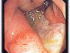
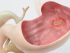
Acid Ulcers (Open Sores) – Causes, Location, Symptoms and Treatment
Ulcers are open sores that can form on the surface of the body as well as internally. One of the common sites of ulcers within the body is the digestive tract. Although these ulcers can form anywhere along the digestive tract, it is more likely to occur in the esophagus, stomach and the first part of the small intestine known as the duodenum. There are many reasons why ulcers may arise but acid is one of the common causes for these open sores in the gut.
What are acid ulcers?
Acid ulcers is a common way to describe open sores that form due to acidity. The stomach produces a highly corrosive acid (hydrochloric acid or HCl) which is needed for digestion. However, this HCl can also digest human tissue. While the digestive tract does have several mechanisms to contend with the HCl, either by withstanding its effects or neutralizing it, the tissue can become damaged if these mechanisms fail or are inadequate.
Ulcers can also arise in the digestive tract for other reasons. For example there may be ulcers in the colon with in inflammatory bowel disease (IBD). This ulceration is due to autoimmune factors where the body’s immune system targets the colon wall and causes inflammation. Therefore ulcers in these conditions are technically not acid ulcers.
Location and Causes of Acid Ulcers
Ulcers that arise from the action of stomach acid are more likely to occur in three possible locations:
- Esophagus (food pipe)
- Stomach
- Duodenum (first part of the small intestine)
Most of the time stomach and duodenual ulcers arise for the same reasons,usually H.pylori infection and excessive use of NSAIDs. Esophageal ulcers on the other hand are more likely to occur due to gastroesophageal reflux disease (GERD), which is commonly referred to acid reflux.
Esophagus
Stomach acid or any of its contents should not enter the esophagus. The LES (lower esophageal sphincter) ensures that the stomach contents do not flow backward. It only opens when food and fluids have to pass down the esophagus into the stomach. However, LES dysfunction is a common problem and the main reason for a GERD (acid reflux). This allows stomach acid and enzymes to enter the esophagus.
The esophagus does not have adequate mechanisms to deal with the acid. Large amounts of saliva are released (water brash). This saliva is swallowed in the attempt to neutralize some of the acid in the esophagus. In addition strong contractions in the wall of the esophagus attempt to push the acid downwards back into the stomach. For minor reflux, these mechanisms are sufficient.
However, chronic GERD is a common problem and this means that the esophagus is repeatedly exposed to stomach acid. It damages the esophagus thereby causing inflammation of the esophageal wall (esophagitis) and eventually ulceration.
Stomach
The stomach is well suited to handle the hydrochloric acid (HCl) as the stomach wall is constantly exposed to it. Cells in the stomach wall produce copious amounts of mucus. This lines the inner wall of the stomach. The mucus barrier prevents the acid from making contact and damaging the stomach wall tissue, which can lead to stomach inflammation (gastritis) and stomach ulcers.
Two common factors that compromise the mucus barrier, thereby exposing the stomach tissue to the acid, are H.pylori bacteria and excessive use of NSAIDs.
- Helicobacter pylori can withstand the stomach acid by secreting substances that neutralize the acid immediately around it. It then burrows into the stomach wall, damaging it in the process. This action compromises the stomach’s mucus barrier.
- NSAIDs are commonly used drugs. While it is intended to counteract inflammation, some of the active ingredients with NSAIDs also impairs the stomach ability to produce mucus. As a result the mucus barrier is significantly weakened.
Read more about stomach ulcers.
Duodenum
The duodenum (first part of the small intestine connected to the stomach) is constantly exposed to small amounts of gastric chyme, especially after eating. However, the duodenum has its own mechanisms to deal with the acid. Water and alkali substances like bicarbonate are pumped into the duodenum to weaken and neutralize the acid. Mucus also coats the duodenal wall to protect the underlying tissue
Ulcers in the duodenum occurs for the same reasons as stomach ulcers such as infection with the H.pylori bacteria. In addition, there is increased stomach acid secretion and reduced bicarbonate secretion in the duodenum with H.pylori infection. This further raises the risk of ulcers forming in the duodenum. Overall duodenal ulcers are more common than stomach ulcers.
It is not uncommon for duodenual and stomach ulcers to occur simultaneously. Collectively ulcers in these parts of the gut are referred to as peptic ulcer disease.
Signs and Symptoms
The signs and symptoms may be similar among the differen types of acid ulcers. In the early stages there may be minor non-specific symptoms, especially if the uclers are small.
- Dull gnawing ache to burning pain in the lower part of the chest (esophageal ulcers), upper left region of the abdomen (stomach) and upper middle region (duodenal ulcers). Heartburn may also be experienced.
- Nausea and sometimes vomiting. Vomitus that has visible blood or ‘coffee ground’ appearance (degraded blood) usually indicates a bleeding ulcer.
- Bloating sensation – feeling of fullness. It may arise after a few bites of food or persist even without eating. It is also often accompanied by excessive belching.
- Changes in appetite, either an increased or decreased appetite. A person with peptic ulcers may also experience intolerance to fatty foods.
- Sleeping problems which may be due to the aggravation of symptoms in the early parts of the morning when the stomach acid secretion increases.
Read more on signs of ulcers.
Treatment of Acid Ulcers
The treatment of acid ulcers requires a combination of dietary and lifestyle changes alongside medication. The main drugs used for acid ulcers work by making the stomach acid less acidic or suppressing the acid-producing cells in the stomach wall to reduce the quantity of gastric acid that is produced.
- Antacids are alkalis that neutralize the stomach acid.
- Acid-suppressing drugs like proton pump inhibitors (PPIs) and H2-blockers reduce stomach acid production.
- Cytoprotective drugs stimulate mucus production thereby coating the stomach wall until it heals.
- Antibiotics are prescribed to eradicate the H.pylori bacteria.
- Prokinetic drugs may sometimes be used for acid reflux to speed up emptying of the stomach.