6 Signs of Parkinson’s Disease and How to Spot It
Parkinson’s disease affects about 1 in 100 Americans and is among the more commonly known neurologic disorders. About 50,000 new cases are reported every year. While there is no cure for Parkinson’s disease, early diagnosis and treatment can help slow the progression of the condition. There is no routine screening test for Parkinson’s disease and diagnosis largely rests on the signs and symptoms.
What happens in Parkinson’s disease?
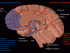
To understand the signs and symptoms of Parkinson’s disease, it is important to first understand what happens in the body and specifically within the brain. The exact cause and mechanism in Parkinson’s disease is not fully understood. In fact it appears that there may be more than one mechanism responsible for Parkinson’s disease. The loss of dopamine-producing nerves in the brain appears to be the most likely cause.
Nerves communicate with each other through chemical messengers known as neurotransmitters. One of these neurotransmitters is dopamine. In Parkinson’s disease, the dopamine-producing nerve cells die. Eventually the loss of these cells is so great that it disrupts brain activity. The area that is most affected in Parkinson’s disease is responsible for body movement.
Read more about Parkinson’s disease brain chemistry.
Therefore a characteristic presentation of Parkinson’s involves slowness of movement and involuntary movements. Parkinson’s disease progresses over years. Therefore symptoms may not be easily spotted at the outset. It is important that the signs and symptoms are evaluated by a medical professional before Parkinson’s disease is diagnosed. The presentation may sometimes vary and in the early stages it can be atypical.
How To Spot Parkinson’s Disease
Many people with early Parkinson’s disease may not have obvious signs and symptoms. In fact the only features of Parkinson’s disease may arise under specific conditions, like when stressed or when resting. It is not uncommon for close contacts, like a spouse or family members, to not spot these early signs and symptoms in a loved one. Sometimes a person with Parkinson’s disease may make a concerted effort to mask the symptoms and is able to successfully do so in the early stages of the disease.
When Parkinson’s disease is suspected it is important to immediately consult with a medical professional for a proper assessment. It is also important to note that other neurologic conditions like a stroke may be mistaken for Parkinson’s disease and vice versa. Although these are different conditions, there are common features like impaired movement and slurring of speech. It can further be missed when there is a history of substance abuse, like in alcoholism.
Read more on how strokes differ from Parkinson’s disease.
Tremors
A tremor is one of the common early signs of Parkinson’s disease. It is typically a resting tremor where the ‘shakiness’ occurs when the affected part is stationary but stops during motion. Most of the time it starts in one arm and specifically in the thumb and fingers. A back and forth rubbing motion of the thumb and forefinger is another typical tremor sign in Parkinson’s disease and is known as a pill-rolling tremor.
Tremors are not always as obvious as described. It may only be noticed when a person is undertaking activities like eating or reading a newspaper. Triggers like stress and fatigue may cause the tremors to arise and worsen. However, tremors are not present in every case of Parkinson’s disease and does not have to be present for Parkinson’s disease to be diagnosed.
Slow Movement
Slowness of movement is another major feature of Parkinson’s disease. However, it may not be present or easy to spot in the early stages of the disease. This slowness of movement is known as bradykinesia. It develops gradually over a long period of time and the presentation varies among Parkinson’s disease patients. Some patients also report it as muscle weakness.
The problem is often with initiating movement and reaches a point where there is a generalized slowness in activities, even blinking and speaking. This may be seen as a slowness when waking from a chair, moving the feet when walking resulting in the feet being dragged, blinking less often than normal and great effort to write, hold a utensil to eat or turn a key or door knob.
Stiff Muscles
Muscle stiffness or rigidity is another feature of Parkinson’s disease but it is not present in every case. Sometimes bradykinesia is mistaken for rigidity. The muscle stiffness limits movement or flexibility and there may be cramping that can be painful. This stiffness is not isolated to the arms or where tremors are more prominent. Rigidity can affect any part of the body.
Posture and Balance Problems
Stooping is another sign of Parkinson’s disease but may not be seen until bradykinesia (slow movement) and rigidity (muscle stiffness) become pronounced. It usually occurs when the disease has advanced significantly. Poor balance is another sign of Parkinson’s disease. It is more likely to be due to the bradykinesia, rigidityand loss of reflexes. This impairs the ability to move and use muscles as normal to maintain an upright posture and move with stability.
Change in Gait
The way a person moves (gait) changes over time in Parkinson’s disease. This varies from shuffling steps when walking and the slowness of movement that is characteristic of all motor activities in Parkinson’s disease. One or both arms may also not swing as normal when walking. Eventually in some patients and specifically in extreme cases there is a complete inability to move. There is difficulty in starting movement and even stopping movement once it starts.
Altered Speech
Due to the difficulty with initiating movement as well as the slowness of muscle activity, speech is often affected in Parkinson’s disease. This can vary from problems with starting to talk (often seen as hesitation) to a softness of the voice, monotone voice and slurring of speech. Words may not be formed properly and there may be difficulty in understanding the person’s speech. Drooling may also occur simultaneously but usually in later stages of the disease.