Types of Cervical Cancer, Causes and Risk Factors
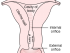
There are two types of cells lining the cervix :
- squamous cells lining the exocervix, and
- columnar cells lining the endocervix
Most cervical cancers arise at the squamocolumnar junction. This is the area where the two cell types meet.
Types of Cervical Cancer
There are two main types of cervical cancer, depending upon the cellular structure as seen under the microscope.
Squamous Cell Carcinoma (SCC)
Almost 80% to 90% of cervical cancers belong to this group. It usually arises at the squamocolumnar junction and is made up of squamous cells. SCC may be further subdivided into
- Well differentiated SCC
- Moderately differentiated SCC
- Undifferentiated SCC
The outlook worsens progressively from the well differentiated type of SCC to the undifferentiated variety.
Adenocarcinoma
Almost all other cervical cancers that do not belong to the SCC group are adenocarcinomas. These arise in the endocervix, which is lined by columnar cells. It accounts for about 5% to 20% of cervical cancers.
The subtypes include :
- Well differentiated mucinous adenocarcinoma
- Papillary adenocarcinoma
- Clear cell adenocarcinoma
Other
The other, less common, types of cervical cancer are :
- Mixed carcinoma or adenosquamous carcinoma
- Variants of SCC and adenocarcinoma.
- Sarcoma
- Lymphoma
- Melanoma
- Metastatic tumors – metastasis is commonly from endometrial malignancies (uterine cancer), but may also come from ovarian, breast, and colon cancer.
Causes and Risk Factors of Cervical Cancer
Cancer of the cervix is usually preceded by a pre-cancerous stage, which may be present for a variable period of time. In most cases it progresses very slowly over years, but in some cases it may develop quite rapidly. If detected and treated early, at the pre-cancerous stage, it may be possible to prevent the development of invasive cervical cancer.
The incidence of cervical cancer has diminished in developed countries, possibly due to effective screening and diagnosis at the pre-cancerous stage. Lack of such screening programs in the developing countries may be the reason for the high incidence of cervical cancer that continues in these countries.
- Infection with human papillomavirus (HPV), which is transmitted by sexual intercourse, can be considered as the most important factor leading to development of cervical cancer, although not all cervical cancers are associated with HPV. Similarly, not all women infected with HPV will develop cervical cancer. Certain strains of HPV have been linked with a increased risk of cancer of the cervix. However, vaccination against HPV can help to protect against cervical cancer to a certain extent.
The other risk factors associated with cervical cancer include :
- Cervical cancer may occur at any age, but pre-cancerous lesions are detected more frequently in women between the ages of 25 and 34. Invasive carcinoma is more likely to be seen in middle aged or older women.
- Women having multiple sexual partners, and those women who have been sexually active from an early age may be at a greater risk possibly due to an increased chance of contracting HPV infection. Male partners having multiple sexual partners may compound the risk for the same reason.
- Multiple childbirths seem to increase the risk, especially in women with HPV infection.
- Race seems to be a factor as well as African-American and Hispanic women are at considerably higher risk than Caucasian women.
- Low socioeconomic status may also be considered as a risk factor but this could probably be attributed to a lack of awareness about the disease, and limited accessibility to health care services for routine screening.
- Smoking may double the risk compared women who do not smoke.
- Impaired immune functioning such as women suffering from HIV/AIDS or those on immunosuppressive drugs.
- Long term use of combined oral contraceptive pills, particularly if used for more than 5 years, may be a risk factor. The risk may be the same as woman who does not use oral contraceptives after stopping the pill for 10 years.
- Daughters of women who took the drug diethylstilbestrol (DES) prescribed to prevent miscarriage during pregnancy appear to be at a greater risk.
- Genetic predisposition – women with first degree relatives (mother or sister) may be more at risk.
- A history of dysplasia or pre-cancerous lesions of the cervix, vagina, or vulva.
- Sexually transmitted diseases, such as chlamydia.