Heart Attack Medication, Drugs to Treat a Myocardial Infarction
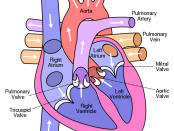
A heart attack (myocardial infarction) is death of a portion of the muscular heart wall as a result of severely reduced blood supply. It is most commonly due to a blockage in the coronary artery which supplies oxygen-rich blood to the heart wall. An occlusion that causes injury but not death to the heart wall over a period >> Read More ...