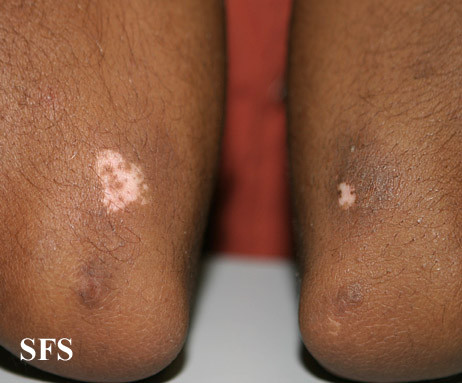
Hypopigmentation can result from various local and systemic causes. The extent of hypopigmentation may vary from partial hypopigmentation as in case of skin injury to complete hypopigmentation as seen in vitiligo. Hypopigmentation is usually a temporary manifestation of some disease process except for conditions like the albinism.
Common causes for hypopigmentation of skin are :
- fungal infections of the skin like Pityriasis alba (usually seen in the infants and the school going children, which presents as dry, scaly and hypopigmented coin-like skin lesions)
- leprosy
- burns
- trauma
- vitiligo
- albinism
Some conditions of hypopigmentation resolve when the underlying cause is identified and treated accordingly while there is no cure for conditions like the albinism as it is a genetic condition.
- Albinism is an inherited genetic disorder characterized by complete absence of the melanin production. The eyes, hair and skin of these patients typically do not have any melanin pigmentation. There is no cure for this condition. These patients are at risk of developing skin cancers and they should be advised to protect themselves by using good sun screens regularly.
- Vitiligo is a condition associated with immune mediated destruction of the melanocytes due to oxidative stress, neurological and viral diseases. The disease usually begins with small hypopigmented patches and the size of the patches increase slowly with time. Usually these hypopigmented lesions appear near extremities, face, and wrists.
Hyperpigmentation Treatment
The management of hyperpigmentation lies in correcting the underlying cause. However symptomatic improvement can be obtained in conditions like melasma by using hypopigmenting (demelanizing) agents.
Hydroquinone
- Hydroquinone reduces the melanin formation by inhibiting the enzymes (mainly tyrosinase) involved in its synthesis. It is a weak hypopigmenting agent.
- Hydroquinone has to be used regularly as 2 to 6% cream or lotion for several months to get the benefit from the treatment.
- The beneficial effects are more significant when used along with sunscreens.
- It is particularly effective to reduce the pigmentation in melasma.
- The chances for recurrence of the hyperpigmentation following the discontinuation of hydroquinone are high, especially on exposure to the sunlight.
- Hydroquinone is an irritant, and some of the patients might develop allergy and rash.
- Proper precautions have to be taken while applying hydroquinone so that it does not enter the eyes.
Monobenzone
- Monobenzone is derived from hydroquinone and is a stronger hypopigmenting agent than hydroquinone.
- It may even destroy the melanocytes and might lead to the development of permanent hypopigmented skin.
- Full therapeutic effect appears after applying a 5 to 20% lotion or ointment it 2 to 3 times daily for 4 to 6 months .
- The hypopigmenting action of monobenzone is not uniform and hence the patient might be left with cosmetically unacceptable hypopigmented patches.
- It can cause dermatological side effects like redness and itching.
- The use of monobenzone is mainly restricted to the treatment of melasma due to inflammation and also in patients with extensive vitiligo to cause hypopigmentation of the normal skin to make the color uniform.
Azelaic acid
- Azelaic acid is effective to treat hyperpigmentation due to acne and melasma.
- It decreases the melanin formation by inhibiting the enzyme tyrosinase.
- It is a weak hypopigmenting agent and does not produce permanent hypopigmentation.
- Azelaic acid is available as a 10 to 20% cream meant for once or twice daily application.
- Adverse effects with the use of azelaic acid are transient and often limited to local irritation.
Other agents
A few other substances which might be helpful in lowering the skin pigmentation are licorice and vitamin C (ascorbic acid). The beneficial effects are not yet proved to be significant like the agents discussed earlier but may have some useful contributory effects.
Hypopigmentation Treatment
The root cause of the condition leading to hypopigmentation needs to be treated in order for the skin color to restore. Albinism cannot be effectively treated with these therapies. However, it is effective for conditions like melanocyte where the primary disease process is destruction of melanin producing cells. Nevertheless, the treatment of vitiligo is often difficult and the response to treatment is often unpredictable.
The most common treatment approach adopted is phototherapy, usually in combination with topical photosensitizers or immunosuppressants. Other treatment options include immunosuppressant creams, topical steroids and melanocyte transplantation. Skin camouflage techniques may be used for temporary cosmetic benefits.
Immunomodulators
- Tacrolimus and pimecrolimus are immune suppressant drugs which are known to possess additional anti-inflammatory action. These drugs are helpful topically in the treatment of vitiligo and are used off-label for vitiligo treatment.
- Combining phototherapy with these drugs is believed to produce a faster response. This is particularly useful approach in treating vitiligo in the children.
- The use of immunomodulators is associated with an increased risk of skin infections and development of skin cancers when used for long term.
Topical steroids
Topical corticosteroids like fluticasone (0.05%) and triamcinolone (0.05%) are helpful in treatment of vitiligo, but prolonged use is associated with thinning of skin, easy bruising of the skin and increased risk of skin infections.
Melanocyte transplantation
- Transplantation of melanocyte is another possible approach in the treatment of vitiligo.
- The procedure involves extraction of melanocytes from the normal skin of the affected individual (usually from the gluteal region) and grafting of these melanocytes into the areas affected by vitiligo.
- A significant percentage of the patients respond with significant re-pigmentation with this procedure but the duration of the re-pigmentation is highly variable from one patient to another.
Phototherapy
UVB therapy
- The exposure of the skin to UV-B rays from special UVB lamps may be of help in restoring the skin pigmentation in some individuals.
- Vitiligo of the face and neck (of less than 3 years of duration) shows signs of response to the UVB exposure in about 3 to 4 weeks.
- UVB treatment may take several months in cases of vitiligo of the legs and the hand, especially those which are more than 3 years of duration.
- Photo sensitizers like methoxsalen 0.4 to 0.6mg/kg taken orally one hour before the phototherapy is known to improve the response of UVB rays.
PUVA therapy
- PUVA therapy is ultraviolet A therapy in combination with photosensitizers like psoralen. Methoxypsoralen (methoxsalen) is the commonly used psoralen in the PUVA therapy.
- Methoxsalen is used in the dose of 0.4 to 0.6mg/kg orally one hour before exposing the patient to UV-A rays of sunlight or artificial UV-A sources. The time of exposure should be gradually increased with each session.
- The patient may expose the affected part to UV-A rays for 15 minutes initially and then gradually the time may be increased up to 30 minutes.
- The psoralen therapy with such exposure sessions should be repeated every alternate day for several months to years till the pigmentation is regained satisfactorily.
- The main adverse effect of PUVA therapy is redness and itching on the sun exposed areas. Other side effects include vesicle and bullae formation, rash, folliculitis, gastrointestinal disturbances, and skin tenderness. PUVA therapy has higher chances of causing skin injury and freckling compared to UVB therapy. Prolonged exposure to the ultraviolet rays can potentially increase the risk of developing skin cancers.
- PUVA therapy is contraindicated in patients with disease conditions associated photosensitivity like porphyrea, xeroderma pigmentosum, lupus erythematosus and so on. It is also contraindicated in individuals with skin cancers like melanoma or having history of melanoma. Patients should use protective sunglasses during daylight while on PUVA therapy to prevent injury to the eyes.
- Topical application of methoxsalen 1% solution on the affected sites may be used instead of oral methoxsalen. The sun exposure should be limited to one minute when the topical methoxsalen is used. After the therapeutic exposure, further exposure to the sunlight should be avoided. Adequate covering with occlusive bandage or sun screen protection should be taken before going into sunlight under unavoidable circumstances. The treatment should be repeated every week with gradual increase in the duration of sun exposure. Observable pigmentation starts in about a few weeks time while full therapeutic effect might be seen only after several months.