Oral Leukoplakia (White Patches Inside the Mouth)
Some disorders of the skin and inner lining of cavities like the mouth seem like harmless abnormalities that do not warrant much medical attention. Apart from moderate discomfort, it does not appear to cause any damage to tissue or affect functioning. Oral leukoplakia is one such condition. However, it needs to be carefully monitored as it has the potential to become malignant (cancerous).
There are a number of different types of tongue coating and the most common is usually not a cause for any concern. It is a result of food particles, bacteria and saliva accumulating between the papillae of the tongue but can be easily removed with proper brushing. However, sometimes white coatings in the mouth may be a disease that cannot be removed and requires medical treatment.
What is oral leukoplakia?
Oral leukoplakia are white patches or plaques that appear on the inside of the mouth (oral mucosa). It cannot be rubbed or scraped off and may be precancerous (early signs of cancer) or potentially cancerous. However, most of the time these lesions are benign (non-cancerous) and therefore not serious. The exact cause of leukoplakia is unknown but is closely associated with tobacco use. Another similar condition known as hairy leukoplakia is associated with EBV (Epstein-Barr virus) infection.
Oral Leukoplakia (OL) describes the appearance of white or gray patches on the in the mouth cavity – on the inner cheek, tongue and gums. Typical leukoplakia plaques may appear inside mouth that do not get scraped off easily. The cause of oral leukoplakia remains unclear but it seems like to persistent irritation of the tissue of the mouth.
Although harmless, oral leukoplakoa patches have a high risk of becoming malignant (cancerous). It is therefore considered as a pre-malignant clinical sign. Another form that appears as fuzzy, hairy patches called hairy leukoplakia appear during severe viral infections like HIV. Oral leukoplakia affects 1% of the population, mainly people above 40 years, and the elderly in particular.
It affects less than 1 out 100 people and is more common among men than women. Oral leukoplakia mainly occurs after the age of 40 years. The risk of oral leukoplakia lesions being pre-cancerous ranges from 0.6% to 20% based on the results of various studies. It can be removed by physical scraping with a scalpel, laser or freezing if stopping tobacco does not lead to resolution of the lesions.
What Happens in Oral Leukoplakia?
The inner lining of the mouth is known as the oral mucosa. It covers the gums, inner cheeks, inner lips, roof of the mouth (palate), tongue and under the tongue. The mucosa is continuous with the throat. In oral leukoplakia, the affected parts of the oral mucosa are abnormally thickened. When the epithelial cells of the oral mucosa appear abnormal in shape, size and other characteristics as would be expected then it may be indicative of a pre-cancerous lesion.
The exact cause of oral leukoplakia is unknown. It is associated with tobacco use, both chewed and smoked, and is usually seen in long term tobacco use. It is believed that this link may be due to chronic irritation of the mucosa by tobacco and tobacco smoke. However, tobacco is not the only link that has been observed. Habitual alcohol use, poorly fitting dentures, oral candidiasis, glossitis (tongue inflammation) due to syphilis and certain vitamin deficiencies may also be associated with oral leukoplakia.
Inner lining of the mouth
The soft thin tissue that covers the mouth cavity is called the oral mucosa. It protects the underlying tissues like muscles, fats, nerves and blood vessels from mechanical injury. It is thin and almost transparent and has a red color due to the blood flow in the superficial blood vessels just underneath it. Although mucus glands secrete small amount of mucus, the oral mucosal membrane is largely kept moist by saliva secreted from the major salivary glands.
Injury to the oral mucosa
Injury of any form causes tissue become inflamed which is then followed by healing and tissue regeneration. Although the cause of oral leukoplakia is unknown, it appears to be linked to ongoing injury. Persistent irritation of the mouth mucosal membrane usually elicits development of oral leukoplakia lesions. Often diagnosed in the tobacco users, it appears that tobacco and the range of chemicals within it act as a major irritant to the moral mucosa. Certain infectious diseases like AIDS also present unusual, fuzzy or hairy lesions known as hairy leukoplakia. Hairy leukoplakia is often indicates a weak immune system and is among the first signs of viral infections including HIV. Although harmless initially, oral leukoplakia patches may become malignant and develop into oral cancers.
Skin protein clumps
Keratin deposition or keratinization usually marks the maturity of epidermal skin cells that makes it strong and resistant to injury. Mucosal lining of the mouth, unlike skin cells, is soft and contains relatively less keratin. Oral epithelium is frequently subjected to mechanical injuries including chewing and denture fittings. Rapid turnover rates and regenerative abilities compensate for the absence of keratinization. Excessive keratin deposition in mouth epithelium often appears as white plaque, a characteristic feature of typical oral leukoplakia patch which is markedly different from the surrounding red oral mucosa.
Oral Leukoplakia Causes
The causes of oral leukoplakia remain unclear. However, certain events are linked to its appearance :
- Excessive and prolonged use of tobacco (smoking or chewing).
- Abrasions from rough teeth or ill-fitting dentures, fillings or crown and chewing areca nut and betel leaf.
- Viral infections like HIV or AIDS.
- Deficiency of vitamins – A, B12, C and folic acid in the blood.
- Endocrine disturbances
- Exposure to sun
Although tobacco is considered to be the major contributor of oral leukoplakia, none of its individual biochemical components have been isolated as the sole irritant that could cause these lesions. Men are at twice the risk of developing oral leukoplakia as compared to females.
Oral leukoplakia patches resemble thrush that appears commonly in the mouth of patients suffering from diabetes, HIV or cancer due to accumulation of fungus (candida). Thrush, like hairy leukoplakia, indicates a weak immune system optimum for harboring viral infections. Unlike oral leukoplakia lesions, thrush presents creamy, painful patches that bleed upon scraping.
Most oral leukoplakia lesions are of unknown origin (idiopathic). Idiopathic oral leukoplakia patches are considered as precursors of oral cancers (pre-malignant lesion) and warrant a regular check up (biopsy) every 2 to 3 months. Excessive tobacco and alcohol consumption are important risk factors related to transformation of oral leukoplakia into malignant cancers. Oral leukoplakia contributes to 20% of the total oral cancers detected.
Oral Leukoplakia Symptoms
Oral leukoplakia appears as white to gray patches or plaques that are irregularly shaped and are either flat or slightly raised. Some lesions may be thick and hard. There is usually no pain or any other symptoms and smaller patches may often go unnoticed. Many people may try to brush or scrape it off on their own but to no avail. Sometime these lesions may also be accompanied by redness of the underlying and surrounding oral mucosa.
The development of oral leukoplakia patches is progressive starting from small, translucent patch to prominent, slightly raised, opaque white plaque with granular texture.
Usually without symptoms, oral leukoplakia manifests itself as:
- White or gray sores in the cheek wall, floor and roof of the mouth or on tongue, gums and lips.
- Thick, slightly raised, hardened mass of skin cells having rough texture that could not be scraped off.
Hairy Leukoplakia
A variation of oral leukoplakia is hairy leukoplakia. It manifests itself as hairy or fuzzy skin patches in the mouth. Usually hairy leukoplakia patches appear during viral infections like HIV/AIDS.
Erythroplakia
Instead of white or gray patches, rarely red sores (erythroplakia) appear. Erythroplakia patches have abnormalities in maturation of epidermal cells (dysplasia). The absence of outer epithelial lining, reveal the underlying blood vessels making these lesions appear red-colored. They are highly potent of becoming cancerous.
Location
Although oral leukoplakia can occur anywhere on the oral mucosa, the most commonly affected sites are:
- Under the tongue
- Side of the tongue
- Floor of the mouth
- Soft palate
- Gums
- Lower lip
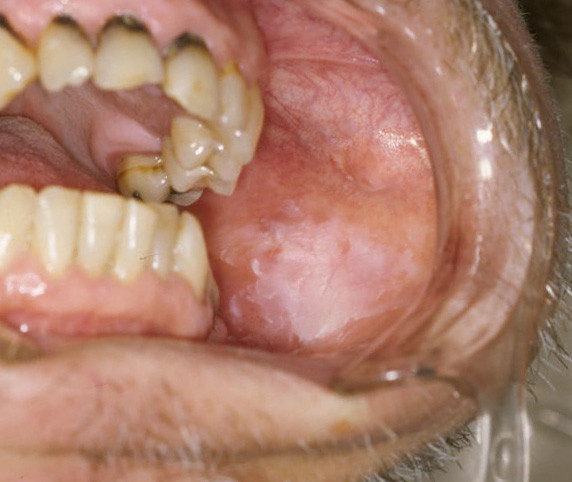
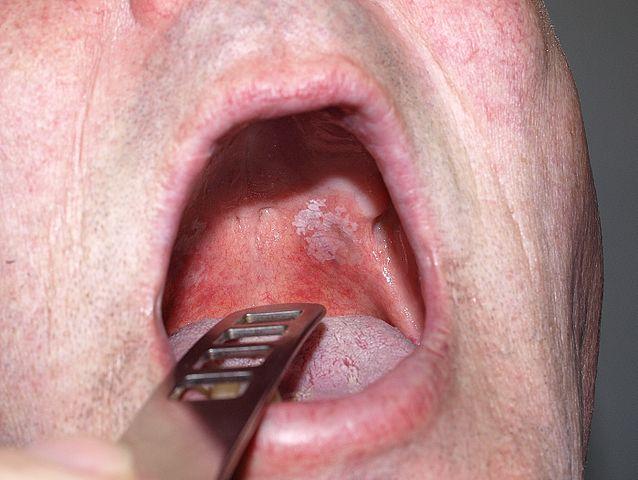
Oral Leukoplakia Pictures
The oral leukoplakia pictures are typical presentations of the condition. However, it is important to note that these lesions should be investigated further by a medical professional before reaching a diagnosis of oral leukpoplakia. Various conditions or the mouth and oral mucosa may appear in a similar manner and these pictures should not be used as a guide for self diagnosis.
Pictures of oral leukoplakia from Wikimedia Commons
Oral Leukoplakia Types
Based on their malignant potentials, clinically, there are two types of oral leukoplakia that may be observed:
- Homogenous oral leukoplakia lesions are uniformly flat and white in color with a thin appearance. These lesions less likely to be pre-cancerous.
- Non-homogenous oral leukoplakia lesions are irregular in color (white to white-red) or in texture (flat, nodular, speckled or verrucous). These lesions are more likely to be pre-cancerous.
Oral Leukoplakia Diagnosis
Typical oral leukoplakia patches are harmless and develop slowly over few weeks to months. Patches are usually painless but may be sensitive to touch, heat, spicy food or any other cause of irritation.
A biopsy test of the cells from oral leukoplakia lesion could confirm the nature of lesion and help in ruling out the possibility of oral cancer. Idiopathic oral leukoplakia lesions should be monitored carefully as they could serve as important prognostic indicator of oral cancers. Independent studies suggest that rigorous monitoring for 2-3 years, after the initial oral leukoplakia diagnosis, may be important for studying malignancy-related developments.
Oral Leukoplakia Differential Diagnosis
Oral leukoplakia plaques are clinically different from mouth lesions present in other conditions or diseases like:
- Chemical burns
- Typical mouth ulcers indicating gastrointestinal disturbances
- Other leukoplakia present during infections like candidal and syphilitic leukoplakia, including hairy leukoplakia that indicates viral infections like HIV or Epstein-Barr virus
- Congenital lesions (white-sponge nevus, dyskeratosis congenital, pachyonychia congenita)
- Common skin-related problems that present as pre-disposing conditions to cancers like keratoses, oral submucous fibrosis, lupus erythematosus or frank carcinomas.
Oral Leukoplakia Cancer Risk
Clinical criteria demonstrating a high risk of malignant transformation of oral leukoplakia patches are:
- Appearance of verrucous type of oral leukoplakia
- Formation of ulcers within the lesions
- Presence of nodules
- Lesions with hard periphery indicating abnormal maturation of epidermal cells (dysplasia)
- Lesions at the sides and under-surface of tongue and anterior floor of mouth
Oral Leukoplakia and Mouth Cancer
Oral leukoplakia is the most common type of lesion seen preceding mouth cancer. This does not mean that every person who has oral leukoplakia will develop mouth cancer. In fact, the majority of people with oral leukoplakia have benign (non-cancerous) lesions and it will not progress to a malignancy (cancer). Similarly not every person who has mouth cancer has oral leukoplakia initially.
Mouth cancer following oral leukoplakia appearance is more likely with the non-homogenous form. During the early stages of mouth cancer associated with oral leukoplakia, there may be no significant changes or alteration in appearance of the oral leukoplakia lesions. Therefore every person with oral leukoplakia should have the lesions monitored on an ongoing basis. The presence of bleeding, ulceration (open sores), protruding masses or hard masses are more likely to be associated with a malignancy (cancer). Pain may be absent in the early stages of mouth cancer.
Oral Leukoplakia Treatment
Usually removing the source of irritation offers the best treatment for oral leukoplakia.
- Repairing the dentures and rough teeth surfaces.
- Reducing tobacco and alcohol consumption.
- Beta-carotene, as oral supplement, tends to improve and accelerate healing of oral leukoplakia patches.
- Retinoids that arrest abnormal cell-growth and are potent anti-acne, could reduce progression of oral leukoplakia lesions into malignant tumors.
- Treatment of hairy leukoplakia patches requires antiviral medication.
Oral leukoplakia resolves spontaneously within a few weeks to months after removal of the cause. However, few oral leukoplakia patches need to be surgically removed. This removal is only considered when other measures to attend to the underlying cause and lifestyle changes fails to resolve the lesions. It should only be done once a diagnosis of oral leukoplakia is confirmed. In order to remove the plaque it is scraped by one of the following methods:
- Manually with a scalpel.
- Cryotherapy (freezing).
- Laser ablation.
If the following treatments fail, then ongoing assessment by an otorhinolaryngologist (ENT specialist) is advisable to consider other approaches to treating the condition as well as for ongoing monitoring to detect oral cancer as early as possible.
Prevention and Lifestyle
Oral leukoplakia cannot always be prevented. For underlying conditions like oral thrush (candidiasis), proper medical treatment of these conditions can reduce the chance of oral leukoplakia forming. Preventative measures should be targeted at lifestyle habits since these are the most likely causes or triggers of oral leukoplakia. This includes:
- Stop using all tobacco products. This includes tobacco smoking and chewing.
- Reduce alcohol intake or stop it altogether. The risk of oral leukoplakia increases in smokers who also consume alcohol.
- Seek immediate correction for poorly fitting dentures.
- Avoid repeatedly scraping the lesions with a brush or other object. It contributes to the repeated irritation of the area.
- Have regular dental checkups to ensure that new oral leukoplakia lesions are not developing as well as to monitor existing lesions.
References:
- Mouth growths. Merck Manual
- Leukoplakia. Mayo Clinic
- Oral leukoplakia. Medscape
- Carcinoma in situ of oral cavity. Dermnet NZ
Last updated on August 13, 2018.